Background and epidemiology: Although the Canadian territories and provinces had committed themselves to eliminating measles by 2005, hopes continue to be dashed by small eruptions, such as the 4 cases reported in November 2005 in the greater Toronto area. Certain members of our population continue to be susceptible to the measles virus: in particular, nonimmunized and incompletely immunized children born in Canada and abroad, and health care workers born after 1970 who are incompletely immunized — that is, who have received only a single dose of measles vaccine instead of the recommended 2 doses.
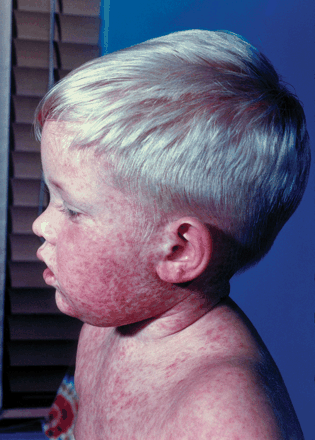
Figure. Boy with measles, on third day of rash. Photo by: US Centers for Disease Control and Prevention
People born before 1970 are probably immune from natural infection. At least 15% of children born after 1970 vaccinated with only 1 dose of MMR (measles, mumps and rubella) vaccine remain unprotected against measles, mostly because immunity wanes over a 5-year period after the first vaccination,1 which is why a 2-dose regimen vaccine schedule has been adopted in more recent years and augmented by mass vaccination “catch-up” programs — which inevitably miss members of the targeted cohort. According to 1 seroprevalence study2 conducted in the United States in the early 1990s, about 6%– 10% of new or current medical personnel lacked measurable antibodies in their serum and therefore were presumed to be susceptible to infection. Since cases of measles infection almost invariably involve health care, it is not surprising that historically, physicians have been twice, and nurses 8 times, as likely to acquire measles than adults who do not work in health care.
Measles virus is highly contagious, transmitted by inhalation of the virus by a susceptible individual. It is spread by airborne droplet nuclei or by close personal or direct contact with the nasal or throat secretions of infected people. The virus can remain active and infectious in the air or on surfaces for up to 2 hours. Measles is communicable from 1 day before the onset of prodromal symptoms to 4 days after onset of rash.3
Clinical management: The characteristic maculopapular rash appears first on the face and behind the ears of an infected person and spreads downward to the trunk and extremities. The incubation period can be 7– 18 days until onset of fever, then usually an additional 14 days (rarely, up to 21 days) until the rash appears. Prodromal symptoms, which may include cough, fever, coryza, malaise and conjunctivitis, occur 3–7 days before the rash, typically followed by Koplik spots that emerge on the buccal mucosa shortly before the rash begins.
All suspected cases of measles must be reported to public health authorities. Complications may result from viral replication or bacterial superinfection; they include otitis media, pneumonia, croup, diarrhea and encephalitis.
Laboratory testing should include serological tests of IgM and IgG antibody levels, both acute (within 7 days of rash onset) and convalescent (> 10 days after the acute specimen). In addition, it should include virus isolation from a sample collected within 7 days of rash onset: a nasopharyngeal swab or aspirate, a throat swab or a 50-mL urine sample.
Prevention and infection control: The 2002 Canadian Immunization Guide (available at www.phac-aspc.gc.ca/publicat/cig-gci) outlines the vaccine regimens recommended.
According to the Health Canada's 2002 infection-control guidelines,3 a health care worker may be considered immune to measles if she or he was born before 1970 or else has evidence of having had physician-diagnosed measles, 2 doses of live measles– containing vaccine or measles IgG. Susceptible health care workers who have been exposed to measles (e.g., have spent any time in face-to-face contact in an open area or being in a room with recirculated air within 2 hours of occupation by an infectious person) should be immunized with the measles vaccine (unless contraindicated) within 3 days of exposure. If more than 3 days have passed, an administration of immune globulin is recommended within 6 days of exposure, followed by immunization with vaccine 5 months later. Susceptible exposed health care workers should be excluded from work from the fifth day after their first exposure until the 21st day after their last exposure. Exceptions may be made for exposed workers with a history of a first dose of measles vaccine who received a second dose within 72 hours of exposure, or who test positive for measles antibody after 1 dose of vaccine.








