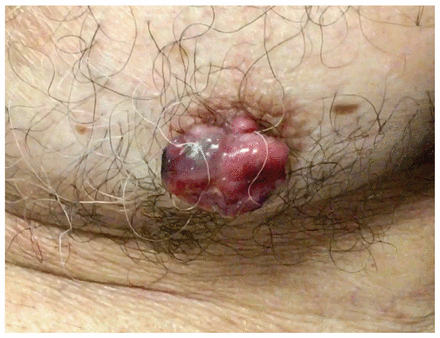
An 85-year-old man presented to our outpatient breast surgery clinic with an enlarging nipple mass and spontaneous bloody discharge for 1.5 years. The patient’s history included coronary artery disease and bilateral carotid endarterectomies, for which he was taking acetylsalicylic acid and clopidogrel. Because of his increasing nipple bleeding, he had stopped taking the clopidogrel of his own accord, but without resolution. He did not have changes of the contralateral nipple or skin lesions. He had no history of tobacco use, excessive or long-term alcohol use, or excessive sun exposure. Physical examination showed a 2-cm pedunculated mass over the nipple and associated nipple and areola enlargement (Figure 1). Excisional biopsy showed invasive ductal carcinoma that was positive for estrogen and progesterone receptors, and equivocal for HER2/neu. Mammography was negative and the patient underwent unilateral mastectomy with sentinel node biopsy (stage T4bN0M0). Given his age, comorbidities and low performance status, he was not a candidate for chemotherapy or radiation, but received tamoxifen.
Left nipple of an 85-year-old man with a pedunculated and erythematous mass and associated nipple and areola enlargement.
Male breast cancer represents 1% of breast cancer diagnoses and typically presents as a painless subareolar mass and can be mistaken for gynecomastia; however, nipple involvement, such as retraction, ulceration, bleeding or discharge, can be seen and confused for a primary skin lesion.1,2 Risk factors include increasing age, African-American race, processes causing elevated estrogen and genetic mutations.1–3 Male breast cancer is an indication for genetic testing, with BRCA2 seen in 4%–16% of cases.1,2,4 Imaging of choice is ultrasound if patients are younger than 25 years or mammography if older than 25.2 Patients tend to present at a later stage and undergo a modified radical mastectomy and axillary staging.2,3
Like female breast cancer, invasive ductal carcinoma is the predominant histological type in men and most are positive for estrogen and progesterone receptors; however, they are typically HER2/neu negative.2,5 Tamoxifen has been shown to be effective in improving recurrence-free and overall survival in men with tumours that are positive for estrogen and progesterone receptors. Aromatase inhibitors in men should be avoided unless used in conjunction with medical or surgical orchiectomy.3 There is a benefit in survival and recurrence rates with systemic chemotherapy.5
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.