Abstract
The Sexual Assault Service, operated by the Children's & Women's Health Centre of British Columbia in partnership with the Vancouver General Hospital Emergency Department, started offering HIV prophylaxis in November 1996 to patients presenting to the emergency department after a sexual assault. In the first 16 months of the program a total of 258 people were seen by the service, of whom 71 accepted the offer of HIV prophylaxis. Only 29 continued with the drug treatment after receiving the initial 5-day starter pack, and only 8 completeid the full 4-week treatment regmen and returned for their final follow-up visit. Patients at highest risk for HIV infection (those who had penetration by an assailant known to be HIV positive or at high risk for HIV infection [men who have sex with men, injection drug users]) were more likely to accept prophylaxis and more likely to complete the treatment than those at lower risk. Compliance and follow-up were the main problems with implementing this service. Service providers found it difficult to give the information about HIV prophylaxis to traumatized patients. After this program evaluation, the service changed its policy to offer HIV prophylaxis only to people at high risk of HIV infection. This targeting of services is expected to make the service providers' jobs easier and to make the program more cost-effective while still protecting sexual assault victims against HIV infection.
Women and men who have been sexually assaulted often express a fear of getting AIDS. The Sexual Assault Service, a program operated by the Children's & Women's Health Centre of British Columbia in partnership with the Vancouver General Hospital Emergency Department, offers 24-hour on-call service to patients who have been sexually assaulted. About 200 patients are seen each year. On Nov. 1, 1996, the service started offering HIV prophylaxis. This was the first time a sexual assault service in North America had initiated such a policy. In this article the authors describe why and how the policy was implemented, the evaluation of the first 16 months after its implementation and changes to the program resulting from the evaluation.
Information about the effectiveness of postexposure HIV prophylaxis comes from experiences with health care workers. In 1995 a retrospective case-control series in the United States showed a 79% reduction of HIV transmission among health care workers who had had needle-stick injuries and who had taken zidovudine (AZT) prophylaxis.1 In 1997 a large case-control study showed a 10-fold decrease in the seroconversion rate with postexposure prophylaxis.2 In 1998 the US Centers for Disease Control and Prevention (CDC) recommended that postexposure HIV prophylaxis be offered to health care workers.3
Because there are no published data on the effectiveness of HIV prophylaxis among people who have been sexually assaulted, the decision to offer it through the Sexual Assault Service was based on an assessment of the rate of HIV transmission through sexual intercourse and the rate of HIV infection among assailants. There are few reports of HIV transmission due to sexual assault.[4–9] The rate of transmission from consensual vaginal intercourse is about 1 in 500 and for anal intercourse 1 in 50.7 There have been reports of "high-risk HIV transmitters,"[10, 11] including those recently infected and those at late stages of the disease.[12, 13] Rates also increase with exposure of non-intact mucosa.10 Among sexual assault victims, there are often documented genital injuries[14–16] and a high rate of STDs.17 In British Columbia the rate of HIV infection in the male population is about 0.5%, but it is about 15% among men who have sex with men and 30% to 40% among injection drug users.[18, 19] In about half of the cases seen in our service, the person attacked does not know the assailant and thus the assailant's sexual or drug history.14
Side effects of the various antiretroviral drugs are common and often severe enough to cause noncompliance. In a study of HIV prophylaxis after accidental exposure, 5-day starter kits were given to 176 people, of whom 78 received the rest of the 23 days' worth of therapy; only 58 completed the full treatment, and 52.4% of them had side effects.20 Older health care workers who had a needle-stick injury involving a patient known to be HIV positive were the most likely to complete treatment, and younger health care workers who had community exposure to someone with unknown HIV status were least likely to complete treatment.
In cases of recent infection, the virus replicates and creates more than 10 billion new virions per day before a host immune response develops.21 With combination antiretroviral therapy, the viral load can be decreased by 50% within 3 days and, ultimately, by more than 99%.22
Objective
Because we felt that patients deserve the choice to try to reduce their chance of HIV transmission after a sexual assault, the Sexual Assault Service decided to initiate a program through which HIV prophylaxis would be offered to patients at moderate to high risk of infection. Although the 1998 CDC guidelines recommend that prophylaxis be offered only within 72 hours after exposure for health care workers who have percutaneous exposure to HIV,3 for patients presenting to our service between 1996 and 1999 it was decided not to restrict the timing because it has been shown that treating HIV infection early can also be helpful.23
Program description
Input was solicited from several groups who worked with HIV-positive patients and sexual assault victims. These included physicians from the BC Centre of Excellence in HIV/AIDS, a physician treating women with AIDS at the Oak Tree Clinic (a clinic affiliated with the Children's & Women's Health Centre of British Columbia that is dedicated to the treatment of women and children with HIV disease), members of a community organization called Women Against Violence Against Women Rape Crisis Centre (WAVAW), street nurses, representatives from the BC Centre for Disease Control, and nurses and physicians with the Sexual Assault Service. The policy and patient handouts were designed with input from these groups.
The debate about whether to offer HIV prophylaxis was interesting. Proponents of the program argued that, if there was a possibility of preventing HIV transmission, the service had an obligation to offer it. Those against the program argued that the patients were already so traumatized that they would be overwhelmed and would have difficulty giving truly informed consent, that the evidence was limited about the effectiveness of HIV prophylaxis in this patient population, that there were concerns about the side effects and risks of the drug therapy and that the duration of the examination would be increased.
In the end the program was approved. It consisted of 4 steps: risk assessment, offer of prophylaxis, arrangement for follow-up and outcomes assessment.
Risk assessment
Each patient's risk factors for HIV transmission were assessed by the physician or nurse in the emergency department. Patients at high risk of infection were defined as those who suffered a penetration assault by one or more assailants known to be HIV positive or at high risk of HIV infection (injection drug users or men who have sex with men). Patients at moderate risk were defined as those who suffered a penetration assault by one or more assailants of unknown HIV status. Patients at low risk were those whose assault involved no anal or vaginal penetration, no ejaculation from the assailant, oral penetration only or condom use, or whose assailant was known to be HIV negative.
Offer of prophylaxis
Medical contraindications to the offering of prophylaxis included renal insufficiency, hepatic insufficiency, myelosuppression and concurrent therapy with myelosuppressive, hepatotoxic or nephrotoxic drugs. Patients at low risk of HIV infection were not offered prophylaxis; anxiety in low-risk cases was dealt with as anxiety and not a reason to start prophylaxis. Other patients were counselled that they were at higher risk; most of them were considered to be at moderate risk. All patients who were not at low risk were told about the medications, that there was no proof that the drugs would prevent HIV infection but that they may work, and that the chances of HIV transmission after one sexual contact are very low.
Because the timing of HIV prophylaxis is important, patients who had difficulty deciding whether to take the drugs were started on the medications as soon as possible and told that they could make a more considered decision later to quit or continue the therapy. This step was taken because patients seen hours after a sexual assault are traumatized and have difficulty processing all the information about risks, side effects and benefits of HIV prophylaxis.
Patients who agreed to the prophylaxis were given a 5-day starter kit of 2 antiretroviral agents, AZT and zalcitabine (DDC), and information about the side effects and about the follow-up appointments. During the 16-month study period, the BC Centre for Excellence in HIV/AIDS changed the drugs to AZT and lamivudine (3TC) because of drug resistance.
Arrangement for follow-up
Follow-up was offered at an easily accessible community clinic where the physicians were trained to handle patients from the Sexual Assault Service. At the first follow-up visit, 2 to 5 days after the initial presentation, the risks, benefits and side effects of HIV prophylaxis were reviewed, and blood was drawn for HIV antibody testing, a baseline complete blood count, and liver and renal function tests. The patient was provided with a prescription for the next supply of drugs (for up to 23 days).
At the 2-week follow-up visit the test results were given, side effects reviewed and blood tests repeated. At the final visit, at the end of the 4-week treatment period, the blood tests were repeated and a schedule for HIV antibody testing at 6 weeks, 3 months, 6 months and 12 months was recommended. The BC Centre for Excellence in HIV/AIDS recommended following patients for 12 months because antibody formation can be delayed in cases in which prophylaxis fails. This policy is based on an unpublished report of a health care worker who was given HIV prophylaxis and in whom seroconversion occurred 9 months after exposure. Others recommend a 6-month follow-up.24
Outcomes assessment
During regular follow-up telephone calls, the counsellor working with the Sexual Assault Service asked the patients whether they were having any problems with the medications. The physicians at the follow-up clinic kept records of side effects and drug compliance.
After implementation of the program, at the regular meetings of the Sexual Assault Service, the physicians and nurses talked about the difficulties of discussing HIV prophylaxis with traumatized patients.
Program evaluation
During the 16-month study period of Nov. 1, 1996, to Feb. 28, 1998, the service saw 256 women and 5 men; 258 of the patient charts had adequate information for review. The mean age of the patients was 26 years (range 13 to 82). Of the 244 patients for whom the time from the assault to presentation at the service was recorded, 69 (28.3%) were seen within 6 hours, 106 (43.4%) between 6 and 24 hours, 31 (12.7%) between 24 and 48 hours, and 38 (15.6%) after 48 hours. Police were involved in 58.1% (150/258) of the cases. Sperm was noted in only 19.4% (50/258) of the cases. The assailant was unknown to the victim in 45.7% (116/254) of the cases. Anal injuries were seen in 7.8% (20/258) and vulvovaginal injuries in 42.2% (109/258). A condom was used in only 16 (6.2%) of cases.
Of the patients, 71 accepted HIV prophylaxis. They appeared to be at higher risk than the ones who did not accept it. This was especially true for those whose assailant was known to be HIV positive, was a man who has sex with men or was an intravenous drug user (p = 0.033), and for those whose assault involved anal penetration (p = 0.01) (Table 1).
Table 1: Details of sexual assault cases seen by the Sexual Assault Service between November 1996 and February 1998
Although the income level of those accepting prophylaxis was higher than that of the group who did not accept it, this difference was not statistically significance (χ2 = 2.51, p = 0.11). There was also no significant difference in age, police involvement or recognition of the assailant between those who did and those who did not accept prophylaxis.
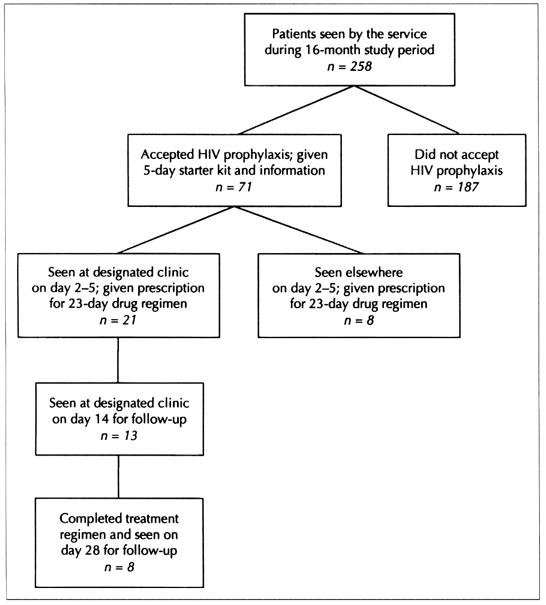
Of the 71 patients given the 5-day starter kit, 42 did not return for their first follow-up visit (Fig. 1). Some of these were contacted by telephone: most of them said that they had quit taking the medications because they had read the information at home and decided that it was not worth the side effects.
Fig. 1: Flow of patients who had been sexually assaulted and were offered HIV prophylaxis by the Sexual Assault Service between November 1996 and February 1998.
A total of 29 returned for the first follow-up visit and the prescription for the rest of their medications. Nine of them later dropped out of the program for the following reasons: they were "too sick," were "unable to work," had a rash, decided against the prophylaxis after reviewing handouts at home or with their family physician, discovered they were HIV positive on baseline testing or had abnormal blood test results (this last patient was also receiving psychotropic medication). Another 12 did not return for follow-up; we do not know whether they completed the treatment. Of the 8 patients known to have completed the whole course of treatment, most were at high risk for HIV infection. Two of the 8 were incarcerated or admitted to a drug treatment facility, where the medications were dispensed. There were no known seroconversions.
Cost analysis
Although the fear of HIV infection is a major reason for offering prophylaxis to sexual assault victims, it is important to consider the costs.25 The cost per patient of the 5-day starter kit was $100 and of the remaining 23 days of treatment $460. The total cost during the study period was $20 440 for the drug therapy and about $2500 for the blood tests and office visits. This translated to about $90 per patient seen in the service, $325 per patient started on prophylaxis, $700 per patient who may have completed the treatment and $3000 per patient known to have completed the treatment.
The cost of a single case of seroconversion has been estimated to be $150 000.26 This estimate was based on direct medical costs alone, not on lost wages or other social costs. This means we could offer HIV prophylaxis to 1500 sexual assault victims before we would have spent what it costs to treat one person who becomes HIV positive. Even in the worst case, if each patient has a 1% risk of becoming HIV positive and takes $700 worth of drugs and services to have a 70% decrease in risk, 140 patients could be treated at a cost of about $100 000 to prevent one case of seroconversion.
Lessons learned
The biggest barrier to implementation of the program was drug compliance. Once HIV prophylaxis was started, the likelihood was very low that the patient would continue the complicated drug regimen for 4 weeks to prevent a theoretical risk. Even programs in occupational settings have found compliance to be a major problem. In a study of HIV prophylaxis after accidental exposure, only 58 of 176 patients completed the full treatment.20 In our study population, in which post-traumatic stress symptoms from the sexual assault were common and 55% of the patients were found to have an income level representing the lowest third decile for British Columbia,[27, 28] the poor compliance rate is not surprising.
Since our program evaluation, we have changed the program significantly. Instead of offering HIV prophylaxis to all patients at moderate and high risk, we now offer it only to those at high risk. This change is likely to improve compliance, because in our evaluation those at highest risk were most likely to complete the drug treatment. It will also reduce drug costs and will ease the burden on the physicians and nurses, as fewer patients will need to be counselled about HIV prophylaxis.
The BC Centre for Excellence in HIV/AIDS has again changed the drugs given for HIV prophylaxis, and now we offer a 5-day starter kit containing stavudine (D4T), 40 mg twice daily, and lamivudine (3TC), 150 mg twice daily, with the addition of nelfinivir, 750 mg 3 times daily, in cases in which there is a concern about drug resistance. The BC Centre for Excellence in HIV/AIDS also changed the timeframe of starting HIV prophylaxis to 36 hours after exposure. The new drugs are more expensive, but they are necessary because the drug-resistance profiles have changed. Also, they may improve compliance rates because there are fewer side effects.
Our program evaluation had limitations. The collection of information at the time of starting the prophylaxis and at the follow-up visits was not sufficiently rigorous. As a result, we do not know the outcomes of many of the patients who accepted HIV prophylaxis, or how many were not offered prophylaxis and why. We have changed the forms that patients are asked to complete in the emergency department so that we can determine why patients are not offered prophylaxis. Another limitation was that we were unable to track seroconversion rates among the patients who took the HIV prophylaxis because of the difficulties in obtaining consent for longer follow-up.
On the basis of our experience, we believe that sexual assault services should offer HIV prophylaxis to patients at high risk of HIV infection, because some cases of HIV infection after such exposure may be preventable and because HIV infection is a major fear of sexual assault victims. Moreover, since the CDC has recommended that postexposure HIV prophylaxis be offered to health care workers, people may be expecting it. We hope that our experience and the information we have reported here will assist others in deciding on and planning service needs in other areas.
We are grateful to the other members of the Sexual Assault Service for their help with this project.
Competing interests: None declared.
Footnotes
-
This article has been peer reviewed.
Reprint requests to: Dr. Ellen R. Wiebe, Ste. 1013, 750 West Broadway, Vancouver BC V5Z 1H9; fax 604 873-8304; [email protected]