Abstract
Background: The timing of cardiovascular risks associated with the use of cyclooxygenase-2 (COX-2) inhibitors is unclear. Using data collected in a previous population-based cohort study of elderly people starting nonsteroidal anti-inflammatory drug (NSAID) therapy, we evaluated the temporal nature of the risk of a first myocardial infarction (MI) associated with the use of rofecoxib and celecoxib.
Methods: We identified people 66 years of age or older without previous MI who were currently taking rofecoxib and celecoxib using Quebec's computerized health databases (January 1999 to June 2002). Data on use and MI outcome were analyzed using a time-matched, nested case–control approach with rate ratios, comparing current users and non-users of rofecoxib and celecoxib in the year preceding the index date, estimated using conditional logistic regression.
Results: The risk of MI was highest following first-time use of rofecoxib (adjusted rate ratio [RR] 1.67, 95% confidence interval [CI] 1.21–2.30), with events occurring within a median of 9 (6–13) days after therapy was started. The risk increase for first-time use of celecoxib was not statistically significant (RR 1.29, 95% CI 0.90–1.83). Repeated exposure to rofecoxib was associated with a small but statistically nonsignificant delayed risk (RR 1.17, 95% CI 0.98–1.40), but no risk was seen with celecoxib (RR 0.97, 95% CI 0.82–1.14). Treatment duration was not associated with increasing risk for either agent. The risk remained elevated for the first 7 days after rofecoxib was discontinued (RR 1.23, 95% CI 1.05–1.44) but appeared to return to baseline between day 8 and 30 (RR 0.82, 95% CI 0.61–1.09).
Interpretation: A small proportion of patients using rofecoxib for the first time had their first MI shortly after starting the drug. This risk did not increase with the length of treatment and returned to baseline shortly after treatment was discontinued. More research is needed to identify those most susceptible to cardiotoxicity mediated by COX-2 inhibitor therapy.
Rofecoxib was withdrawn from the market on Sept. 30, 2004, after investigators in the Adenomatous Polyp Prevention on Vioxx (APPROVe) trial reported a 2-fold increase in cardiovascular toxicity after 18 months of use.1,2 In contrast, in the Vioxx Gastrointestinal Outcomes Research (VIGOR) study, a similar increase in risk was reported after only 9 months of treatment.3,4 Of interest, the risk curves in the latter study diverge after the first month of therapy.4 Two additional trials of cyclooxygenase-2 (COX-2) inhibitors have recently been published describing still different timelines for this association. In the Adenoma Prevention with Celecoxib (APC) trial,5 celecoxib was associated with a dose-dependent risk increase after 3 years of use, whereas the combination of injectable parecoxib followed by orally administered valdecoxib6 resulted in an increased risk after only 10 days of treatment. Although these variations in the timing of the risk could be due to differences in the populations, agents and dosing regimens studied, these observations nonetheless suggest the possibility of an early risk, at least in some populations. In addition, it is unclear how duration of use in a real-life setting contributes to this risk and for how long users of COX-2 inhibitors might remain at heightened risk after they discontinue therapy.
In a previous population-based cohort study of elderly people with no history of myocardial infarction (MI) initiating nonsteroidal anti-inflammatory drug (NSAID) therapy,7 we found an increased risk of acute MI among those currently taking rofecoxib. Here, using the data collected on current users of rofecoxib and celecoxib, we evaluated the temporal nature of the risk of a first MI.
Methods
The study cohort was the object of a previous report on NSAIDs and acute MI, where the methods are described in detail.7 In brief, the original study population, identified using the computerized databases of the universal health care programs of the province of Quebec, Canada, consisted of a random sample of 125 000 residents of the province, 66 years of age or older, who were dispensed an NSAID between Jan. 1, 1999, and June 30, 2002, and had been enrolled in the health plan for a period of at least one year. The date of the first such prescription was taken as cohort entry. To identify people starting NSAID therapy, we excluded those who had received such an agent in the year preceding cohort entry (n = 1193). In addition, we excluded those who had received ASA but no other NSAID (n = 1552) or had received prescriptions from 2 or more NSAID categories on the day of cohort entry (n = 153). The latter criterion made it possible to define mutually exclusive exposure groups. To study the risk of a first event, people with a hospital discharge diagnosis of MI (International Classification of Diseases, Ninth Revision [ICD-9] codes 410 and 412, all diagnostic fields) any time before cohort entry were also excluded (n = 8168). An additional 7 cohort members were excluded because their follow-up was less than 0 days (possible data errors). The remaining 113 927 people were followed until the earliest of the date of a first study end point, termination of health coverage (i.e., death or emigration), death, or Dec. 31, 2002 (end of study). The beneficiary file, prescription drugs, physician services, hospital admissions and vital statistics databases were linked, using a unique encrypted identifier, to provide individual-level information on health insurance coverage, demographic characteristics, medical and drug history, and vital status. This information was available for a minimum of 5 years preceding cohort entry as well as the duration of follow-up.
The study end point was a first hospital admission with a discharge diagnosis of acute MI (ICD-9 code 410), nonfatal or fatal, occurring any time after cohort entry. The date of admission was taken as the event date (referred to as the index date), and the MI was classified as fatal if the person died within 30 days of this date. The MI was considered a valid study end point if the hospital stay was 3 days or greater unless the person had been transferred to or from another institution or had undergone percutaneous coronary angioplasty.8
All NSAIDs available during the study period, including over-the-counter ASA and ibuprofen, were covered by Quebec's drug benefit program and available without prescribing restrictions. However, only agents obtained by prescription were captured by this database.
Since the results of our previous study demonstrated that the risk of MI was limited to those currently exposed to rofecoxib,7 the present analyses target these people (n = 239). Current users of celecoxib were also targeted (n = 287) because data published to date for this COX-2 have been conflicting. People for whom the duration of the last prescription dispensed in the year preceding the index date overlapped with this date were classified as current users; otherwise, people were considered past users. Those who did not receive at least one NSAID prescription in the year preceding the index date were considered non-users during this period. Current users of rofecoxib and celecoxib were categorized according to the following patterns of use: first-time use (the current prescription represented first exposure to that agent) and prevalent use (at least one additional prescription for the same agent had been received during follow-up). First-time users were further divided into naive users (no other NSAIDs had been dispensed during follow-up) or switchers (at least one other NSAID from a different category had been dispensed in addition to that defining current use). Prevalent users were further divided into users of monotherapy (only prescriptions for the same agent had been dispensed during follow-up) or switchers (at least one other NSAID from a different category had been dispensed in addition to 2 or more prescriptions for the COX-2 inhibitor that defined current use).
Two measures of cumulative exposure were used to assess the effect of duration of use in the year preceding the index date: total number of prescriptions dispensed for the same agent, and proportion of days exposed to the same agent, calculated as the sum of the number of days supplied with each prescription divided by 365 days. In this way, we were able to assess the effect of rofecoxib and celecoxib even among intermittent users. For the purposes of the analysis, the number of prescriptions dispensed was divided a priori into 4 categories: 1, 2–4, 5–8, and more than 8 prescriptions, whereas the proportion of days exposed was divided into quartiles.
The time since treatment discontinuation was calculated as the number of days between the date of the last available dose (based on the number of days supplied for the last prescription dispensed) and the index date. For the purposes of assessing the risk of MI after treatment cessation, this variable was divided a priori into 3 categories: 0–7 days, 8–30 days, and more than 30 days.
To study the effect of exposure to rofecoxib and celecoxib in the period preceding the event (i.e., the etiologically relevant time window) while simultaneously controlling for the potentially confounding effect of calendar time, we used a time-matched, nested case–control analysis of the cohort.9,10 This approach has been shown to provide unbiased estimates of the rate ratios that would be obtained from a traditional time-to-event analysis of the full cohort, with little or no loss in precision but significant gains in computational efficiency, particularly when analyzing time-varying exposures within large cohorts.11–13 This is not surprising, given that the primary difference between these 2 analytical techniques is the number of non-cases or control subjects that is retained in the analysis. With the standard time-to-event analysis, all people remaining at risk of the event (i.e., non-cases or control subjects) on the date of the case-event (i.e, the failure time that defines the “risk-set”) are retained in the analysis, whereas with the nested case–control approach only a random sample of the tens of thousands of controls are retained. The significant gains in computational efficiency are obtained from analyzing a subset of the non-cases and from analyzing exposure only in the etiologically relevant time period, thereby avoiding the need to program and evaluate a person's exposure status on a daily basis.
The index (event) date of each case was used to define the risk sets from which people who were still at risk of the event (i.e., non-cases or control subjects) were chosen. For each study end point (case), we randomly selected 20 control subjects matched on month and year of cohort entry and age (within one year) and assigned them the case's index date. Thus, age and follow-up time were identical for cases and control subjects in each risk set. We compared the risk of a first MI associated with various patterns and duration of use of rofecoxib and celecoxib as well as time since treatment discontinuation of users to that of non-users in the year preceding the index date (reference group). Rate ratios for these associations were estimated using conditional logistic regression to account for individual-level matching.14,15 These measures of association are equivalent to the hazard ratios that would be estimated from the corresponding Cox proportional hazards regression.16 Since our previous study results demonstrated no gain in precision with the use of a parsimonious model, all rate ratios were fully adjusted for the potentially confounding effects of conventional determinants of MI, other comorbid conditions, measures of health care utilization, and indices of comorbidity.17–19 With the exception of the latter 2, which were assessed in the year preceding the index date, all other covariates were assessed at baseline (year preceding cohort entry). We identified prognostic factors and comorbid conditions using both hospital admissions and drugs for specific corresponding treatments.
We tested the robustness of our definition of cumulative exposure using intermittent users by repeating the analysis using continuous users only.
This study was approved by the ethics boards of the province of Quebec (Commission d'accès à l'information du Québec) and the Royal Victoria Hospital, McGill University.
Results
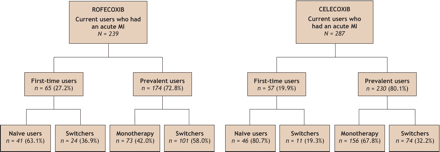
The original study cohort consisted of 113 927 people with a mean age of 75.2 (standard deviation [SD] 5.5) years at cohort entry who were followed for an average of 2.4 (SD 1.0) years. In the year preceding the index date, 70.7% of case and control subjects received at least one NSAID prescription; 18.9% were current users and 51.8% past users. Consequently, 29.3% were classified as non-users (reference category) during this period. Prescriptions had a mean duration of 28 (SD 17) days. Among those who were currently exposed, 239 rofecoxib and 287 celecoxib users had an acute MI (Fig. 1). There were 65 (27.2%) first-time users of rofecoxib, 41 (63.1%) of whom had not received other NSAIDs, including celecoxib, during follow-up (naive users). Among prevalent users of rofecoxib, 73 (42.0%) had used only rofecoxib (monotherapy) and 101 (58.0%) had received at least one other NSAID (switchers), the majority being celecoxib. A similar pattern of use was observed for celecoxib except for a lower proportion of first-time users and switchers. Since the number of first-time users for each drug was small and the majority were naive users, the pattern-of-use analysis was carried out on the combined group of first-time users.
Fig. 1: Patterns of use among current users of rofecoxib and celecoxib who had an acute myocardial infarction (MI).
The characteristics of case and control subjects are outlined in Table 1 according to their exposure status. As expected, regardless of exposure category, cases of MI were more likely to be male, have traditional risk factors and other manifestations of atherosclerosis, and be using ASA therapy. Case subjects also appeared generally sicker than control subjects. These differences were controlled for in the analysis. A comparison of rofecoxib or celecoxib cases according to our previously defined patterns of use revealed no clear or consistent differences between various patterns of the same agent with regard to their cardiovascular risk profile, general health status and dose prescribed (data not shown).
Table 1.
Compared with no use of NSAIDs in the year preceding the index date, the risk of an acute MI was highest after first-time use of rofecoxib (rate ratio [RR] 1.67, 95% confidence interval [CI] 1.21–2.30) (Table 2), with events occurring after a median of 9.0 (interquartile range [IQR] 6.0–13.0) days of a first prescription. The risk increase for first-time users of celecoxib was not statistically significant (RR 1.29, 95% CI 0.90–1.83). Repeated use of rofecoxib was associated with a small but statistically nonsignificant delayed risk increase (RR 1.17, 95% CI 0.98–1.40), with events occurring after a median of 7.8 (IQR 2.8–13.8) months for users of monotherapy (RR 1.20, 95% CI 0.92–1.57) and 6.2 (IQR 3.4–13.8) months for switchers (RR 1.16, 95% CI 0.93–1.45). No risk increase was observed following additional prescriptions of celecoxib (RR 0.97, 95% CI 0.82–1.14), regardless of previous use (RR 1.07, 95% CI 0.88–1.30 and RR 0.83, 95% CI 0.64–1.07, for monotherapy and switchers respectively). Past use of either agent was not associated with increased risk (RR 0.91, 95% CI 0.79–1.06 and RR 1.01, 95% CI 0.89–1.15, for rofecoxib and celecoxib respectively).
Table 2.
In all comparisons related to cumulative exposure, the risk of an acute MI did not increase with increasing exposure to either COX-2 inhibitor (Table 3). Indeed, the risk appeared to decrease as the length of treatment increased. Compared with no use of NSAIDs in the year preceding the index date, the risk for rofecoxib was highest for those having received only one prescription (RR 1.64, 95% CI 1.20–2.23), lower for 2–4 (RR 1.24, 95% CI 0.95–1.61) and 5–8 prescriptions (RR 1.31, 95% CI 0.97–1.76) and returned to baseline for those dispensed more than 8 prescriptions (RR 0.96, 95% CI 0.70–1.32). We observed a similar risk gradient when cumulative exposure was measured in terms of the proportion of days exposed in the year preceding the index date. Similarly, the risk for celecoxib did not increase over time. The results of the sensitivity analysis assessing duration of use among continuous users were essentially the same.
Table 3.
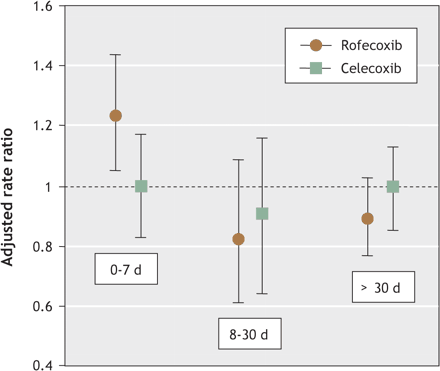
The risk of MI remained elevated for the first 7 days after rofecoxib was discontinued (RR 1.23, 95% CI 1.05–1.44) but appeared to return to baseline between day 8 and 30 (RR 0.82, 95% CI 0.61–1.09) (Fig. 2). The results for celecoxib were less informative since the risk of MI for these patients was not unequivocally increased.
Fig. 2: Adjusted rate ratios as a function of time after treatment is discontinuted.
Interpretation
In this large, population-based study of elderly people we demonstrated that the cardiovascular risks associated with the use of rofecoxib are more acute than previously recognized. About one-quarter of current users of rofecoxib who had an MI experienced this event within a few weeks of receiving their first prescription. This corresponds with the period of highest risk for this agent. The short-term use of celecoxib may also be associated with a clinically significant elevation in risk, but, given that statistical confirmation was lacking, further studies will be required to more completely assess this risk. Among those who “survived” their first exposure, repeated use was associated with a small but statistically nonsignificant delayed risk for some users of rofecoxib but not celecoxib. We also found that the risk of MI did not increase with increasing length of treatment and returned to baseline shortly after treatment was discontinued.
The statistically significant early risk observed with rofecoxib in our study is consistent with the early separation of the time-to-event curves shown in the VIGOR study.4 Trials of rofecoxib and celecoxib published to date have not reported a statistically significant early risk,2,4,5 although a significant risk with short-term exposure to valdecoxib in people at high risk has been observed.6,20 Differences between our results and those of these trials, as well as across trials, could be due to differences in populations, study end points, dosing regimens, agents studied and study methodology. Alternatively, since the risk curves for most of these trials began to separate well before a statistically significant risk increase could be detected, and given the small number of events observed in these trials, previous studies may have been underpowered to detect an early risk. Although we cannot directly compare our results to those of randomized trials, particularly in view of the older age of our study group, we nonetheless demonstrate the presence of an early risk of acute MI for rofecoxib, perhaps in part because of a considerably larger number of events. The overall validity of our results is enhanced by our previous observation of a clear risk for rofecoxib,7 which has been confirmed in multiple trials, and our overall equivocal results for celecoxib, which are consistent with the heterogeneity of trial results published to date.21,22
Our study results provide no conclusive evidence of an increased risk of MI for celecoxib. However, given that nearly 75% of patients receiving this drug were prescribed low doses (≤ 200 mg/d)7 and that the width of the 95% confidence interval does not exclude a clinically significant risk, further definitive studies are required. Our study results do provide support for the clinical equipoise required for further studies of celecoxib.
Three other observational studies provide data that are relevant to our findings.23–25 Two of these also observed a particularly high risk for new users of rofecoxib,23,25 although in the study by Ray and colleagues23 this was limited to 12 events among new users of high (> 25 mg) doses (RR 1.93, 95% CI 1.09–3.43). Johnsen and colleagues25 identified 39 cases of MI among new users of rofecoxib, which resulted in an increased early risk compared with non-users (RR 2.52, 95% CI 1.74–3.64). These investigators also observed a significantly increased risk for first-time users of celecoxib (RR 2.13, 95% CI 1.45–3.13). Neither study provided detailed information on time-to-event for either new users or prevalent users, and our larger sample permits a more precise estimate of the risk. In contrast, Mamdani and colleagues24 reported no excess risk for either agent, but their study evaluated a very different population than did ours. They excluded people who had received only one prescription or less than 30 days of therapy (first-time users in our study), censored those who switched agents (prevalent switchers in our study) and limited their follow-up to one year. In so doing, they may have limited their ability to detect any early risk following first exposure.
In our analyses, since exposure is censored by an event, the patterns of use and measures of cumulative exposure are indicative of a person's susceptibility to the cardiotoxic effects of COX-2 inhibitors, since only those who “survive” their first exposure can go on to receive subsequent prescriptions. The risk gradient that we observed for rofecoxib can be divided into 3 levels of susceptibility: high (patients who had their MI in association with their first prescription), moderate (patients who tolerated their first prescription but had an MI upon subsequent exposure) and low (patients who did not have an MI during 2.4 years of follow-up, despite receiving rofecoxib [i.e., exposed controls]). This pattern is consistent with the phenomenon of depletion of susceptible patients with repeated exposure26 and may explain the variations of MI risk over time that we observed. We did not find any clear differences in the cardiovascular risk profiles of these various groups nor in doses prescribed, which suggests that the delayed risk for rofecoxib cannot be explained by channelling bias. In addition, the risk increase was similar for prevalent users of monotherapy and prevalent switchers.
The limitations of our study need to be considered. We had limited statistical power to analyze prevalent users of either COX-2 inhibitors. Similarly, the analyses of cumulative exposure and duration of use were limited by the number of events in some strata, but in these analyses, the upper limits of the confidence intervals rule out the possibility of an increasing risk with long-term use. It is also possible that the risk of MI returns to baseline sooner than we were able to demonstrate, but we had insufficient numbers for a daily assessment. Only cases admitted to hospital could be included in our analyses, and consequently events such as silent MI or sudden death could have resulted in incomplete case ascertainment. Also, the intermittent use that occasionally accompanies NSAID therapy may have lead to misclassification of exposure. However, there is no reason to believe that ascertainment or exposure misclassification would have occurred differentially across the treatment groups being compared. Consequently, any resulting bias would be toward the null. We did not have information on smoking status, obesity, physical activity, family history or socioeconomic status, but several investigators have demonstrated that, in the context of assessing the risk of MI, unmeasured risk factors result in no or negligible bias toward the null.27–30 Finally, we were unable to account for the use of ASA and ibuprofen obtained without a prescription. However, as discussed previously,7 this source of bias is likely to be negligible and toward the null, thus leading to an underestimation of the true risk.
Although only celecoxib is currently available on the North American market, the results of this study are nevertheless important in understanding the nature of both past and present risks. These data also emphasize the need for early and proactive monitoring of adverse effects in the event that other COX-2 inhibitors are approved or even reintroduced, and provide new information regarding the period of monitoring required following cessation of treatment.
Our results offer new insights regarding the timing of the cardiovascular risks associated with the use of 2 COX-2 inhibitors. We demonstrated that, among elderly users of predominantly low doses of these agents, short-term use of rofecoxib is not without risk, and that risk of MI is not restricted to continuous users nor accentuated with longer-term use. Indeed, the risk of MI appears to decrease over time, despite repeated exposure, presumably owing to the depletion of susceptible people. More research is needed to identify those most susceptible to cardiotoxicity mediated by COX-2 inhibitor therapy and to investigate whether an early risk is present for celecoxib and in other populations.
Footnotes
-
An abridged version of this article is published in the May 23, 2006, issue of CMAJ.
This article has been peer reviewed.
Contributors: All of the authors contributed substantially to the conception and design of the study and the analysis and interpretation of data, drafted the article and revised it critically for important intellectual content and gave final approval of the version to be published.
Acknowledgements: This study was funded by a grant from the Canadian Institutes of Health Research (CIHR grant no. MOP62871), who had no role in the design, conduct, or reporting of the study or the decision to submit the manuscript for publication.
The interpretation and conclusions contained herein do not necessarily represent those of the government of Quebec or the agencies that provided the research data.
Competing interests: None declared.