Intravenous immunoglobulin is derived from pooled plasma from thousands of healthy donors and contains polyspecific IgG. In addition to its indication for immunodeficiency disorders, immunoglobulin is used in a variety of immune-mediated disorders. Several issues remain unresolved: optimal dose, differences in composition between products, and combination therapy with other biologics. More importantly, the mechanisms of action of immunoglobulin remain elusive, although several mutually nonexclusive effects have been proposed.1
In this article, we summarize the impact of intravenous immunoglobulin on the immune system. We also discuss clinical use, emphasizing the evidence supporting immunoglobulin’s use as an immune-modulating agent. Depending on the disease, there is huge variability in the quality of evidence, from single case reports to well-conducted randomized controlled trials (RCTs). The search strategy used for this review is presented in Box 1.
Evidence used in this review
We used national guidelines from France, the United States, the United Kingdom, Canada and Australia to identify approved indications for intravenous immunoglobulin in autoimmune and inflammatory diseases (Appendix 1). In addition, we searched MEDLINE (1980 to present) and the Cochrane Database of Systematic Reviews using the following terms: “immunoglobulins, intravenous,” “immunoglobulins,” “IVIg” and the relevant diseases mentioned in the national guidelines. We excluded the diseases for which there was insufficient evidence and restricted our review to the literature published in English or French. Additional articles were identified through manual searches of the reference lists of relevant articles. We used the US Department of Health and Human Services’ Agency for Healthcare Research and Quality system to assess the level of evidence (see details in Appendix 2). [Appendices are available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.130375/-/DC1]
What is the immunologic basis for intravenous immunoglobulin use?
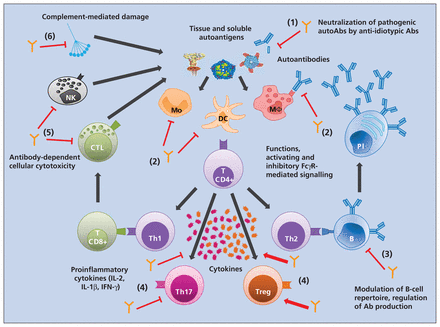
Autoimmune and inflammatory diseases are associated with a highly perturbed immune system implicating various immune cells and inflammatory mediators such as cytokines and chemokines. It is therefore unlikely that a single component of intravenous immunoglobulin provides the immunologic basis for its use as an immune-modulating agent. Depending on the disease and models, different mechanisms of action have been identified, although it is possible that these mechanisms work in a synergistic manner (Figure 1).
Impact of intravenous immunoglobulin on the immune system. Exposure of autoantigens triggers the recognition by antigen-presenting cells, leading to activation and polarization of T helper cells. T helper cells and innate cells provide activation signals through cytokines, which leads either to production of autoantibodies from the differentiated B cells into plasma cells or to tissue damage from the release of inflammatory mediators by immune cells, complement activation and antibody-dependent cell-mediated cytotoxicity. Intravenous immunoglobulin interacts with various cellular and soluble components of the immune system involved in the inflammatory and autoimmune process: (1) it neutralizes pathogenic autoantibodies through the anti-idiotypic network; (2) it modulates the expression of Fc receptors and inhibits the maturation and activation of antigen-presenting cells; (3) it regulates antibody synthesis and the B-cell repertoire; (4) it shifts the balance between subsets of T helper cells and downregulates the production of pro-inflammatory cytokines by T cells; (5) it blocks antibody-dependent cell-mediated cytotoxicity; and (6) it blocks complement activation. Orange antibody structures = intravenous immunoglobulin; dark grey arrows = activation signalling; red arrows = agonist effect of intravenous immunoglobulin; red T bars = inhibitory effect of intravenous immunoglobulin. Ab = antibody, B = B cell, CTL = cytotoxic T cell, DC = dendritic cell, FcγR = Fcγ receptor, IFN = interferon, IL = interleukin, Mo = monocyte, MΦ = macrophage, NK = natural killer cell, Pl = plasma cell, Th = T helper cell, Treg = regulatory T cell.
One of the first identified mechanisms of action of intravenous immunoglobulin was blockade of Fcγ receptors on macrophages, thereby inhibiting platelet phagocytosis in idiopathic thrombocytopenic purpura.2 Subsequently, immunoglobulin was shown to exert an anti-inflammatory effect through upregulation of inhibitory Fcγ receptor IIB on macrophages.3 Fcγ receptor IIB contains an immunoreceptor tyrosine-based inhibitory motif that switches off the intracellular inflammatory cascade. Intravenous immunoglobulin inhibits complement-mediated tissue damage and modulates the cytokine network: it suppresses the production of proinflammatory cytokines4 while increasing the production of anti-inflammatory mediators such as interleukin-1 receptor antagonist.
Intravenous immunoglobulin modulates different cells of the innate and adaptive immune compartments, including dendritic cells, monocytes and macrophages, granulocytes, natural killer cells, B cells and various subsets of T cells.5 It expands the number of regulatory T cells, which play a critical role in maintaining immune tolerance,6 and inhibits the differentiation and function of T helper 17 and T helper 1 cells,7 which are involved in several autoimmune diseases. Intravenous immunoglobulin alters B- and T-cell interactions and downregulates pathogenic antibody production.8
For which diseases is intravenous immunoglobulin effective?
Autoimmune diseases are rare and heterogeneous, involve complex and different physiopathologic mechanisms and demand multiple treatment strategies with varying outcomes. Determining the efficacy of intravenous immunoglobulin for these conditions requires selection of clinically relevant outcome measures that are assessed at appropriate points. Although a limited number of placebo-controlled trials have shown its efficacy, intravenous immunoglobulin is helpful and may avoid the excessive use of immunosuppressive agents such as corticosteroids or invasive procedures such as plasmapheresis. Use of intravenous immunoglobulin is established as a first-line treatment in patients with the following indications.
Neurologic disorders
Intravenous immunoglobulin is effective in the treatment of peripheral nervous system disorders.9,10
In chronic inflammatory demyelinating polyneuropathy, evidence for the use of immunoglobulin (2 g/kg) is supported by a meta-analysis of seven RCTs involving 287 patients.11 Compared with placebo, immunoglobulin resulted in significantly higher rates of improvement overall (44%, 95% confidence interval [CI] 32% to 62%, v. 18%) and reduction in degree of disability (relative risk [RR] 2.4, 95% CI 1.72 to 3.36) over study durations of two to six weeks. The short-term efficacy of intravenous immunoglobulin is similar to that of plasma exchange and corticosteroid therapy but with a better tolerance profile.12 The benefit of immunoglobulin is transient, however, and long-term management of the disease may require regular infusions.
Intravenous immunoglobulin is used in addition to supportive care in patients with Guillain–Barré syndrome and should be started within two weeks from disease onset according to expert opinion. A Cochrane systematic review13 showed that, in at least three RCTs enrolling up to 536 patients, daily doses of 0.4 g/kg for five days improved motor function at one month and reduced time to recovery, efficacy similar to that seen with plasmapheresis. However, intravenous immunoglobulin did not significantly change the disability grade (mean difference −0.02 of a grade, 95% CI −0.25 to 0.2).
In myasthenia gravis, the indication for intravenous immunoglobulin is restricted to either exacerbated or worsened clinical conditions, because first-line treatment with oral cholinesterase inhibitors is sufficient in most patients.14 Limited evidence from a subgroup of 28 patients with severe disease in an RCT of immunoglobulin (2 g/kg) versus placebo showed clinically important improvement after 14 days in the quantified myasthenia gravis score, a validated measure of target organ function (mean difference −3.40, 95% CI −5.74 to −1.06). In another RCT, involving 84 patients, intravenous immunoglobulin showed an improvement rate similar to that seen after five sessions of plasmapheresis (69% v. 65%, p = 0.74).15 A lower dose of 1 g/kg may be sufficient, because it showed similar efficacy to a dose of 2 g/kg in an RCT involving 168 patients.16 In Guillain–Barré syndrome and myasthenia gravis, the choice between intravenous immunoglobulin and plasmapheresis should be based on the practical availability and respective contraindications related to each therapy.
High-dose immunoglobin treatment (2 to 2.5 g/kg) is indicated for use in multifocal motor neuropathy, based on a meta-analysis of four RCTs involving 34 patients.17 Compared with placebo, immunoglobulin showed greater (albeit nonsignificant) reductions in disability (39% v. 11%; RR 3, 95% CI 0.89 to 10.12) and significantly higher rates of improvement in muscle strength (78% v. 4%; RR 11.00, 95% CI 2.86 to 42.25). Intravenous immunoglobulin should be considered as first-line therapy in view of the lack of alternative treatments with an acceptable safety profile. However, cost–benefit issues should be considered, because maintenance therapy is often required.
Autoimmune mucocutaneous blistering diseases
Intravenous immunoglobulin may be effective in corticosteroid-resistant pemphigus vulgaris or pemphigus foliaceus.18 Only one RCT, involving 61 patients, compared a single cycle of immunoglobulin (0.4 or 0.2 g/kg daily for five days) with placebo.19 Patients who received 0.4 g/kg of immunoglobulin stayed on the protocol significantly longer than those given placebo (p < 0.001) without the need for additional treatment during an 85-day observation period. The most effective way of using immunoglobulin in pemphigus has not yet been determined, and response rates appear higher when the agent is given in combination with other biologics than when given alone (91% v. 56%).20 In particular, combination therapy with rituximab seems promising.
In bullous pemphigoid, weak evidence suggests that intravenous immunoglobulin could be used as adjuvant therapy to corticosteroids in refractory cases or as a sparing agent to prevent adverse effects of immunosuppressive drugs. A recent review of 41 published case reports showed that a cycle of immunoglobulin of 2 g/kg was clinically effective in about 80% of the patients and led to the withdrawal of other immunosuppressive treatment.21 In view of the limitations owing to diverse definitions for outcome measures,22 it is difficult to compare the efficacy of therapeutic alternatives and to indicate a schedule of treatment.
Idiopathic thrombocytopenic purpura
The efficacy of intravenous immunoglobulin on the recovery of platelets in idiopathic thrombocytopenic purpura has long been shown to be similar to that of steroids, with some advantages.23 Several dosage regimens of immunoglobulin have been designed, and in a meta-analysis of 13 trials enrolling 646 patients,24 a dose of 1 g/kg for two consecutive days had an efficacy rate of about 80% in obtaining an increase of more than 50 000 platelets per mm3 (50 × 109/L) on day 5. In relapsing idiopathic thrombocytopenic purpura, repeat infusion of immunoglobulin could constitute an alternative for splenectomy,25 although newer strategies such as rituximab and thrombopoietin receptor agonists are currently favoured.
Kawasaki disease
Beneficial effects of intravenous immunoglobulin have been clearly shown in patients with Kawasaki disease.26 In one trial, involving 85 children, high doses of immunoglobulin (0.4 g/kg daily for four days) reduced the occurrence of coronary artery abnormalities at day 30 compared with acetylsalicylic acid (ASA) alone (15% v. 42%, p = 0.006).27 A meta-analysis of several studies, involving more than 1000 children, showed that immunoglobulin given at a high infusion rate (2 g/kg over 10 h) and in combination with ASA and steroids reduced the rate of coronary artery defects significantly more than a standard immunoglobulin regimen combined with ASA (7.6% v. 18.9%; odds ratio 0.3, 95% CI 0.20 to 0.46).28
Kidney transplantation
Few treatment options are available to enable patients highly sensitized to human leukocyte antigens (HLA) to undergo kidney transplantation. An RCT involving 24 patients showed that, compared with placebo, intravenous immunoglobulin at a dose of 2 g/kg monthly for four months before transplantation significantly reduced anti-HLA antibody levels and the projected mean time to transplantation (4.8 v. 10.3 yr, p < 0.05).29 Another RCT, involving 30 patients with steroid-resistant graft rejection, showed that intravenous immunoglobulin at 0.5 g/kg daily for seven days provided a two-year graft survival rate of 80%, similar to that achieved with muromonab-CD3.30
Inflammatory myopathy
Intravenous immunoglobulin has been used successfully in steroid-resistant and severe forms of myopathy.31,32 In dermatomyositis, a pivotal RCT of three monthly injections of immunoglobulin (2 g/kg) versus placebo in 15 patients showed a rapid and significant improvement (p < 0.02) in the mean muscle strength score in the treatment group (from 76.6 ± 5.7 standard deviations to 84.6 ± 4.6), compared with no change in the placebo group (from 78.6 ± 6.3 to 78.6 ± 8.2). In polymyositis, no randomized studies were identified in the literature search, but intravenous immunoglobulin was found to be effective in uncontrolled studies.33,34
Other diseases
Evidence, albeit relatively weak, has shown promising outcomes with the use of intravenous immunoglobulin in several other conditions. For some of these indications, use of immunoglobulin is authorized by national drug agencies; for others, it is off-label use. The lack of evidence is due mainly to underpowered studies related to small numbers of patients. Systematic reviews and guidelines35,36 specify the level of evidence, the details of which are summarized in Table 1.
For which diseases is intravenous immunoglobulin not recommended?
In certain diseases, the use of intravenous immunoglobulin has met with only little efficacy and is therefore not recommended. In others, it is not recommended based on a strong level of evidence (RCTs or meta-analyses of RCTs). For example, in relapsing–remitting multiple sclerosis, an RCT involving 150 patients showed no improvement in the occurrence of relapses with immunoglobulin versus placebo.37 Immunoglobulin was found to be ineffective in secondary progressive multiple sclerosis in a placebo-controlled RCT involving 197 patients.38 A recent placebo-controlled RCT failed to show a beneficial effect in Alzheimer disease.39 In juvenile rheumatoid arthritis, inclusion body myositis and eczema, evidence from small RCTs failed to support immunoglobulin use.40–42
In other diseases, alternative treatments are more effective. In an observational study involving infants with autoimmune neutropenia, 50% of those given intravenous immunoglobulin before elective surgery or because of severe infection responded to treatment, as compared with 100% of the eight patients given granulocyte colony-stimulating factor.43 In chronic fatigue syndrome, asthma and schizophrenia, the efficacy of immunoglobulin seems to be unlikely because the physiologic rationale is not sound.
In certain conditions, intravenous immunoglobulin has been shown to be deleterious and should be avoided. A trial of immunoglobulin therapy for the DRESS (drug reaction with eosinophilia and systemic symptoms) syndrome was stopped because of serious adverse events (severe malaise with hemodynamic changes during immunoglobulin infusion, and pulmonary embolism and hemophagocytic syndrome during follow-up).44 Although use of immunoglobulin as first-line treatment in diseases such as hemophagocytic syndrome has been reported in a few cases,45 another report46 suggests that it is not adequate for secondary hemophagocytic syndrome related to Epstein–Barr virus infection and would delay the appropriate treatment.
What are the adverse effects?
The most common adverse events associated with intravenous immunoglobulin use are mild and transient (Table 2).47 Potentially serious but less common events include volume overload, acute renal failure, thromboembolism and anaphylaxis. Adverse reactions are generally managed with supportive treatment and by slowing or stopping the immunoglobulin infusion.
Adverse effects associated with intravenous immunoglobulin use
Contamination of immunoglobulin with infectious agents is always a possibility. However, multiple steps of chemical and enzymatic purification followed by chemical or physical virus inactivation help improve the safety of the product.48
Unanswered questions
Although intravenous immunoglobulin has been widely used as an immune-modulating agent for more than 30 years, little is known about factors that predict treatment success, even in situations for which a well-documented evidence base exists. Treatment-responsive subsets of diseases have to be identified to clarify the real impact of immunoglobulin therapy. Furthermore, one could expect differences in effectiveness between the various preparations because of their different subclass compositions, but data are lacking as to whether this has important clinical implications.
In several diseases, the effect of intravenous immunoglobulin is transient. In the event of relapses, long-term management is difficult because optimal combination therapy or schedules of treatment are not well established.
Because of safety issues and manufacturing processes, the cost of intravenous immunoglobulin is not likely to decrease. Thus, use of more concentrated preparations may be an alternative to reduce the duration of infusion and the time required for involvement of health professionals. Subcutaneous administration of immunoglobulin has shown promising results in patients with multifocal motor neuropathy,49 and other trials of subcutaneous use are under way in patients with myasthenia gravis (ClinicalTrials.gov NCT01828294), chronic inflammatory demyelinating polyneuropathy (ClinicalTrials.gov NCT01017159) and dermatomyositis (ClinicalTrials.gov NCT02271165).
Another concern relates to the limited availability of immunoglobulin, because shortages have occurred in the past. In such circumstances, priority for allocation should be given to indications for which strong evidence of benefit exists or to severe life-threatening conditions. Alternatively, in view of promising results in experimental models,50 clinical trials should be undertaken with recombinant sialylated Fc fragments of IgG that are not derived from blood, which could help to overcome shortages of intravenous immunoglobulin in the future.
Key pointsIntravenous immunoglobulin exerts anti-inflammatory and immune-modulating effects through broad and possibly synergistic mechanisms.
Conditions for which clear evidence favours first-line use of intravenous immunoglobulin include idiopathic thrombocytopenic purpura, Kawasaki disease and polyneuropathies such as Guillain–Barré syndrome.
Most unlicensed and off-label use is supported by little or no evidence.
Prioritization of indications for this limited and costly product is important to avoid the risk of shortages owing to increasing off-label use.
Acknowledgements
The authors thank Olivier Benveniste for critical reading of the manuscript, Antoine Guéguen and Denis Glotz for their constructive comments and Mathieu Ing for his help in drawing the figure. Laurent Gilardin was the recipient of a Poste d’accueil INSERM, Institut national de la santé et de la recherche médicale.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Laurent Gilardin performed the literature search. All of the authors reviewed the literature, drafted and revised the manuscript, approved the final version for publication and agreed to act as guarantors of the work.