Abstract
Background: Intracranial hemorrhage (ICH) after head injury is a concern among older adult patients on anticoagulation. We evaluated the risk of ICH after an emergency department visit for head injury among patients 65 years and older taking warfarin or a direct oral anticoagulant (DOAC) compared with patients not taking anticoagulants. We also evaluated risk of 30-day mortality and neurosurgical intervention among patients with ICH.
Methods: In this retrospective cohort study, we used population-based data of patients 65 years and older seen in an Ontario emergency department with a head injury. We matched patients on the propensity score to create 3 pairwise-matched cohorts based on anticoagulation status (warfarin v. DOAC, warfarin v. no anticoagulant, DOAC v. no anticoagulant). For each cohort, we calculated the relative risk of ICH at the index emergency department visit and 30-day mortality. We also calculated the hazard of neurosurgical intervention among patients with ICH.
Results: We identified 77 834 patients with head injury, including 64 917 (83.4%) who were not on anticoagulation, 9214 (11.8%) who were on DOACs and 3703 (4.8%) who were on warfarin. Of these, 5.9% of patients had ICH at the index emergency department visit. Patients on warfarin had an increased risk of ICH compared with matched patients on DOACs (relative risk [RR] 1.43, 95% confidence interval [CI] 1.20–1.69) and patients not on anticoagulation (RR 1.36, 95% CI 1.15–1.61). We did not observe a difference in ICH between patients on DOACs compared with matched patients not on anticoagulation. In patients with ICH, 30-day mortality did not differ by anticoagulation status or type. Patients on warfarin had an increased hazard of neurosurgery compared with patients not on anticoagulation.
Interpretation: Patients on warfarin seen in the emergency department with a head injury had higher relative risks of ICH than matched patients on a DOAC and patients not on anticoagulation, respectively. The risk of ICH for patients on a DOAC was not significantly different compared with no anticoagulation. Further research should confirm that older adults using warfarin are the only group at higher risk of ICH after head injury.
Falls resulting in a head injury are common among older adults.1,2 Advanced age and anticoagulation are thought to be associated with an increased risk of intracranial hemorrhage (ICH) after a head injury.3–5 With the aging population and increasing use of anticoagulants, older patients on anticoagulation are commonly seen in the emergency department after a head injury. The Canadian CT Head Rule suggests that patients presenting to the emergency department with a minor head injury who are older than 65 years should undergo head imaging to rule out ICH.6 This clinical decision tool did not include patients on anticoagulation; however, a clinical policy from the American College of Emergency Physician suggests computed tomography (CT) imaging for these patients.7
Before 2010, warfarin, a vitamin K antagonist, was the oral anticoagulant used most commonly in North America. Since then, direct oral anticoagulants (DOACs) have been approved for various indications including treatment of venous thromboembolism, prevention of venous thromboembolism after arthroplasty, and stroke prophylaxis in patients with atrial fibrillation. Unlike warfarin, DOACs either directly inhibit clotting factors II (e.g., dabigatran) or X (e.g., apixaban, rivaroxaban, edoxaban). Although more expensive than warfarin, DOACs are attractive alternatives because of their simplified dosing and predictable therapeutic effect, and now account for most anticoagulant prescriptions.8–10
Previous research suggests that patients on anticoagulation, particularly those on warfarin, are at increased risk of ICH and may have worse outcomes after a head injury than those not on anticoagulants. 5,11 Fewer data exist on the risk of traumatic ICH among patients on a DOAC, and there is a paucity of research in real-world, population-based cohorts comparing the risk of ICH between anticoagulants after a head injury. Therefore, the objective of this study was to evaluate the risk of ICH among older patients who present to the emergency department with a head injury and compare this risk by type of anticoagulation. Secondary outcomes included the hazard of neurosurgical intervention and 30-day mortality among the subgroup of patients with ICH.
Methods
Study design and setting
We conducted a retrospective cohort study of population-based health data in Ontario from 2016 to 2018. We obtained patient information from province-wide health administrative databases held at Ontario Health.
Data sources
We obtained information regarding emergency department visits from the Canadian Institutes of Health Information National Ambulatory Care Reporting System (CIHI-NACRS) and the electronic Canadian Triage and Acuity Scale (eCTAS) databases. The NACRS database contains abstracted data on all emergency department visits in Ontario. The eCTAS is an electronic triage system introduced in Ontario emergency departments in 2016 that is now used in more than 90% of emergency departments across the province. We also used CIHI’s Discharge Abstract Database (DAD), which contains information on all acute care hospitalizations and inpatient surgical procedures in the province, the Ontario Health Insurance Plan (OHIP) database, which contains all physician billings for medically necessary care, and the Registered Persons Database, which contains information on the deaths of all Ontario residents, including out-of-hospital deaths. We used the Ontario Drug Benefit database, which contains all medical prescriptions covered by the provincial government, to identify anticoagulant status at the time of the emergency department visit. For patients older than 65 years, the Ontario government covers the costs for all warfarin prescriptions, DOAC prescriptions for stroke prevention in atrial fibrillation and DOAC prescriptions during the initial 6 months of anticoagulation treatment for venous thrombosis. Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.210811/tab-related-content, contains further description of databases. We linked patient records using a unique, encoded identifier.
Study population
Using NACRS and eCTAS, we identified patients 65 years and older with a valid OHIP number who presented to the emergency department with a triage complaint of head injury or trauma, identified by electronic searching of free-form text and manual review of eCTAS comment fields in patients triaged via eCTAS between January 2016 and December 2018. We included only the first emergency department visit for a head injury during the study period. We excluded visits to emergency departments that were not open 24 hours per day, visits to urgent care centres (as these are typically centres treating lower-acuity patients than an emergency department, usually without access to CT imaging), patients who left the emergency department without being seen or left against medical advice, and patients who died en route to the emergency department. We excluded patients prescribed heparin during the 7 days before the emergency department visit. We also excluded patients on dialysis because these patients are not likely to receive DOACs.
Exposure
The main exposure variable was anticoagulation status, categorized as no anticoagulation, warfarin or DOAC (i.e., apixaban, dabigatran, edoxaban or rivaroxaban). To be classified as an anticoagulant user, patients must have had a filled prescription for an anticoagulant that covered the 2 days before the index emergency department visit for the head injury (see Table e1 in Appendix 1 for codes used to identify medications).
Outcomes
The primary outcome of this study was ICH, as identified during the index emergency department visit. We included all types of intracranial bleeds. To identify ICH, we used discharge diagnoses in NACRS, which uses the International Statistical Classification of Diseases and Related Health Problems, 10th Revision (ICD-10) codes. For patients with an ICH diagnosed at the index visit, we evaluated secondary outcomes of interest, including 30-day mortality and neurosurgical intervention within 90 days (see Tables e2 and e3 in Appendix 1 for outcome definitions).
Covariates
We chose the covariates included in the statistical models a priori based on potential predictors or confounders of ICH or the risk of head injury. Covariates included demographics (i.e., age, sex), comorbidities (i.e., Charlson Comorbidity Score, atrial fibrillation, cancer, coronary artery disease, chronic obstructive pulmonary disease, congestive heart failure, dementia, diabetes, hypertension, liver failure, multiple sclerosis, Parkinson disease, renal failure, seizure disorder, ischemic stroke or transient ischemic attack, hemorrhagic stroke, venous thromboembolism), clopidogrel prescription in the last 7 days and hospital type (i.e., small, community or academic) (see Table e4 in Appendix 1 for covariate definitions).
Statistical analysis
We compared baseline patient characteristics by anticoagulant status using frequencies for categorical variables and medians (with interquartile range) for continuous variables. We used propensity score matching to create 3 pairwise-matched cohorts based on anticoagulation status (warfarin v. DOAC, warfarin v. no anticoagulant, DOAC v. no anticoagulant). We estimated the propensity score using logistic regression, where exposure status was regressed on the covariates. We matched patients in each cohort on the logit of the propensity score using a 1:1 without replacement approach and a caliper width of 0.2 of the standard deviation of the logit of the propensity score.12 We evaluated balance in baseline covariates for each cohort using standardized differences and considered standardized differences of less than 0.10 between groups as well matched.12 When evaluating outcomes in patients with ICH, we rematched patients within this subgroup. For each cohort, we calculated the average treatment effects of patients who were treated, and the relative risk (RR) and corresponding 95% confidence intervals (CIs) of ICH and 30-day mortality in patients with an ICH. We used Cox proportional hazards models, censoring for death, to determine the hazard of neurosurgical intervention among patients with an ICH, with a robust variance estimator to account for the matched nature of the sample.13 We conducted all analyses using SAS 9.4.
Ethics approval
The study was compliant with privacy procedures at Ontario Health and received approval from the Research Ethics Board at Sinai Health.
Results
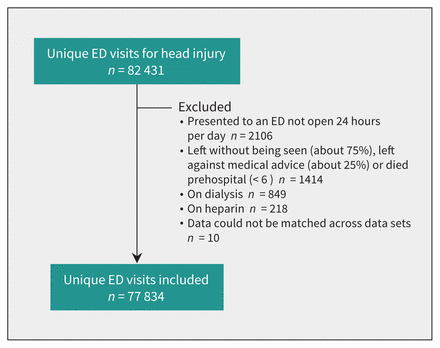
We included 77 834 emergency department visits made by patients 65 years and older for a head injury (Figure 1). We excluded 12 076 repeat visits to the emergency department. Of the included patients, 64 917 (83.4%) had not filled a prescription for anticoagulation, 9214 (11.8%) had a prescription for a DOAC and 3703 (4.8%) had a prescription for warfarin at the time of the emergency department visit (Table 1). Overall, 75% of patients had CT imaging of their head; more than 90% of patients on either warfarin or a DOAC received CT imaging. Of the total, 4620 (5.9%) patients had an ICH at the index emergency department visit; 3772 (5.8%) patients not on an anticoagulant had an ICH, whereas 303 (8.2%) patients on warfarin and 545 (5.9%) patients on DOACs had an ICH. Among patients with an ICH, 394 (8.5%) underwent neurosurgical intervention within 90 days, and 591 (12.8%) died within 30 days. See Table e5 in Appendix 1 for standardized differences in the baseline characteristics in each pairwise cohort before matching.
Study flow diagram. Note: ED = emergency department.
Baseline characteristics of patients 65 years and older seen in the emergency department with a head injury
After propensity score matching, there were 3654 pairs (98.7% of warfarin patients matched) in the warfarin versus DOAC cohort, 3634 pairs (98.1% of warfarin patients matched) in the warfarin versus no anticoagulation cohort and 8329 pairs (90.4% of DOAC patients matched; see Table e6 in the Appendix 1 for characteristics of unmatched DOAC patients in this cohort) in the DOAC versus no anticoagulation cohort. Patients in each matched cohort were well balanced, with standardized differences less than 0.10 (Table 2). Patients on warfarin had an increased risk of ICH compared with matched patients on DOACs (RR 1.43, 95% CI 1.20–1.69) and patients not on anticoagulation (RR 1.36, 95% CI 1.15–1.61). There was no difference in ICH in those on DOACs compared with matched patients not on anticoagulation (RR 0.94, 95% CI 0.83–1.05).
Balance in covariates and standardized differences in matched pairwise cohorts
Patients with an ICH were then re-matched for each cohort. We removed covariates for which there were fewer than 10 patients with the condition (see Table e7 in Appendix 1 for balance in covariates). The cohort of patients on warfarin versus those with no anticoagulation had 2 covariates that were not well balanced, which were then adjusted for in the Cox proportional hazards model. For patients with ICH, relative risk of 30-day mortality was not significantly different in any matched cohorts (Table 3). Patients on warfarin had an increased hazard of neurosurgical intervention compared with matched patients not on anticoagulation (hazard ratio [HR] 1.67, 95% CI 1.10–2.54). Patients on warfarin did not have a significantly different hazard of neurosurgical intervention compared with those on a DOAC (HR 1.36, 95% CI 0.93–2.01), nor did patients on a DOAC compared with those not on anticoagulation (HR 1.13, 95% CI 0.80–1.58).
Outcomes in propensity score matched cohorts
Interpretation
In this population-based study of 77 834 patients aged 65 years and older seen in the emergency department for a head injury, 5.9% had an ICH at the index emergency department visit. We found DOAC users had a similar risk of ICH to matched patients not prescribed anticoagulation, and warfarin users had an increased risk of ICH compared with matched patients on DOACs and those not on anticoagulation.
Our observed rate of ICH of 5.9% was lower than the 21% observed among patients older than 65 years in the derivation study of the Canadian CT Head Rule, which reported that 75 of 356 patients had a “clinically important brain injury” on CT.6 This study included patients with blunt head trauma resulting in loss of consciousness, amnesia or disorientation. Our study had different inclusion criteria; the difference in findings may reflect that we included more patients with minor injuries that did not result in bleeds. In the validation of the NEXUS head CT rule, 8.9% of patients older than 65 years (331 of 3705 patients) had a clinically significant injury on CT.14 The incidence of ICH we found is similar to that of a 2020 systematic review that reported a 5% incidence of ICH in patients older than 65 years who had a fall.15 A meta-analysis of 4080 patients on anticoagulants (98.3% on warfarin) and with head injuries reported an 8.9% incidence of ICH, which is similar to the 8.2% incidence of ICH we found in patients on warfarin.5
Our findings are consistent with those of previous studies showing an increased risk of ICH among patients on warfarin compared with those not on anticoagulants.16–18 Less evidence has compared the risk of traumatic ICH between DOACs and warfarin; however, studies evaluating specific DOACs compared with warfarin suggest a lower risk of ICH in patients on a DOAC compared with warfarin.19–24 The ROCKET-AF,19 RE-LY20 and ARISTOTLE21 studies of patients with atrial fibrillation showed that the risk of ICH (spontaneous and traumatic) was lower with rivaroxaban, dabigatran and apixaban, respectively, compared with warfarin. Our study is one of the largest studies evaluating risk of ICH in anticoagulant users after head trauma, and our results suggest that patients on DOACs seen in the emergency department do not have an increased risk of traumatic ICH compared with patients not using anticoagulants. In contrast, those taking warfarin had a higher ICH risk compared with both patients on DOACs and those not on anticoagulation. Future prospective research should test the hypothesis that warfarin users are the only group at higher risk of ICH. If validated, the implications of our findings are considerable, including a potential reduction in neuroimaging among head-injured patients on DOACs, which could translate into shorter emergency department visits and cost savings for the health care system.
There is conflicting evidence surrounding differences in mortality rates by anticoagulation status. The RE-LY trial reported higher mortality rates after ICH among patients on warfarin compared with dabigatran.22 In a study of 2245 patients with nontraumatic ICH, patients on warfarin had higher rates of in-hospital deaths compared with DOACs.25 Similarly, a registry study of more than 140 000 patients with spontaneous ICH found that DOAC use was associated with a lower rate of in-hospital mortality compared with warfarin.26 However, a meta-analysis of patients with traumatic brain injury found that in-hospital mortality rates were not different for patients on DOACs compared with patients on warfarin. 27 Other studies have shown an increased risk of death among patients on warfarin compared with patients not on anticoagulation after a traumatic ICH.28,29 We did not find significant differences in 30-day mortality rates between matched patients on warfarin, DOAC and no anticoagulation with ICH; however, the number of deaths was small and we were underpowered to detect small differences in mortality rates.
Previous literature on neurosurgical intervention after ICH by anticoagulation status has been inconsistent. In a meta-analysis of 2622 patients with traumatic ICH, no overall difference was observed in the risk of neurosurgical intervention among patients using a DOAC compared with warfarin.27 In patients with an ICH, we found an increased hazard only of neurosurgery among patients on warfarin compared with those not on anticoagulation. The need for surgical intervention among patients on warfarin may be related to the hemorrhage itself. Previous studies have described a larger hemorrhage volume and increased progression of bleed in patients on warfarin compared with those not on anticoagulation. 30,31 Because of the small number of patients undergoing intervention, we may not have been able to detect small differences in neurosurgical intervention among other groups.
Limitations
We only included patients with head injuries seen in the emergency department, so we cannot draw conclusions about those who did not seek medical attention or who visited their family doctor. We identified patients by triage complaint, which may not capture every patient with a head injury (e.g., if patients also presented with a serious medical condition or other major trauma, or had a different presenting complaint recorded at triage). Therefore, the total number of head injuries is likely higher than our sample and we cannot comment on whether our findings are applicable to this group. Our study used administrative data, which has the potential for misclassification bias if there were coding errors for the variables used, including the main diagnosis. However, many studies have used these databases and found good agreement between chart reviews and databases for mandatory variables32 and the main emergency department diagnosis for various diseases.33–35 We classified anticoagulant use based on patients having filled government-reimbursed prescriptions. This assumes patients took medication as prescribed, consistently rather than intermittently. We were unable to obtain laboratory data to evaluate coagulation markers. Furthermore, it is possible we misclassified patients as not being anticoagulant users if their medication was covered by private health insurance. This likely results in some misclassification of anticoagulation use, which would be expected to underestimate the real effect of current anticoagulant use on the risk of ICH. We were not able to account for the use of over-the-counter acetylsalicylic acid, which may affect bleeding outcomes. We were not able to evaluate outcomes such as disability among patients who had an ICH. Finally, this study was retrospective, and although we adjusted for many comorbidities and conducted propensity score matching, residual differences may exist between groups from unmeasured confounders.
Conclusion
Older patients on warfarin who present to the emergency department with a head injury have an increased risk of ICH compared with matched patients on a DOAC and patients not on anticoagulation. Patients on a DOAC and those with no anticoagulation do not have a significantly different risk of ICH. Future research is needed to confirm that warfarin users are the only group at higher risk of ICH. These findings could substantially affect the need for neuroimaging after head trauma among patients on DOACs.
Acknowledgements
The authors acknowledge Ontario Health (Cancer Care Ontario) for their in-kind support. They also thank Brooke Filsinger, Andrea Mackesy, Lisa Ellison, Tamer Ahmed and Steve Scott at Ontario Health for their assistance in obtaining the study data.
Footnotes
Competing interests: Clare Atzema reports payment for presentations from the Canadian Association of Emergency Physicians, the Cardiovascular Virtual Update Congress and the Emergency Medicine Update. Kerstin de Wit reports a research grant from Bayer, and Bjug Borgundvaag reports a grant from the Canadian Institutes of Health Research, outside the submitted work. No other competing interests were declared.
This article has been peer reviewed.
Contributors: Keerat Grewal, Clare Atzema, Kerstin de Wit, Sunjay Sharma, Bjug Borgundvaag and Shelley McLeod were involved in study conceptualization. Keerat Grewal, Clare Atzema, Peter Austin, Shelley McLeod were involved in data analysis plan. Nicole Mittmann, Bjug Borgundvaag, Shelley McLeod helped obtain data. Keerat Grewal conducted the analysis. All authors contributed to data interpretation. Keerat Grewal and Shelley McLeod prepared the first draft of the manuscript. All authors revised it critically for important intellectual content and approved the final manuscript. Keerat Grewal and Shelley McLeod agree to be accountable for all aspects of the work.
Data sharing: The data set from this study is held securely in coded, deidentified form at Sinai Health. The data sharing agreements prohibits us from making the data set publicly available. The full data set creation plan and underlying analytic code are available from the authors upon request, understanding that the computer programs may rely upon coding templates or macros that are unique to the dataset and are therefore either inaccessible or may require modification.
Funding: The study was funded by the Canadian Association of Emergency Physicians through an Emergency Medicine Advancement Fund research award. The funding agreement ensured the investigators maintained control over the study design, methods and interpretation of the results. Keerat Grewal was supported by a CanVECTOR fellowship award; the CanVECTOR Network receives grant funding from the Canadian Institutes of Health Research (Funding Reference: CDT-142654). Clare Atzema and Peter Austin were supported by Mid-Career Investigator Awards from the Heart and Stroke Foundation. Kerstin de Wit was supported by grants from Hamilton Health Sciences Foundation and the PSI Foundation. Bjug Borgundvaag was supported by the Department of Family and Community Medicine at the University of Toronto and the Sinai Health System.
Disclaimer: Parts of this material are based on data and information provided by Ontario Health (Cancer Care Ontario), and includes data received by Ontario Health (Cancer Care Ontario) from the Canadian Institute for Health Information (CIHI), the Ministry of Health (MOH), and ICES. The opinions, reviews, view and conclusions reported in this publication are those of the authors and do not necessarily reflect those of Ontario Health (Cancer Care Ontario), CIHI, the MOH, and/or ICES. No endorsement by Ontario Health (Cancer Care Ontario), CIHI, the MOH, and/or ICES is intended or should be inferred.
- Accepted July 15, 2021.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/