The case
A 32-year-old male runner visits his family physician in late spring complaining of pain in his knees over the past month. The pain is mostly anterior but is not well localized. It is aggravated by running, especially on hills, but subsides after the patient stops running. The patient has kept fit during the winter by swimming and occasional cross-country skiing. He has no history of obvious trauma or a noticeable injury.
Anterior knee pain (AKP), that is, pain localizing to the anterior region of the knee, is the most common knee problem seen by family physicians.1 Although the potential causes are numerous, most cases can be diagnosed without extensive radiologic investigations through careful history-taking and physical examination. Few randomized controlled trials have evaluated treatments for benign knee disorders; however, most patients will respond to some combination of analgesics, application of heat or ice, strength and flexibility exercises, orthotics, bracing and taping, or wearing more suitable shoes.
Cause
The appropriate combination of treatments will depend on the underlying cause. The vast majority of cases of AKP are caused by trauma superimposed on a predisposing anatomical malalignment (Table 1). The trauma may be acute but is more frequently the result of repetitive overuse.1 Training errors (usually too much exercise too soon), malalignment of the hip or the extensor mechanism including the patella and the feet, deficiencies in strength and flexibility, ill-fitting shoes and uneven training surfaces are the most common problems that contribute to AKP.
Table 1.
Although physical examination may reveal abnormalities of structures within the knee joint, in approximately 5% of patients with AKP the pain is referred from a source outside the knee. For example, the diagnosis of slipped capital femoral epiphysis is frequently made when adolescents first present to their family physician with the complaint of knee pain.
History
The history provides essential clues to the diagnosis. In most cases, careful questioning of the patient can elicit information about precipitating factors, such as changes in training surfaces (including road camber), exercise intensity (including hill and weight training), shoes and equipment (Table 2). Information about previous episodes, injuries, surgeries, medical conditions, medications and treatment to date is essential. One should also enquire about a history of knee grinding, locking and giving way, night pain, relieving and aggravating factors, systemic symptoms and the involvement of other joints.
Table 2.
In most cases, the history allows one to distinguish malalignment and overuse from traumatic causes. In cases of trauma, the onset of pain is usually sudden, whereas with malalignment and training errors, the onset is gradual and the course progressive. Patients with pain due to malalignment or training errors may also note that the pain is aggravated by running up or down hills and stairs, or by holding the knee in a flexed position such as at the theatre or in an airplane. These patients may state that they usually request an aisle seat (the “theatre sign”).
Physical examination
This discussion assumes that the reader is comfortable using the standard knee examination to assess the major structures within the knee, namely, the menisci, ligaments and bony surfaces, using the “look, feel and move” approach (Table 3). If there is an effusion present or any clinical concern exists for pathology of the intra-articular structures, these should be referred to a specialist or treated appropriately if it falls within the reader's own area of expertise.
Table 3.
The patient should be asked to wear shorts during the examination because both knees and feet should be fully exposed. The patient should also bring along a used pair of exercise shoes. The physician should check their suitability for the patient's foot type and described activity. For example, “stability” shoes may not provide sufficient support for individuals with severe pronation. Excessive or uneven wear or collapse of the midsole will help the physician identify problems.
Stance, alignment and gait
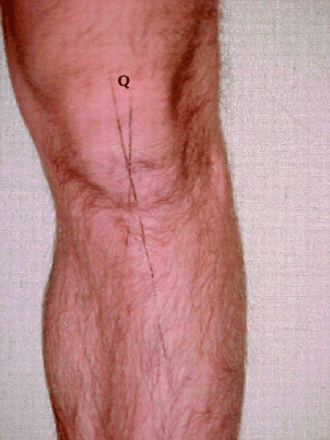
As the patient stands barefoot facing the physician, the physician should check the alignment of the patellae and should look for angular abnormalities. An increased quadriceps angle (Fig. 1)2 (10ο in males and 15ο in females) will cause the patella to track laterally in the trochlea, with flexion resulting in abnormal facet stresses.
Fig. 1: Quadriceps (Q) angle is the angle between the line of the femur and the line of the patellar tendon. 2
The feet should be observed for excessive hind foot pronation, namely, the foot appears to collapse inward with weight bearing. This can be done by asking the patient to stand on his or her toes and observing, from behind, the rigidity of the pronation (if supple, the hind foot will invert or tilt inward at this stage). The shoes of a patient with hind foot pronation will show excessive lateral heel wear and medial collapse of the heel counter (supporting structures of the heel) compared with the rest of the shoe.
The combination of excessive femoral anteversion (i.e., “squinting” inward) and external tibal torsion (turning outward) is known as miserable malalignment syndrome. (With the feet parallel, the patellae will point inward.)
The patient should be observed from the front and rear as he or she walks in a straight line. Look for any pelvic “rocking” or asymmetry in the gait, which may indicate a leg-length discrepancy (leg lengths should be measured from the anterior superior iliac spine to the medial malleolus). An antalgic gait on flat ground may indicate significant internal knee pathology.3 Tracking of the patella in the trochlea should also be assessed.
Mobility and flexibility
The knee should be observed with the patient sitting on the edge of the examination table with the knees flexed to 90°. As the patient actively extends and flexes the knee, observe the tracking of the patella throughout the range of movement and feel for any crepitus. The patella normally sits in the middle of the knee, but in patients with AKP it may be high or to one side. Both lateral and proximal displacements of the patella are predisposing factors for AKP.
It is essential to compare crepitus in both knees, because it is commonly present without pain. If the crepitus is more marked in the symptomatic knee, this may signify articular cartilage damage. However, articular cartilage damage alone is not a cause of pain, because there are no nerve endings within this cartilage.4 Cadaveric studies5 have revealed patellar chondral lesions in 40%–60% of the population.
With the patient supine and the knee extended, assess the patella for lateral mobility by attempting to displace the patella medially. The extent of movement is normally one-quarter to three-quarters of patellar width. Less movement suggests a tight lateral retinaculum, which is a predisposing factor for lateral tracking or patellar subluxation, or both; patients with greater than normal movement may have a history of patellar subluxation or dislocation and may display apprehension during this test (“positive apprehension sign”).
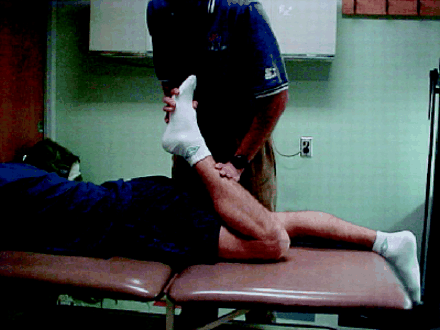
Still lying supine, the patient should be asked to flex the hip to 90° and extend the knee. It should be possible to extend the knee fully in this position; however, extension is commonly restricted in runners who do not stretch regularly (Fig. 2). Dancers and athletes who practise sports such as gymnastics are often able to flex the hip to 160ο, and limitation to the “population norm” of 110ο may reflect restriction specifically in such individuals.
Fig. 2: Measuring hamstring tightness. 1
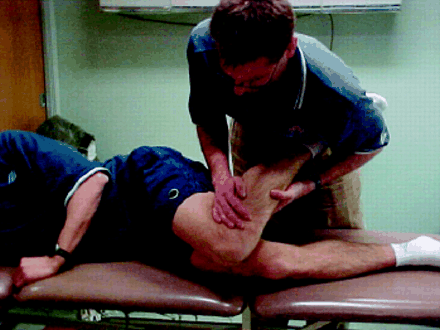
Lying supine with the hips flexed, patients should be able to bring their heels up against their buttocks. The physician should repeat this assessment of quadriceps flexibility with the patient in the prone position (Fig. 3), comparing both sides and watching for involuntary hip extension, pelvic lifting or tightness.
Fig. 3: Measuring quadriceps flexibility. 1
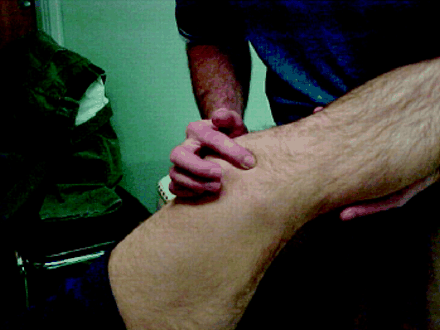
Heel cord flexibility is measured with the patient in the supine position with the knee fully extended. He or she should be able to dorsiflex (upward) the ankle 15° beyond the neutral (90°) position (Fig. 4).
Fig. 4: Measuring heel cord tightness. 1
In Ober's test for iliotibial tightness, the patient lies on his or her side with the affected leg on top and flexes the lower hip and knee to 90° on the table. Standing behind the patient, the physician holds the pelvis steady with one hand and uses the other hand to flex the knee of the upper leg to 90° and fully extend the hip. The leg is then lowered toward the table; in normal flexibility, the knee should come close to the surface of the table (Fig. 5).
Fig. 5: Ober's test for iliotibial band tightness. 1
Muscle bulk and strength
Muscle bulk should be measured for the major muscle groups in both legs. For accuracy and follow-up, it is useful to measure diameters at specific levels.6 The vastus medialis obliquus (VMO) muscle is of particular importance in AKP. Assess its bulk bilaterally by having the patient extend the knee to 45° while sitting. Wasting of this muscle may be a cause or a result of AKP and will result in abnormal tracking of the patella.
As the patient, in a supine position, contracts the quadriceps, the VMO and vastus lateralis should contract simultaneously; however, with ongoing AKP, the VMO will often be seen to contract later.4 Demonstrating this to patients often motivates them to adhere to a rehabilitation program and assists in biofeedback therapy.
Tenderness
The entire extensor mechanism should be assessed for tenderness. Palpation of the quadriceps insertion (VMO, rectus femoris and vastus lateralis) and its musculotendinous structures should be carried out with the muscle both relaxed and contracted to avoid missing any partial tears that would be readily palpable during contraction.
Palpate the lateral retinaculum and the patellar tendon along its whole length. In patellar tendinitis (jumper's or runner's knee), there is often point tenderness on the inferior patellar border. Swelling and tenderness of the tibial tuberosity is commonly found in Osgood-Schlatter disease (a traction apophysitis of the distal patellar tendon common in teenage athletes).
The medial patellar border is often tender in AKP. Whether this is due to the soft tissue or the patellar facets should be determined by palpating along the medial border with the patient's knee flexed to 30°–90° and feeling for a thickened or tender medial plica running vertically along this border (Fig. 6). The patient may also feel a painful popping sensation, recreating his or her symptoms, as the plica is palpated. This condition may account for 10%–15% of patients presenting with AKP to a sports medicine practice.
Fig. 6: Palpation for synovial plica. 1
Compress the patella into the trochlea while flexing the knee through its full range. Lesions of the subchondral bone will cause tenderness as they are brought into articulation. The distal patellar facets articulate first from about 15° of flexion; then, as the knee is flexed further, the proximal facets come into contact.7 This test will allow better localization of lesions and the site for radiography, if needed.
Point tenderness over the patellar body may indicate prepatellar bursitis (housemaid's knee) or a patella stress fracture.
Within and beyond the knee
A complete assessment of the internal structures of the knee (including the menisci, ligaments and bony surfaces) is necessary, but description of this is beyond the scope of this article. The presence of disruption of these structures, the presence of a significant effusion or hemarthroses, or a history of patellar dislocation would require referral to a specialist. In addition, any pathology of the hip, spine and femur may present as AKP and must be considered in the diagnosis.
Further investigations
Not all patients will require radiographic investigation. If x-ray films are necessary (with suspicion of osteochondral fractures, significant osteoarthritis or unexplained night pain), these should include an anteroposterior view and a lateral view of the knee at 90° of flexion. Patellar (or infrapatellar) views at 30°–45° of flexion are helpful to assess positioning of the patellae in the trochlea and may reveal osteochondral lesions or avulsion fractures of the medial patellar border, as seen in recurrent patellar dislocation.
Further radiologic investigations, such as CT and MRI, are not usually indicated unless the patient fails to respond to a full course of nonoperative therapy.
Treatment
Both the physician and the patient must realize that in order to prevent repeated injury, the ultimate goal of therapy is to surpass the preinjury level of conditioning, which was not sufficient to prevent the initial injury, and to improve the malalignment that was present when the symptoms occurred. Treatment should be directed by the clinical findings and should involve a combination of methods.
Analgesics
Analgesics including nonsteroidal anti-inflammatory drugs (oral and topical) play an important role in therapy but should never be the only form of treatment.
Ice and heat
Ice is essential during the acute phase of injury and is also useful after exercising. Ice therapy causes capillary vasoconstriction with decreased blood flow and decreased metabolic activity.8 The resulting decreased inflammatory edema and hemorrage will prevent further damage and will provide analgesia. The local application of ice and massage has been shown to provide greater temperature reduction and analgesia than the simple application of an ice pack. This is easily done at home by massaging the affected area with an ice cube. Patients should be warned to avoid application that lasts longer than 20 minutes, because this has been shown to cause injury to the skin and to underlying superficial structures such as nerves.8,9
Heat application causes increased capillary blood pressure and increased cellular permeability, with resultant increased swelling and edema. Heat should thus be used after the initial postinjury swelling and edema have stabilized (about 24–48 hours post injury). The effect of heat is to increase blood flow and local metabolic activity with relaxation of muscle spasm.8
The application of heat has been used in conjunction with ice to increase flexibility in stiff joints (i.e., contrasting hot and cold baths or packs). Alternating vasoconstriction and dilation with analgesia has been proven to be effective in increasing joint range of motion.9
Muscle strengthening
Quadriceps strengthening, especially of the VMO, usually forms the basis of therapy for AKP and many programs, both simple and complex, exist for this purpose. One of the most effective (and simplest) is an eccentric quadriceps exercise known colloquially as the “drop squat” program, in which the patient starts in a standing position and drops to a half-squat (or 45°), with the kneecap over the second toe. This takes less than 2 minutes to demonstrate in the office and may easily be done by the patient at home as 3 sets of 20 repetitions per day. Over 6–8 weeks, the patient may progress to using hand-held weights and a balance board.
Flexibility
Stretching should be carried out in conjunction with strengthening exercises. If a specific muscle group is restricted, more emphasis may be placed on these areas but there must be stretching of all the major muscle groups of the lower limb, because they all have an effect on the biomechanics of the knee. Patients should be instructed to hold a stretch for 20–30 seconds for it to be effective.10
Orthoses and shoes
If there is an obvious problem with pronation (midfoot pronation with hind foot valgus), orthotics may be necessary.4 Patients should usually be advised to undergo physiotherapy or active rehabilitation first, and footwear should be assessed before recommending prescription orthotics.
Patients should be advised about the types of shoes recommended for their particular gait or alignment and sporting activity. They should be instructed to check regularly for early signs of wear in the midsole and to replace shoes before the supporting structures collapse. For patients with pronation, a stiffer motion-control or stability shoe with medial support is indicated; for those with more rigid pes cavus feet, a more cushioned, shock-absorbing shoe is best. The most expensive shoe is not necessarily the best one for a particular patient. For stability or motion control, we look for a firm heel cup with supportive medial midsole cushioning (this may include gels or supportive structures, e.g., bridges) and torsional rigidity. (A local running equipment store is a good source of advice on shoes.)
Taping and bracing
Taping helps in the realignment of the patella, it may aid in stretching a tight lateral retinaculum, and it may rest irritated soft tissues by altering tissue tensions. It is an important adjunct to the rehabilitation program and may allow some patients to partake in sports without pain. Patellar braces are more convenient and may have similar effects. It is important that the brace be used in conjunction with the rest of the rehabilitation program as an adjunct, while attempting to correct the underlying malalignment and biomechanic problems, as discussed above.
Surgery
Surgery is occasionally necessary in patients with severe osteochondral lesions or when the problem is unresponsive after 4–6 months of conservative treatment.5,11 Such cases should be referred to a specialist for further assessment but may include a possible lateral retinacular release or arthroscopic debridement.
Treating our patient
Our patient had a Q angle of 20°, a very tender inferior patellar pole and tight hamstrings and gastrocnemii. He also exhibited marked hind foot pronation, for which he had recently bought a new pair of suitable stabilizing running shoes. A diagnosis of inferior patellar tendinosis was made. Treatment included reducing running mileage by 50%, followed by a gradual increase of 10% per week; avoidance of hill training; starting the “drop squat” program to strengthen his quadriceps; icing the lower patellar pole; and stretching his iliotibial band, gastrocnemii, hamstrings and quadriceps.
When the patient returned for follow-up about 6 weeks later, his problem was much improved, but his pronation was not being controlled by the running shoes. The patient was referred for orthoses and has been doing well since.
Key points
-
Anterior knee pain (AKP) is the most common knee problem seen by family physicians.
-
Although the causes are numerous, most cases can be diagnosed through careful history-taking and physical examination and treated with a combination of analgesics, physiotherapy and behaviour modification.
-
Most cases of AKP are caused by trauma when there is a predisposing anatomical malalignment.
-
The physician should question the patient about changes in exercise intensity and methods; previous injuries, conditions and treatment; and a history of pain, relieving and aggravating factors, systemic symptoms and the involvement of other joints.
-
For the physical examination, the patient should wear shorts and should bring along a pair of used exercise shoes.
-
The physician will assess the patient's stance, alignment and gait from a variety of perspectives; mobility and flexibility; muscle bulk and strength; and tenderness.
-
Any pathology of the hip, spine and femur should be identified because it may appear as AKP; suspected disruption of the internal structures of the knee requires referral to a specialist.
-
Although analgesics play an important role in therapy, they should never be the only form of treatment.
-
Ice is essential during the acute phase of injury to decrease swelling and edema; later, heat can be applied to increase blood flow and local metabolic activity and to relax muscle spasm.
-
Muscle strengthening and stretching will form an important part of therapy.
-
Patients should seek advice about the types of shoes recommended for their particular gait or alignment and sporting activity. They should check the shoes regularly for early signs of wear and replace shoes before the supporting structures collapse.
-
Taping or bracing helps realignment and rests irritated soft tissues, but these should be used as an adjunct to a rehabilitation program that addresses the underlying malalignment and biomechanic problems.
-
Surgery is occasionally necessary in patients with severe osteochondral lesions or when a problem is unresponsive after 4–6 months of conservative treatment.
Articles to date in the rheumatology series
-
Esdaile JM. Rheumatology: introduction to the series. CMAJ 2000;162(7):1007.
-
Ensworth S. Rheumatology: 1. Is it arthritis? CMAJ 2000; 162 (7): 1011-6.
-
Shojania K. Rheumatology: 2. What laboratory tests are needed? CMAJ 2000;162(8):1157-63.
-
Reid G, Esdaile JM. Rheumatology: 3. Getting the most out of radiology. CMAJ 2000;162(9):1318-25.
-
Cibere J. Rheumatology: 4. Acute monoarthritis. CMAJ 2000; 162(11):1577-83.
-
Klinkhoff A. Rheumatology: 5. Diagnosis and management of inflammatory polyarthritis. CMAJ 2000;162 (13): 1833-8.
-
Price GE. Rheumatology: 6. Localized therapy. CMAJ 2000; 163(2):176-83.
-
Huang SHK. Rheumatology: 7. Basics of therapy. CMAJ 2000; 163(4):417-23.
-
Lacaille D. Rheumatology: 8. Advanced therapy. CMAJ 2000; 163(6):721-8.
-
Clark BM. Rheumatology: 9. Physical and occupational therapy in the management of arthitis. CMAJ 2000; 163 (8):999-1005.
-
Brady OH, Masri BA, Garbuz DS, Duncan CP. Rheumatology: 10. Joint replacement of the hip and knee — when to refer and what to expect. CMAJ 2000;163(10):1285-91.
-
Puttick MPE. Rheumatology: 11. Evaluation of the patient with pain all over. CMAJ 2001;164(2):223-7.
-
Tsang I. Rheumatology: 12. Pain in the neck. CMAJ 2001;164 (8): 1182-7.
-
Wing PC. Rheumatology: 13. Minimizing disability in patients with low-back pain. CMAJ 2001;164(10):1459-68.
Footnotes
-
This series has been reviewed and endorsed by the Canadian Rheumatology Association.
The Arthritis Society salutes CMAJ for its extensive series of articles on arthritis. The Society believes that this kind of information is crucial to educating physicians about this devastating disease.
This article has been peer reviewed.
Contributors: Dr. Wilkinson was the principal author of the manuscript. Dr. Taunton was responsible for manuscript review, correction and advice.
Competing interests: None declared.
Reprint requests to: Dr. Jack E. Taunton, Allan McGavin Sports Medicine Centre, 3055 Wesbrook Mall, Vancouver BC V6T 1Z3; fax 604 822-3614; [email protected]
Series editor: Dr. John M. Esdaile