Abstract
The caseA 6-month-old girl presents to her pediatrician with lethargy; she has been vomiting and the vomit is bile stained. She is admitted to hospital for tests. Plain radiographs of the abdomen and barium enema examination are normal. Results of an upper gastrointestinal (GI) study are suspicious for, but not diagnostic of, intestinal malrotation. The patient improves quickly and is discharged the following day. Over the next 2 months she continues to have similar short-lived episodes lasting a few hours, for which she is seen in the emergency department by on-call physicians. Her pediatrician initiates investigations to rule out an endocrine cause of the vomiting, when she has to be readmitted to hospital because of a severe episode. On this occasion, the girl's condition rapidly deteriorates and, despite active resuscitation during a barium enema examination to rule out intussusception, she dies. Post-mortem examination shows midgut infarction due to malrotation-associated volvulus with peritonitis.
Definition
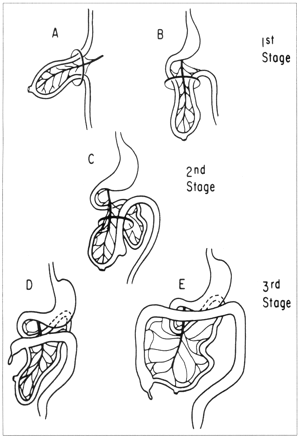
Intestinal malrotation is the term given to errors of rotation of the midgut around the superior mesenteric artery and the midgut's subsequent fixation in the peritoneal cavity. (See Fig. 1 for stages in normal intestinal rotation.) Many embryonic variants of the anomaly exist, ranging from nonrotation to reversed rotation.[1–5] In the most common type encountered in children, malrotation, the process of rotation is incomplete and the attachment of the mesentery of the midgut to the posterior abdominal wall is narrow and predisposes the midgut to volvulus (Fig. 2). Unless diagnosed promptly this condition can result in death or the short-bowel syndrome.
Fig. 1: Stages in normal intestinal rotation. A, gestational age 6 weeks; B, 8 weeks; C, 9 weeks; D, 11 weeks and E, 12 weeks (from Filston and Kirks,11 with permission).
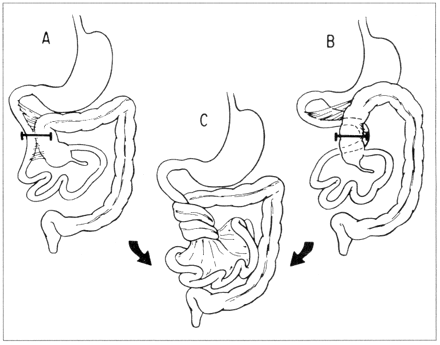
Fig. 2: Pathophysiology of midgut volvulus with malrotation. A narrow mesenteric attachment may cause midgut volvulus (from Filston and Kirks,11 with permission).
Epidemiology
Nonrotation occurs in approximately 1 in 500 live births.6 The true incidence of malrotation is unknown, however.[5, 7] Either sex can be affected with the anomaly. Approximately 60% of cases present in the first month of life, about 20% of cases between 1 month and 1 year of age, and the remainder present after the first year of life. Thereafter, the anomaly continues to manifest itself throughout childhood with decreasing frequency; it can occur in adults and even in the elderly.[8, 9]
Malrotation is an integral part of other major anomalies that do not allow for the return of the midgut to the peritoneal cavity (e.g., gastroschisis, omphaloceles and congenital diaphragmatic hernia)10 and is frequently associated with other congenital and acquired lesions of the gastrointestinal tract including Hirschsprung's disease, intussusception and atresia of the jejunum, duodenum and esophagus.[6, 11–13]
Clinical features
Neonates with intestinal malrotation present with bilious (green) vomiting caused by duodenal obstruction by congenital bands or midgut volvulus.[14, 15] Beyond the neonatal period, however, the clinical presentation of malrotation is variable and not as well defined.[7, 14–16] Symptoms that may be encountered in children after 1 month of age are listed in Table 1. Unfortunately, a physical examination is often unrewarding until late in the disease process when abdominal distention and other signs of peritonitis develop with the onset of ischemic necrosis of the volvulated bowel.17
Table 1: Possible presentations of malrotation beyond the neonatal period
Diagnosis
The upper GI study is key and very accurate for the diagnosis of intestinal malrotation.[18, 19] The landmark in the upper GI series is the position of the duodenojejunal flexure, and various radiographic patterns of duodenal malrotation have been described in detail to aid physicians in their diagnoses.19 Plain films of the abdomen, barium enema, abdominal ultrasound and CT scans are often not sufficiently reliable to rule out the diagnosis.[7, 11, 20–24] Rarely, laparotomy or laparoscopy may be required to make the diagnosis.[7, 25, 26]
Management
Patients who, on physical examination, present with a "surgical" abdomen and in whom the diagnosis of malrotation is suspected should be referred for immediate Ladd's procedure surgery.27 This consists of derotation of the midgut if volvulus exists and the division of the adhesions obstructing the duodenum and those that bind down and narrow the mesentery of the midgut. Gangrenous bowel, if encountered, is resected. The small bowel is placed in the right side of the abdomen and the colon in the left side. Appendectomy completes the procedure. If, however, the diagnosis is suspected on the basis of the patient's history and the physical examination is unremarkable, an upper GI study specifically designed to rule out malrotation should be arranged; if positive, urgent surgery should be planned. It is in these patients that the ticking bomb should be defused.
Key points
• Volvulus due to malrotation should always be kept in mind when assessing a child with abdominal pain and vomiting, particularly if the vomit is green. It cannot be ruled out on the basis of a negative abdominal examination or normal plain radiographs.
• Midgut volvulus may be present with chronic or intermittent symptoms.
• The best aids in making the diagnosis of malrotation are a careful and detailed history and an awareness of the anomaly.
• An upper GI study is very accurate in confirming the diagnosis.
• All children diagnosed with malrotation should be referred for a pediatric surgery consultation.
Thanks to Margaret Darling, Librarian, and Victoria Lemon, Library Technician, Kingston General Hospital, Kingston, Ont., for their valuable help.
Competing interests: None declared.
Acknowledgments
Want an easy way to check out what's in the next issue of CMAJ?
CMAJ now offers an email alert service. We'll send the table of contents for each issue of the journal to interested readers via email. The URL for each article is provided so that you can go directly to the full text online of any article that piques your curiosity.
Register on our Web site (www.cma.ca/cmaj) for this free service.
Footnotes
-
This article has been peer reviewed.
Reprint requests to: Dr. Ihab M. Kamal, Department of Surgery, Kingston General Hospital, 76 Stuart St., Kingston ON K7L 2V7; fax 613 545-3203; [email protected]