- © 2005 Canadian Medical Association or its licensors
Emmanuel Andrès and colleagues,1 in their comprehensive review of diagnosis and treatment of vitamin B12 (cobalamin) deficiency, fail to consider 2 elements relevant to the Canadian experience.
First, because Canada's flour supply is fortified with folic acid,2 plasma homocysteine level (determined primarily by folate status) is much less effective in the diagnostic work-up of suspected cobalamin deficiency.3 In a large population-based study, we established the test properties of total plasma homocysteine for the diagnosis of cobalamin deficiency among 692 adults in Ontario, after exclusion of people with renal impairment or folate deficiency (red cell folate less than 215 nmol/L).2 A homocysteine value of 15 μmol/L or more did not discriminate between cobalamin concentrations below and above 120 pmol/L (positive and negative predictive values 7.4% and 97.2%, respectively), nor did it discriminate “indeterminate” cobalamin levels between 120 and 150 pmol/L (positive and negative predictive values 6.3% and 94.0%, respectively).2
Second, the diagnostic algorithm for cobalamin deficiency proposed by Andres and colleagues (Fig. 3 in their article1) is unnecessarily complex, especially for seniors, in whom cobalamin malabsorption is commonly found because of age-related atrophic gastritis.4 Although serum methylmalonic acid (MMA) may have a place in a diagnostic algorithm, this indicator of cobalamin insufficiency is falsely elevated in the presence of modest renal impairment5 with advancing age. Furthermore, serum MMA is commonly elevated in elderly North Americans,6 but lowering it through vitamin B12 supplementation does not appear to affect blood hemoglobin concentration, neurological disability score or quality of life.7 Like homocysteine, MMA has not been fully validated as a routine clinical test of cobalamin deficiency,8 especially in the face of increased folate fortification,2 and MMA testing is not routinely available in Canadian centres and community laboratories.
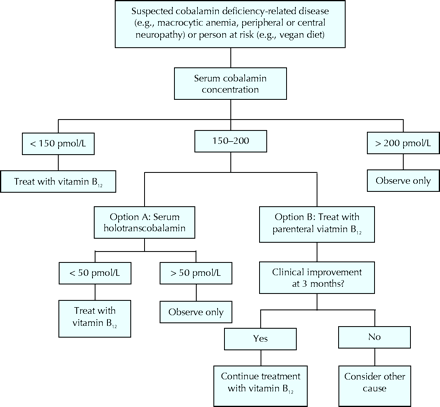
We propose a simpler and more direct diagnostic approach in elderly patients (Fig. 1), with 2 options for serum cobalamin concentrations in the “grey zone” of 150 to 200 pmol/L. Option A involves testing for serum holotranscobalamin — the complex formed by cobalamin and its transport protein, transcobalamin — the physiologically active form of vitamin B12 that is transported into cells.9 This inexpensive, simple radioimmunoassay-based test, which will become more readily available in Canada, displayed a sensitivity of 100% and a specificity of 89% for cobalamin deficiency in one study.9 Option B involves initial treatment with parenteral cobalamin according to the dosing schedule outlined by Andrès and colleagues,1 with assessment of the clinical response after 3 months. High-dose oral cobalamin (e.g., 1000 μg/day) can be used thereafter, as described by Andrès and colleagues.1 A therapeutic response validates not only the diagnosis, but also the treatment, which is otherwise safe and inexpensive.
Fig. 1: Diagnostic approach to suspected cobalamin deficiency in elderly patients.
Footnotes
-
Competing interests: None declared.