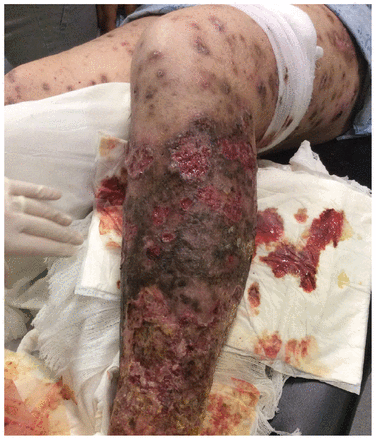
A 41-year-old man was admitted to hospital with painful necrotic leg ulcers (Figure 1). He exhibited narcotic-seeking behaviour, such as requesting narcotics daily, refusing non-narcotic analgesia and hiding narcotics, but he denied using injection drugs. The patient’s ulcers were irregular, with a peculiar black scale on the intact skin. Skin biopsy showed an extensive ulcer with neutrophilic inflammation, and heavy growth of Proteus vulgaris and Morganella morganii was seen on tissue culture. Our presumptive diagnosis was pyoderma gangrenosum with secondary infection. We prescribed prednisone, wound care and antibiotics, and our patient’s lesions began to improve. At the same time, we managed his opioid withdrawal symptoms. About a month into our patient’s stay in hospital, we learned from his roommate and family that he had been injecting a synthetic morphine derivative known as krokodil.
Left leg of a 41-year-old man with injection drug use, showing extensive necrotic ulcers at injection sites. Similar findings were seen on the right leg.
Krokodil is a highly addictive, inexpensive alternative to heroin that has been linked to thousands of deaths in Russia.1–4 In North America, usage is increasing, although it remains much less common than heroin.5 Krokodil has a short half-life, and therefore tends to be injected frequently.4 “Skin-popping,” or injecting drugs into the skin, can induce extensive ulcerative necrosis. Krokodil is believed to cause more extensive skin necrosis than other injected drugs, for reasons that are unknown, with a characteristic green-black scaling likened to crocodile skin (“krokodil” in Russian).1–3 Our patient’s late presentation, and his long stay in hospital before a definitive diagnosis, reflect the stigma of injection drug use.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.