A 36-year-old man with a 9-year history of stable, relapsing-remitting multiple sclerosis (MS) presented to the emergency department with a 1-week history of blurred vision, vertigo, perioral numbness, difficulty walking, aggression and confusion. Symptoms persisted despite the patient having started prednisolone 3 days before presentation. Several months previously, he had discontinued his maintenance therapy for MS — dimethyl fumarate, a nuclear factor erythroid 2–related factor 2 activator — owing to severe diarrhea.
After admission, the patient became increasingly quadriplegic. His state of arousal changed rapidly, with initial inattention quickly progressing to obtundation, then coma. Our differential diagnoses included opportunistic central nervous system (CNS) infection, acute disseminated encephalomyelitis, CNS lymphoma, Marburg multiple sclerosis (MS) and Balo concentric sclerosis, rare variants of MS. His lumbar puncture showed a raised leukocyte count of 66 (normal < 5) × 106 L, 91% lymphocytes, increased immunoglobulin G index and oligoclonal bands. Magnetic resonance imaging (MRI) showed numerous large subcortical T2 hyperintense and postgadolinium-enhancing lesions, and a ring-enhancing lesion, showing a breakdown of the blood–brain barrier and acute inflammation (Figure 1). We diagnosed fulminant MS (Marburg MS).
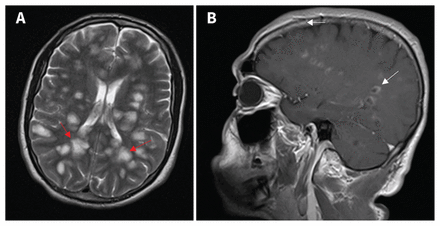
(A) Magnetic resonance imaging (axial T2 image) in a 36-year-old man, demonstrating multiple tumour-like, confluent and demyelinating hyperintense lesions (red arrows) through the subcortical white matter. (B) Sagittal postgadolinium T1 image, showing numerous enhancing lesions, indicative of acute inflammation, with a representative partially ring-enhancing lesion (white arrows).
After admission to intensive care, the patient received 3 days of methylprednisolone and, because of rapid deterioration, high-dose intravenous cyclophosphamide over 4 days with granulocyte-colony stimulating factor support. Two weeks later, an MRI scan showed marked reduction in the number of enhancing lesions, and the patient regained functional independence.
Marburg MS accounts for less than 4% of MS and is usually fatal unless promptly recognized and treated.1 It typically presents in children or young adults, with multifocal diffuse white matter lesions in the brain or brainstem and severe acute myelin loss.1 The etiology of Marburg MS remains unclear, but we considered that our patient stopping his maintenance therapy was a major contributing factor.
Rapid progression to coma and confluent tumefactive lesions with incomplete ring enhancement on MRI differentiates Marburgvariant from classic MS.2 Patients do not usually respond to high-dose steroids or plasmapheresis; however, recent reports have shown efficacy with high-dose cyclophosphamide, as in our patient, as well as intravenous immunoglobulin and mitoxantrone.3,4
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/