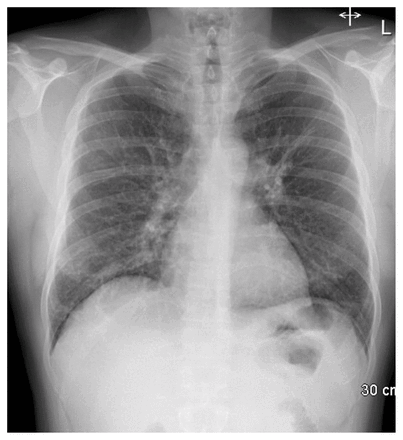
A 44-year-old man with a history of chronic granulomatous disease presented to the emergency department with a 1-day history of fever and shortness of breath. Physical examination showed only tachycardia and tachypnea, with lungs clear to auscultation. Chest radiograph showed diffuse, ill-defined micronodular opacities (Figure 1). The patient was treated with amoxicillin–clavulanic acid for presumed community-acquired pneumonia. He returned 5 days later with persistent fever, progressive dyspnea and hypoxia. Repeat chest radiograph showed substantial progression with new coarse interstitial infiltrates and ground glass opacities (Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.220713/tab-related-content). The patient reported that the day before his symptom onset, he had been feeding hay to large animals at a livestock farm in rural Ontario.
Chest radiograph of a 44-year-old man with chronic granulomatous disease on day 2 of symptom onset, showing ill-defined micronodular opacities with a mid- and lower-lung predominance.
We considered the following diagnoses: acute fungal (aspergillosis, histoplasmosis, blastomycosis) and bacterial (Q fever, nocardiosis) infections. We admitted the patient to hospital on supplemental oxygen and started voriconazole, linezolid, meropenem and doxycycline. Bronchoscopic examination on day 3 of admission showed inflamed bronchial walls. On day 7, samples from bronchoalveolar lavage grew Aspergillus fumigatus complex. He improved and was discharged home on day 12 to continue voriconazole for 3 months.
Chronic granulomatous disease is a genetic condition that arises from a lack of nicotinamide adenine dinucleotide phosphate oxidase; this causes phagocytic dysfunction that predisposes patients to recurrent fungal and bacterial infections. Pneumonia from Aspergillus spp. is the most common infection and cause of death in patients with chronic granulomatous disease.1 This patient’s presentation was most consistent with mulch pneumonitis, an acute fulminant fungal pneumonia after exposure to mulch.2 Mulch pneumonitis typically develops within 1 week of exposure to organic materials such as mulch, wood chips, hay or leaves. The mortality rate for mulch pneumonitis in a case series of patients with chronic granulomatous disease was more than 50%.2 Chest radiography may be unremarkable in the early phase, but diffuse pulmonary infiltrates may occur within 10 days. Mulch pneumonitis should be considered in patients with chronic granulomatous disease who develop respiratory symptoms with history of exposure to organic materials.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/