An 81-year-old woman with chronic schizophrenia was living alone in her home with support from a homemaker and watchful neighbours. An embolus developed in her distal femoral artery, likely a result of atrial fibrillation untreated due to her reclusiveness. She presented to the emergency department, a few days after the event, with severe pain in her left lower leg. An embolectomy was performed within a few hours, but there was already irreversible local ischemia. Although aware of the possibility of complications, including death from sepsis, the woman adamantly refused amputation. Her answers to questions were brief, but she had no obvious delusional thoughts. She had recently been active in caring for herself, maintaining her own home and helping neighbours with lawn care. She no longer took neuroleptics but had severe tardive dyskinesias from her past use. She was considered to have adequate decision-making capacity, and no amputation was undertaken. Referral was made to the palliative care team for management of her pain, which she described as severe.
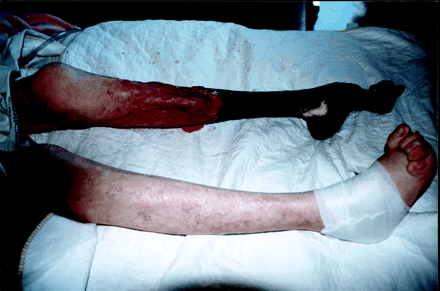
The pain was treated initially with a fentanyl patch, increasing to a dose of 125 μg/h, hydromorphone 6–9 mg for breakthrough pain and sufentanil 50–100 μg during dressing changes. Her extrapyramidal symptoms were treated with a very small dose of neuroleptic, with great improvement. Dry gangrene developed in her left lower limb over the ensuing weeks, and the area of interface between the healthy tissue and the dry gangrene developed putrefaction, which required débridement several times and intravenous ketamine therapy for pain relief during the procedure. Systemic sepsis never developed, but by 5 weeks after admission marked dry gangrene of the left leg developed below the knee (Figs. 1 and 2), and the woman continued to experience severe pain. After discussions with the palliative care team, she eventually consented to an above-knee amputation, which was performed without complication.
Figure 2. Photo: Courtesy: Romayne Gallagher
Figure 1. Photo: Photos courtesy of Romayne Gallagher
Gangrene often results from protracted ischemia of an affected body part1 and can arise because of atheroembolism, chronic atherosclerotic disease, vasculitis, trauma, frostbite and sickle cell disease.2 It is usually accompanied by extreme pain, although people with diabetes may have little or no pain because of neuropathy. Complications of gangrene include infection, sepsis, disseminated intravascular coagulation and death.3 If critical ischemia persists despite embolectomy or reperfusion using angioplasty or vessel grafting, amputation of the affected part is often necessary.4 Dry gangrene represents slow tissue breakdown without infection. The tissue ultimately becomes dessicated and mummified. Gangrene of this magnitude is rare except when patients refuse amputation.
This patient's case highlights how mental illness can complicate the detection and management of medical illness. Once adequate decision-making ability has been established, honouring the patient's autonomy remains a fundamental medical principle, but revisiting such decisions in the face of continuing, and potentially preventable, suffering is often necessary.
Romayne Gallagher Director, Division of Palliative Care University of British Columbia Vancouver, BC