A 23-year-old man presented to our clinic with acute left-sided numbness for one week. He had been given a diagnosis of lymphoma as a child and had been in remission for more than 10 years. The neurologic examination showed decreased sensation to pinprick over the left side of the patient’s face and left extremities. Brain magnetic resonance imaging (MRI) showed two cystic lesions with concentric rings in the right parietal and right frontal lobes (Figure 1A). We performed a brain biopsy, and the pathology finding showed inflammatory change and gliosis (Appendix 1, available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.180048/-/DC1). The patient’s symptoms resolved after five days of intravenous dexamethasone (4 mg, every 12 hours), but another episode of acute left-sided numbness and weakness developed eight months later. Repeated brain MRI showed large concentric bands in the right parietal lobe (Figure 1B). We diagnosed Balo concentric sclerosis. The patient’s symptoms improved after five days of methylprednisolone treatment (500 mg, once daily). No relapse has been noted in three years of follow up.
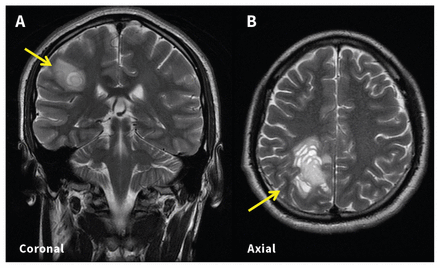
T2-weighted magnetic resonance imaging of the brain of a 23-year-old man showing (A) a concentric ring consisting of hyperintense and isointense signal in the right parietal region; (B) recurrent large concentric bands with multiple hyperintense and isointense layers in the right superior parietal lobe.
Balo concentric sclerosis is an uncommon variant of multiple sclerosis.1 It is distinct from multiple sclerosis owing to a lack of oligoclonal bands in the cerebrospinal fluid, which are commonly found in patients with multiple sclerosis.2 The prevalence is unknown, but may be more common in the Asian population. Using MRI, the diagnosis can be made when there are two or more concentric rings consisting of hyperintense and isointense signals on T2-weighted images; brain biopsy is needed only when the diagnosis is ambiguous.3,4 The differential diagnosis includes acute disseminated encephalomyelitis, central nervous system lymphoma or brain abscess. Pathology findings show demyelinating change in white matter with gliosis and microvascular involvement.1
Generally, the clinical course is monophasic, meaning there is one episode of the disease. Corticosteroids are suggested as first-line treatment; plasma exchange and immunosuppressants are second-line options. The prognosis is favourable if it is managed in a timely manner.1
Acknowledgements
The authors thank Drs. Che-Yi Chou, Ming-Kuei Lu, Nien-Yi Chang and Kai-Po Chang for their guidance and effort. The paper was supported in part by grants from the Ministry of Science and Technology (MOST 105-2314-B-039-004-MY2, MOST107-2632-B-039-001), the China Medical University Hospital (DMR-106-180, DMR-107-189), and the Taiwan Ministry of Health and Welfare Clinical Trial and Research Center of Excellence (MOHW107-TDU-B-212-123004).
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.