Eosinophilic esophagitis is becoming more common
Eosinophilic esophagitis is defined by esophageal dysfunction and eosinophilic infiltration of the esophageal mucosa refractory to treatment with proton pump inhibitors.1 The incidence has increased from 0.35 to 9.45 cases per 100 000 person-years over the last 30 years, and prevalence has been reported to be as high as 55 per 100 000 population.2
Eosinophilic esophagitis should be suspected in patients presenting with dysphagia or food bolus obstruction
Eosinophilic esophagitis is most common among young men (aged 20–40 years) and typically presents with dysphagia or food impaction, usually to meats. It can also be associated with atopy.1 Patients fitting this profile should be referred for endoscopy and mucosal biopsies.1
Endoscopic findings alone are not sufficient to make a diagnosis of eosinophilic esophagitis
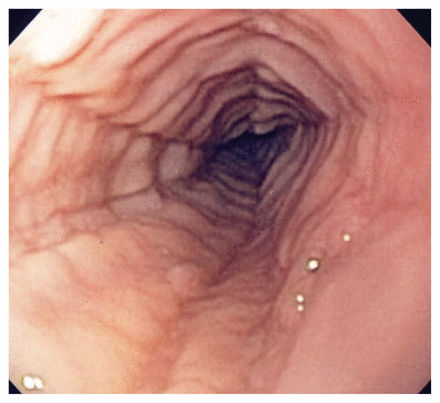
Although the endoscopic appearance of the disorder may be characterized by edema, concentric rings and furrows (Figure 1), a range of findings are possible, including normal endoscopy.1 Therefore, an endoscopic mucosal biopsy should be performed when eosinophilic esophagitis is suspected to determine if esophageal eosinophilia is present.1
Circular rings and furrows in the esophagus (trachealization) may be visible on endoscopy for eosinophilic esophagitis.
Proton pump inhibitors should be prescribed for a histologic finding of esophageal eosinophilia
The differential diagnosis for esophageal eosinophilia is broad and includes gastroesophageal reflux disease and a related entity, proton pump inhibitor–responsive esophageal eosinophilia. To exclude this latter entity, patients should have an eight-week trial of proton pump inhibitors followed by a repeat endoscopic mucosal biopsy; persistence of eosinophilia (defined as more than 15 eosinophils per high-power field) is suggestive of eosinophilic esophagitis.1
Topical steroids and elimination diets are the mainstays of therapy
Placebo-controlled randomized trials of budesonide and fluticasone administered orally have shown efficacy in improving symptoms and histologic findings in eosinophilic esophagitis.3,4 A six-food elimination diet (i.e., wheat, milk, eggs, soy, nuts and seafood) is based on the assumption that food allergies may contribute to the pathophysiology of eosinophilic esophagitis and also has shown efficacy in prospective studies.5 Skin prick testing is not useful generally in guiding dietary elimination.5
Footnotes
Competing interests: Samir Grover has received grants from Abbvie and Janssen, personal fees from Abbvie and Takeda, and is owner and has shares in Volō Healthcare, outside the submitted work. No other competing interests were declared.
This article has been peer reviewed.