- © 2004 Canadian Medical Association or its licensors
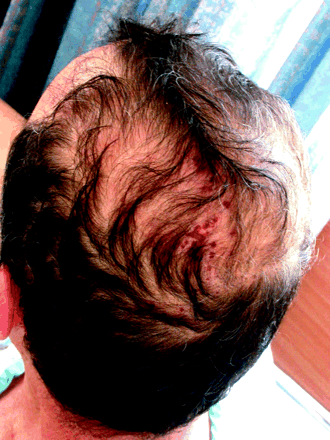
Three weeks after receiving a prosthetic aortic valve because of severe aortic stenosis, a 71-year-old man was admitted to hospital with a 3-day history of gradually increasing temperature. His temperature was 38.3οC, but the results of a physical examination were unremarkable. After 4 sets of blood cultures were obtained, ceftriaxone (1 g twice daily), vancomycin (1 g twice daily) and gentamycin (80 mg 3 times daily) were administered intravenously on the assumption that early infective endocarditis of the prosthetic valve was the most likely diagnosis. The patient's condition did not improve. His high temperature continued through his fourth day in hospital, accompanied by intense headache with no localizing complaints. The results of laboratory tests were strikingly normal, including a leukocyte count of 5.6 х 109/L with a normal differential and an erythrocyte sedimentation rate of 9 mm/h. Blood cultures yielded no growth, and transesophageal echocardiography showed no vegetation. On the fourth day after admission, the patient had nausea, vomited once and was mildly obtunded. Another physical examination revealed scalp lesions that had been hidden by the patient's hair (Fig. 1).
The skin lesions were unilateral, vesicular and pathognomonic of herpes zoster in dermatome C2 of the scalp. The patient's acute febrile illness with severe headache, nausea and obtundation was suggestive of meningitis. The normal leukocyte count and erythrocyte sedimentation rate were consistent with a viral cause rather than with infective endocarditis. Once the typical skin lesions of herpes zoster were revealed, varicella-zoster virus (VZV) meningitis was a likely association.
A lumbar puncture showed a protein level of 30.4 g/L, a normal glucose level and a leukocyte count of 15.1 х 109/L (85% mononuclear). The results of a real-time polymerase chain reaction assay were positive for VZV DNA. Antimicrobial therapy was discontinued, and acyclovir (10 mg/kg 3 times daily) was administered intravenously for 4 days, followed by oral acyclovir therapy (800 mg 5 times daily) for 6 days. There was no evidence of immunodeficiency, and the patient made a full, if slow, recovery.
Among 50 immunocompetent patients with herpes zoster who had no clinical signs of meningeal irritation or central nervous system involvement, more than half had cerebrospinal fluid abnormalities (e.g., pleocytosis, elevated protein levels, presence of VZV DNA) or lesions attributable to VZV on an MRI scan of the brainstem and cervical cord.1 Thus, extension of viral inflammation into the central nervous system commonly occurs among patients who have cutaneous herpes zoster. This may be subclinical or overt, as with our patient, who had symptoms of meningitis. Encephalitis, myelitis, radiculitis or other neurological syndromes may also occur.2 Reactivation of latent ubiquitous VZV infection usually occurs in patients who are immunosuppressed or elderly, but here virus reactivation may have been secondary to surgical and psychological stress,3,4 since it appeared 3 weeks after major surgery.
Ami Schattner Department of Medicine Addenbrookes Hospital University of Cambridge Cambridge, UK Joel Cohen Oren Zimhony Department of Medicine and Infectious Diseases Unit Kaplan Medical Center, Rehovot Hebrew University Hadassah Medical School Jerusalem, Israel