A recent CMAJ article1 does not give Ben Chan's study2 the emphasis it deserves. This is an important document on physician human resources that will have as much impact as the landmark Barer–Stoddart report of 1991.3 Chan diplomatically says “one cannot ‘prove’ that any particular policy ‘caused’ a particular trend to occur. The reader is encouraged to draw his or her own conclusion.”2
However, most of us in the “business” of health care provision recognize the poor quality of decisions made a decade ago by departments of health, licensing bodies, medical associations and medical schools. These decisions were made in the absence of national or regional physician resource planning and without allowance for checks along the way to correct any adverse outcomes.
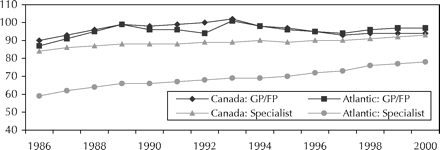
For the 2.4 million people living in Atlantic Canada, the problem is further complicated by the existence of 4 uncoordinated health care plans, one for each province. Economic restraints have not allowed the 2 medical schools in Atlantic Canada to raise their enrolments or adjust postgraduate residency training positions. Physician-to-population ratios for the Atlantic provinces expose the difference in physician resources between this region and the rest of Canada, particularly for specialists (Fig. 1).4
Fig. 1: Physicians per 100 000 population, Altantic provinces, 1986–2000. Calculated from Statistics Canada population data and physician data from the Canadian Institute of Health Information (available on the CMA web site).44
Unfortunately, the same players are now making decisions to increase physician supply, again without national or regional physician resource planning. There is an immediate need to review the increasing health care demands of Canadians and the new technologies becoming available within the Canadian health care system, but already there are plans to increase medical school enrolment. These plans do not account for the fact that primary care physicians are not providing comprehensive care,5 nor do they account for the rising demands for physician extenders in both primary and acute hospital care. We can easily predict the appearance of another report in the next decade, describing another “crisis” and another perceived surplus.
Atlantic Canada urgently needs regional physician resource planning; in fact, we urgently need regional health care planning.
Kevork M. Peltekian Department of Medicine Dalhousie University Halifax, NS