Gastroesophageal reflux disease (GERD) affects 17–40% of North Americans1,2 and is increasing in incidence.3 Although some suspect that the rise in GERD is an artifact of improved diagnosis, others have postulated a relation to the declining rate of Helicobacter pylori-related gastritis, which may have protected against GERD by causing gastric hypochlorhydria.3
GERD is a risk factor for esophageal cancer. In a case–control study,4 people with esophageal adenocarcinoma were found to be much more likely to have had recurrent symptomatic GERD than age- and sex-matched members of the control group (odds ratio 7.7, 95% confidence interval [CI] 5.3–11.4).
Drugs, such as proton-pump inhibitors (PPIs), are highly effective in the treatment of GERD,5 but relapse is frequent after medications are discontinued,6 and long-term therapy is often required.
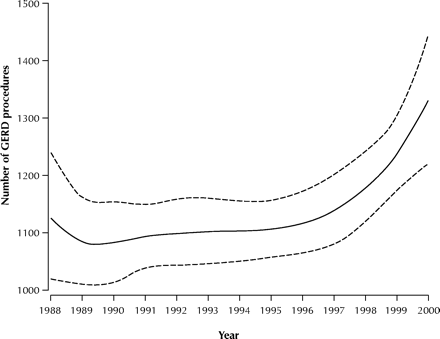
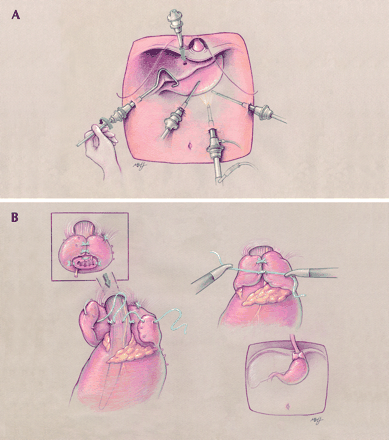
Surgical antireflux procedures for GERD, such as the Nissen fundoplication, represent an alternative to medical therapy. In recent years, minimally invasive or “laparoscopic” surgery (Fig. 1) has been used increasingly.7 The annual number of laparoscopic GERD operations is increasing in the United States8 and Canada.9 In Ontario, the number of GERD procedures declined between 1988 and 1990 (Fig. 2), remained stable until 1996, then increased rapidly and continued to rise through 2000.
Fig. 2: Trends in the use of surgery for gastroesophageal reflux disease in Ontario, 1988–2000. The solid line indicates the estimated annual number of antireflux operations (Canadian Classification of Procedures10 codes 54.76, 56.59 and 65.7) and the dashed lines indicate 95% CI. The annual number of procedures was modeled as a function of time using negative binomial regression.11 To produce a smooth curve, time (in fiscal years) was specified as a restricted cubic spline polynomial,12 with a “knot” at the year 1991 (allowing for a change in the rate of surgery at this point, when laparoscopic surgery13 became widespread). The analysis was done using SAS/GENMOD statistical software (SAS Institute, Cary NC).
Fig. 1: Laparoscopic Nissen fundoplication. This operation is done under a general anesthetic and takes 1–2 hours, and patients typically return home after an overnight hospital stay. Most patients are able to resume a normal diet and return to usual activity within 2 weeks. A: placement of ports for laparoscope and instrument access to the abdominal cavity. B: typical fundoplication procedure. The fundus of the stomach is wrapped around the lower esophagus, creating a 1-way valve that prevents the reflux of gastric contents into the esophagus without impeding the transit of swallowed food from the esophagus to the stomach. Most surgeons also repair the diaphragmatic crura (hiatal hernia). After a successful fundoplication, patients should have no heartburn, regurgitation or dysphagia and should be able to burp when necessary. Complications of surgery include mechanical disruption or migration of the fundoplication, recurrent reflux, dysphagia, inability to burp or vomit, bloating and diarrhea. Photo: Marisa Bonofiglio
The initial decline and subsequent rise in GERD surgery over the past decade reflects 2 important trends in therapeutic approaches to GERD. First, the arrival of PPIs in the marketplace in the late 1980s was associated with a sharp decline in GERD surgery. Second, the increased use of GERD surgery after 1996 was probably related to the widespread use of laparoscopy. The increased popularity of GERD surgery over the last few years suggests that patients and physicians consider laparoscopic GERD surgery an improvement over conventional open surgery and an effective alternative to long-term medical therapy for GERD.
Although the use of GERD surgery has increased, disagreement between surgeons and gastroenterologists persists regarding the role of surgery in patients with uncomplicated GERD. The predominant surgical perspective, that surgery is more effective than medical therapy and should be offered even to patients who respond well to PPIs,14 conflicts sharply with the medical perspective that surgery is ineffective or lacks durability in many patients and should be reserved for the rare patient who fails, or is unwilling to continue, drug therapy.15
Lack of consensus is not the result of a lack of prospective randomized trials; several have been conducted over the last 3 decades as both medical and surgical therapies have evolved. Conventional antireflux surgery proved far more effective than antacids and lifestyle modifications in 1975,16 modestly more effective than histamine type-2 receptor antagonists (H2RAs) in 199217 and perhaps marginally more effective than PPIs in 2001.18 The principal message from randomized trials is that, under ideal circumstances, modern surgical and medical management are both highly efficacious in the reduction of GERD symptoms.
However, surveys19 and administrative database analyses20,21 indicate that many people remain symptomatic or still take medications after GERD surgery. Also, there is no evidence that surgery can prevent esophageal adenocarcinoma. We know little about how patients are selected for GERD surgery and even less about the outcomes of surgery done outside specialized centres.
How can the conflicting perspectives regarding the effectiveness of GERD surgery be reconciled? Where does surgery fit into the treatment of GERD? Defining a role for surgery in the treatment of GERD will require more than information on the relative efficacy of surgical and medical therapy in randomized trials. We need data on the results of GERD surgery in clinical practice, where most patients will actually have surgery, rather than only results from the select institutions that have published most of the glowing reports. We need to be able to identify patients who might benefit most from surgery, perhaps with the use of preoperative esophageal 24-h pH monitoring.22
Finally, we need data from population-based studies to link variations in the practice of GERD surgery with outcomes. The outcomes of GERD surgery are highly dependent on operative technique. For this procedure, which has too often been a source of disappointment to patients and the gastroenterologists who referred them for surgery, we need to identify those aspects of surgical care that are most strongly associated with good results.
To further add to the confusion, several novel endoscopic interventions for GERD have recently emerged as alternatives to surgery, including plication23,24 and radiofrequency energy25,26 and polymer27 augmentation of the lower esophageal sphincter.
In the meantime, when should physicians send patients with GERD to a surgeon, and which surgeon should they send them to? The indications for surgery for uncomplicated GERD are still controversial. However, a reasonable approach is to limit surgical therapy to those patients with unequivocal evidence of pathologic GERD, who are highly motivated to have surgery and have a realistic understanding of its benefits and potential risks. A patient with classic GERD symptoms, who responds well to PPIs, should continue medical therapy unless he or she has a compelling reason to discontinue it (e.g., medication cost or the persistence of disabling symptoms, such as severe regurgitation, which do not respond as well to PPIs as heartburn). Finally, in the absence of better data on the outcomes of GERD surgery in usual clinical practice, it is reasonable to assume that the functional results will be better if the GERD surgery is done by a surgeon who has expertise in laparoscopic surgery and a special interest in the assessment of esophageal diseases and in managing the complications of GERD surgery.
Footnotes
-
This article has been peer reviewed.
Contributors: Dr. Urbach contributed substantially to the conception and design of the study and the analysis and interpretation of the data; he drafted the article and approved the final version. Drs. Ungar and Rabeneck contributed substantially to the conception and design of the study, revised the manuscript critically for important intellectual content and approved the final version.
Acknowledgements: We thank Muhammad Mamdani and Deanna Rothwell for their contributions to this paper. This research was supported in part by a Junior Faculty Research Grant from the Surgical Infection Society and by the physicians of Ontario through the Physicians Services Incorporated Foundation. Dr. Urbach is a Career Scientist of the Ontario Ministry of Health and Long-Term Care, Health Research Personnel Development Program. Dr. Ungar is a Canadian Institutes of Health Research New Investigator.
Competing interests: None declared.
Correspondence to: Dr. David R. Urbach, Institute for Clinical Evaluative Sciences, G Wing, Room 140, 2075 Bayview Ave., Toronto ON M4N 3M5; fax 416 480-6048; david.urbach{at}ices.on.ca