In 1993 the World Health Organization declared tuberculosis a global emergency. The tubercle bacillus infects one-third of the world's population. It is the most common single agent causing death in young adults and causes 2 million deaths each year around the world.1 Although tuberculosis is common in many parts of the world, Canada enjoys one of the lowest prevalence rates, 7 per 100 000 population.2 The average family physician in Canada can expect to see only 1 active case in every 10 years of practice.3 This lack of familiarity with the disease may contribute to the delay in diagnosis of atypical presentations, particularly extrapulmonary tuberculosis. We present a case highlighting the diagnostic difficulties that bone and joint tuberculosis poses for clinicians as well as the barriers to appropriate assessment and treatment that marginalized people face in our health care system.
Case report
A 40-year-old man living in an inner-city shelter was seen in September 2000 by an outreach nurse practitioner regarding a painful, swollen right knee. He had noticed a small, tender lump on the side of his knee in June. He had visited a walk-in clinic for this problem in July and had been prescribed an NSAID. This treatment initially attenuated his pain but did nothing to stop the swelling in the knee, which grew to involve the entire joint. Over the next 2 months his knee became increasingly painful. He returned to the walk-in clinic in October and was referred to a local hospital emergency department for evaluation of suspected septic arthritis.
In the emergency department he was noted to have a moderate effusion of the right knee and a large swelling in the popliteal fossa. He was afebrile. A total of 40 mL of straw-coloured fluid was removed from the swollen joint and sent for Gram staining, culture and microscopy. Culture yielded negative results, and no crystals were seen. Culture for acid-fast bacilli was not requested. Radiography was not ordered. The patient left against medical advice several hours later.
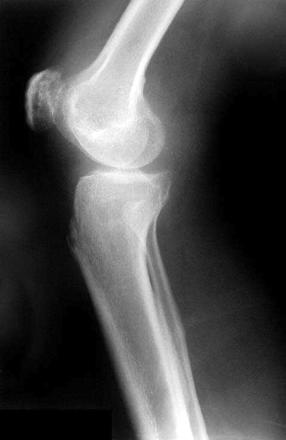
He returned to the walk-in clinic in November for wound care to a nonhealing, weeping lesion that had developed over the lump in the popliteal fossa, which he attributed to the aspiration procedure done at the hospital emergency department. He was told to return for daily dressing changes and was given a course of cloxacillin for suspected cellulitis. This had no effect on the wound. He was sent again for evaluation to the emergency department in December. Radiography done at this visit reported only on the presence of a small suprapatellar effusion (Fig. 1). Aspiration of the joint fluid was performed. Culture of the fluid showed no growth after 5 days. Gram staining revealed no bacteria, and no crystals were seen on microscopy. Culture for acid-fast bacilli was not requested. A complete blood count showed a hemoglobin concentration of 97 g/L (normally 130–170 g/L) and a normal leukocyte count. The erythrocyte sedimentation rate was elevated, at 133 mm/h (normally < 9 mm/h). The serum creatinine and electrolyte levels were within normal limits. Once again, the man left against medical advice.
Fig. 1: Radiograph, showing small suprapatellar effusion in right knee of man later found to have osteoarticular tuberculosis.
He was subsequently referred to a community health centre by the nurse practitioner he had seen initially at the shelter in September because she was concerned by the lack of a diagnosis. The man had come to Canada from Ethiopia in the late 1980s. He had no known exposure to tuberculosis but had been homeless for several years. He had received bacillus Calmette–Guérin vaccine as a child. He recalled that he had had a “negative” Mantoux test result in 1996 and chest radiography in 1989 and 1990, which he had been told gave normal results. He denied any intravenous drug use or HIV risk factors. There was no history of antecedent injury to his knee. He reported a weight loss of about 15 kg since 1996. He denied cough, fever, anorexia or night sweats.
On physical examination the patient was cachectic but showed no other signs of pulmonary tuberculosis. He was afebrile. His lungs were clear to auscultation. There was neither lymphadenopathy nor organomegaly. His right knee was extremely swollen. There was marked wasting of the quadriceps muscles, and he was unable to fully extend the knee. Flexion was also severely limited. An ulcerative lesion measuring about 3 cm by 4 cm on the posterolateral aspect of the right knee joint continuously oozed a thin, milky liquid. The lesion appeared to be connected to the joint itself because pressure on the joint directly increased the drainage from the lesion.
A Mantoux test gave a positive result (21 mm of induration). Specimens from the lesion as well as sputum samples were sent for culture for acid-fast bacilli. A chest radiograph was interpreted as normal. An HIV test gave a negative result. The public health department was informed of the positive tuberculosis skin test result and of the suspicion of tuberculous arthritis. A referral was arranged to a local hospital's tuberculosis clinic, and a decision was made to start antitubercular treatment with isoniazid, rifampin, pyrazinamide and ethambutol pending the culture results and before the clinic appointment, several weeks away. The public health department arranged directly observed therapy. Culture of the fluid from the lesion yielded fully sensitive Mycobacterium tuberculosis. Sputum samples were smear-negative; however, they subsequently grew M. tuberculosis complex on culture.
The patient completed 4 months of a proposed year-long course of therapy, and his knee improved somewhat; however, his compliance with treatment was hampered by mental illness, poverty and homelessness. Fortunately, he voluntarily admitted himself to the tuberculosis service of a local chronic care hospital, where compliance could be assured. He stayed at the hospital for over 2 months. During his stay he received aggressive physiotherapy and was ambulating well, with decreased pain and swelling in the knee on discharge. At the time of writing, he was continuing to follow up as an outpatient at the tuberculosis clinic and was scheduled to see an orthopedic surgeon.
Comments
Tuberculosis is typically classified as pulmonary or extrapulmonary. In Canada 60% of cases are pulmonary, and of the remainder about 7% involve bone or joints or both.2 Half of all musculoskeletal cases involve the spine.4,5,6 Tuberculous arthritis is usually monoarthritis with a predilection for weight-bearing joints;7 however, up to 15% of cases are polyarticular.8 Culture of synovial fluid gives positive results in 79% of cases,2 but synovial biopsy may be required to grow the organism.6 In some cases the organism will not be seen on smear or culture, but caseating granulomas will be demonstrated on histologic examination.9,10,11 For this reason histologic studies must be performed in cases in which microbiologic tests give negative results in order to confidently exclude tuberculosis as a cause of chronic arthritis. In our case, culture of the joint fluid confirmed the diagnosis, and histologic studies were not necessary. A positive Mantoux test result can be helpful in confirming a suspicion of tuberculosis, but a negative result cannot rule it out. In one case series the rate of false-negative results of the Mantoux test was 14%.9
Musculoskeletal tuberculosis arises from hematogenous seeding of the bacilli soon after the initial pulmonary infection. Osteoarticular tuberculosis usually starts as osteomyelitis in the growth plates of bones, where the blood supply is best, and then spreads locally into the joint spaces.12 The diagnosis of osteoarticular tuberculosis is often delayed, on average by 16 to 19 months,10 and may be delayed up to 10 years.11 The most consistent clinical symptoms are insidious onset, pain, swelling of the joint and limited range of motion.13 In about 30% of cases there is a discharging sinus or fluctuation.11 In one case series 31.5% of patients with musculoskeletal tuberculosis had no systemic symptoms.11 Radiographic changes in the joint are absent or nonspecific early on, but soft-tissue swelling with little periosteal reaction, osteopenia, narrowing of the joint space (a late finding) and subchondral erosions of both sides of the joint suggest tuberculosis.6 MRI imaging has become the preferred imaging technique for spinal tuberculosis because it can differentiate between granulation tissue and abscess, identify soft-tissue masses and assess the degree of bone destruction; however, bone anatomy and abnormalities, including macroscopic calcifications (rice bodies) and sequestra, are better seen on CT scanning.5,14,15 Chest radiographs may show evidence of pulmonary disease in 50% of patients with osteoarticular tuberculosis, but active pulmonary disease is present in fewer than 1 in 5.7 In 10% to 25% of cases of osteoarticular tuberculosis definitive diagnosis remains elusive.7
The colony counts in joint tuberculosis are 1000 times lower than in pulmonary disease.7 Consequently, the risk of transmission of osteoarticular infection is extremely low, with only a few reports of contagion arising from aerosolization of abscess material, presumably from wound irrigation.16 M. tuberculosis does not grow on ordinary culture medium, and it has a slow growth rate, so that several weeks may be needed for colonies to become visible.6 When tuberculosis is suspected, the public health laboratory should be contacted early on. In addition to providing advice on specimen collection and minimizing the risks of contagion, the public health laboratory can expedite the culture results in selected cases using a nucleic acid amplification test. This test can return a positive result within hours to days after specimen arrival versus 2 to 8 weeks with conventional culture methods.17
Our case demonstrates many of the pitfalls around diagnosing osteoarticular tuberculosis. People with extrapulmonary tuberculosis often do not have the classic symptoms associated with pulmonary disease, such as fever, cough, weight loss, anorexia and night sweats. Nor do they exhibit physical findings associated with pulmonary disease. In fact, even in relatively advanced pulmonary disease the findings on physical examination are frequently normal.2 In bone and joint tuberculosis radiographs are typically unhelpful in suggesting the diagnosis, especially in the early stages. Chest radiographs may be often interpreted as normal in patients subsequently found to have coexisting active pulmonary disease, as in our case. It is important to realize the limitations of radiography and to understand that so-called “normal” findings do not rule out disease.
First and foremost one must consider tuberculosis as a diagnostic possibility. Any case of acute arthritis is septic until proven otherwise, and any case of chronic arthritis ought to raise the suspicion of tuberculosis, particularly in a person from an endemic region. A history of exposure and risk factors for tuberculosis should be explored, and a Mantoux test should be performed at a minimum. Since tuberculosis can affect several organ systems, it is crucial to look for it at other sites. Most important, from a public health perspective, concomitant pulmonary involvement must be searched for. Tuberculosis should be considered in patients from high-risk groups, including Aboriginal people, immigrants from countries with a high prevalence of tuberculosis (Table 1), poor and homeless people from the inner city, elderly people and people with illnesses such as HIV infection, chronic renal failure, silicosis and diabetes mellitus. Furthermore, there is an important opportunity for primary health care providers to screen high-risk groups for tuberculosis and offer isoniazid prophylaxis to those found to have latent infection. In this way a sizeable proportion of active disease cases could be prevented.18,19
Table 1.
Finally, as our case illustrates, certain people are at increased risk because they are unable to gain access to health care services effectively. Mental health problems, absence of social supports and a lack of stable housing contribute to uncoordinated care, diagnostic delay and increased morbidity to the individual and threats to public health in general. Clearly, had it not been for the existence of street outreach programs designed to help marginalized people obtain access to services and continuity of care, our patient's diagnosis would have been further delayed.
Footnotes
-
This article has been peer reviewed.
Contributors: Dr. Payne conceived the article, performed the literature review and wrote and revised the manuscript. Dr. Yang contributed to the follow-up of the patient and critically revised the manuscript.
Acknowledgement: We acknowledge the clinical acumen of the outreach nurse practitioner, Catherine Simpson, who first considered the diagnostic possibility of tuberculosis in this case.
Competing interests: None declared.