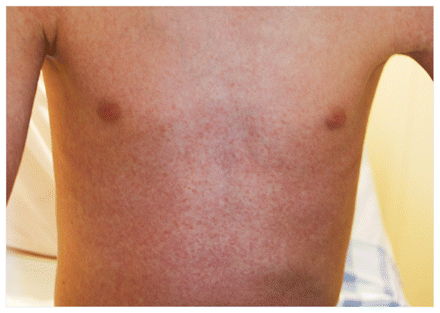
A 14-year-old boy presented with a one-week history of fever up to 39°C and a maculopapular rash on his face, trunk and extremities (Figure 1). Left-sided ulcerative colitis had been diagnosed seven months previously. Initial treatment with oral mesalazine had failed, and sulfasalazine therapy had been started three weeks before presentation. The patient had no other signs of infection or active colitis. Investigations showed elevated transaminases, a high C-reactive protein level and atypical lymphocytosis. Renal function was normal.
Figure 1: Macropapular rash on the trunk of a 14-year-old boy with DRESS (drug reaction with eosinophilia and systemic symptoms) caused by sulfasalazine.
A hypersensitivity reaction to sulfasalazine, known as drug reaction with eosinophilia and systemic symptoms (DRESS), was suspected. The patient’s condition improved with discontinuation of sulfasalazine and treatment with intravenous steroids. His fever resolved within a day, although the rash persisted for two months. The liver enzymes normalized over a month.
A rare idiosyncratic reaction to sulfasalazine, DRESS usually occurs within one to eight weeks after sulfasalazine is started. 1–3 The syndrome is most commonly associated with the aromatic anticonvulsants (i.e., phenobarbital, phenytoin and carbamazepine) and has an incidence of 1:1000 to 1:10 000 exposures to these drugs. 2,3 The exact incidence of DRESS caused by sulfonamides is unknown.
A diagnosis of DRESS requires three criteria: cutaneous eruption, hematologic abnormalities with either eosinophilia (more than 50% of patients) or atypical lymphocytosis (10%–60% of patients, depending on the causative drug), and systemic symptoms (adenopathy, hepatitis, interstitial nephritis, interstitial pneumonitis or carditis). Fever and skin eruption are usually the presenting symptoms. 3 Erythematous and maculopapular lesions typically appear first on the trunk, face and upper extremities, and may progress to blisters, vesicles, pustules or purpura. 3 Exfoliative dermatitis may result.
The late onset and long duration of DRESS, along with presence of hematological abnormalities, differentiate it from other hypersensitivity reactions, such as toxic epidermal necrolysis. Symptoms of DRESS may progress to multiorgan failure; deaths are reported in up to 10% of instances. 2
The pathogenesis of DRESS syndrome is not clear. Patients may have a genetic predisposition characterized by an inability to detoxify the active metabolites. Alternatively, an immuno-allergic mechanism triggered by human herpes virus 6 primary infection or reactivation may be involved. 3,4 Treatment involves discontinuation of the offending drug. Although steroids are often given, the evidence for their efficacy is lacking and symptoms may worsen on tapering them. 5 When DRESS is caused by aromatic anticonvulsants, cross-reactivity is common; the entire class of medications should be avoided. 2 Family members of patients should be counselled for possible genetic susceptibility to DRESS. 3,4
Footnotes
-
Previously published at www.cmaj.ca
This article has been peer reviewed.
Competing interests: None declared.