Pre-exposure prophylaxis (PrEP) is a highly effective modality for HIV prevention that can be prescribed by generalists.
Pre-exposure prophylaxis should be offered to patients who are at high risk of HIV exposure, including gay, bisexual and other men who have sex with men (GBM), women reporting condomless intercourse with partners of confirmed or unknown transmissible HIV status and persons who inject drugs and share injection equipment.
Once daily PrEP (tenofovir disoproxil fumarate/emtricitabine [TDF/FTC] or tenofovir alafenamide fumarate/emtricitabine tablets) is approved by Health Canada.
On-demand TDF/FTC can be prescribed to gay, bisexual and other men who have sex with men and has similar efficacy.
The Canadian guideline details protocolized monitoring for PrEP follow-up including HIV screening, screening for sexually transmitted infection and renal monitoring.
Incidence of HIV has been rising in Canada. The Public Health Agency of Canada estimated 2242 new HIV infections in 2018, which highlights the need for comprehensive prevention strategies. 1 Pre-exposure prophylaxis (PrEP) is an important means of preventing acquisition of HIV; however, it is underused.2–4 Although generalists (e.g., family physicians, nurse practitioners and general internists) could play a vital role in implementing PrEP, a recent small survey of general practitioners in Nova Scotia found that most did not prescribe PrEP.5 We describe PrEP for HIV and discuss current uptake and potential barriers to its use, as well as the approach to prescribing PrEP (Box 1).
Evidence used in this review
We conducted a PubMed search of original research and review articles published from January 2017 to January 2021, using the terms “HIV PrEP” or “HIV pre-exposure prophylaxis” and “Canada” or “Canadian.” We used this time frame because the Canadian pre-exposure prophylaxis (PrEP) guideline was released in 2017. In addition, we reviewed the current Canadian and American guidelines on PrEP. We selected relevant studies and manually searched their references for additional articles.
What is pre-exposure prophylaxis for HIV?
Pre-exposure prophylaxis for HIV is the use of antiretroviral agents by people who are HIV negative that begins before and continues after potential HIV exposures to prevent acquisition of HIV.6,7 It can be taken daily or on demand before an anticipated exposure.6,7 Pre-exposure prophylaxis is best used as part of a comprehensive HIV and sexual health strategy that includes harm-reduction education, screening for sexually transmitted infections (STIs), reproductive and mental health care, and attention to co-occurring conditions such as hepatitis B and depression.
How effective is pre-exposure prophylaxis for HIV?
High-quality evidence from randomized controlled trials (RCTs) and observational studies has shown that use of daily PrEP among gay, bisexual and other men who have sex with men (GBM) is associated with almost 100% prevention of HIV acquisition when adherence is high.8–10 High-quality evidence has shown that efficacy of PrEP is as high as 95% for heterosexual exposure, depending on adherence.11–13 A 2013 RCT involving people who inject drugs in Bangkok, Thailand, (the Bangkok Tenofovir Study) showed 48.9% efficacy of PrEP but had very low adherence among participants; efficacy increased to 74% among a subgroup of participants who had detectable antiviral levels.14 Research in all populations has shown the importance of adherence for efficacy, and observational data have shown high effectiveness in real-world settings, with breakthrough infections being uncommon.15 Uptake of PrEP has been clearly associated with a decline in HIV diagnoses at the population level.16,17
The Intervention Préventive de l’Exposition aux Risques avec et pour les Gays (IPERGAY) trial showed that on-demand PrEP is efficacious in GBM, with a reduction in risk of acquiring HIV of 86%; only 2 breakthrough infections occurred in 2 participants who were not adherent to the prophylaxis regimen.6,18 Participants took a median of 15 pills per month and, although a post hoc analysis showed similar efficacy in participants using fewer than 15 pills per month, there remain modest data on effectiveness in those with more sporadic exposures.18,19
Who should be offered pre-exposure prophylaxis for HIV?
The risk of HIV acquisition depends on the likelihood that the contact person has transmissible HIV infection and on the exposure type (Box 2). Several studies have shown that a person who is HIV positive, is receiving antiretroviral therapy, and has a viral load of less than 200 copies/mL cannot transmit HIV to sexual partners.20–22 The indication for PrEP is based on the likelihood of high-risk exposure to transmissible HIV.6
Risk of HIV transmission by exposure6
Risk that a person has transmissible HIV infection
Substantial
HIV positive with viral load > 40 copies/mL
HIV status unknown but from a population with high HIV prevalence
Low but nonzero
HIV positive with viral load < 40 copies/mL with concomitant sexually transmitted infection present at time of exposure
Negligible or none
Confirmed HIV negative
HIV positive with confirmed viral load < 40 copies/mL and no sexually transmitted infection at time of exposure
HIV status unknown, general population
Risk of HIV transmission by exposure type from HIV-positive source
High
Receptive anal intercourse
Needle sharing
Moderate
Insertive anal intercourse
Receptive vaginal intercourse
Insertive vaginal intercourse
Low
Giving oral sex
Receiving oral sex
Oral–anal contact
Sharing sex toys
Blood on compromised skin
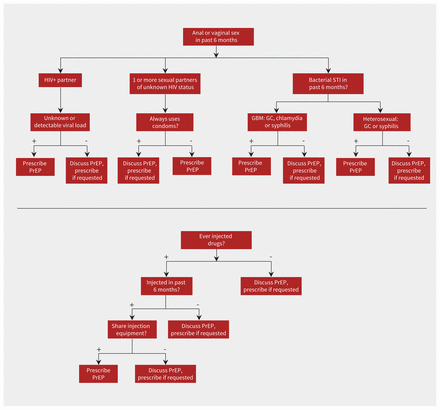
Guidelines have been published to assist with identifying patients who may benefit from PrEP (e.g., from the Centers for Disease Control and Prevention [CDC]; Figure 1); however, these recommendations should be considered in the context of the patient’s individual risk factors and local epidemiology, and should be seen as a tool rather than rigid instructions. Shared decision-making with the patient is essential, and people should not be denied PrEP if they self-identify as being at risk for HIV outside of current guidance.6,7
Pre-exposure prophylaxis (PrEP) algorithm, based on the CDC guideline.6 Note: CDC = Centers for Disease Control and Prevention, GBM = gay, bisexual and men who have sex with men, GC = gonorrhea, STI = sexually transmitted infection.
Although Canadian and American guidelines on PrEP differ slightly, in general, PrEP is recommended for persons engaging in condomless anal or vaginal sex either with partners of unknown HIV status or with partners with known transmissible HIV (i.e., detectable or unknown viral load).6,7,23 Additional risk factors such as previous use of HIV post-exposure prophylaxis and specific bacterial STIs (Figure 1) are also useful in identifying people at elevated risk of HIV exposure.6,7,23 Tools for risk stratification (e.g., HIV Incidence Risk Index for men who have sex with men [HIRI-MSM]) are available to assist health care providers in identifying patients who are at elevated risk of HIV.6
On-demand PrEP can be considered as an effective alternative in GBM or transgender women who do not want to take daily pills or who have few potential exposures per month.6 It is not currently recommended in other populations owing to a lack of evidence.
Canadian and American guidelines have recommended PrEP in patients who share injection equipment.6,7 Risk stratification tools for people who inject drugs have been developed, such as the Assessing the Risk of Contracting HIV in Injection Drug Users (ARCH-IDU) screening tool.24
How is pre-exposure prophylaxis prescribed and monitored?
Currently available daily PrEP regimens (Table 1) include the once-daily combination tablets tenofovir disoproxil fumarate/emtricitabine (TDF/FTC) or tenofovir alafenamide fumarate/emtricitabine (TAF/FTC).6,7,23,25 On-demand PrEP (also known as “2-1-1” PrEP) is 2 tablets taken 2–24 hours before unprotected sex, followed by 1 pill daily until 48 hours after the last sexual exposure.6,7 Long-acting formulations of PrEP have also been developed, such as injectable cabotegravir, which is administered every 8 weeks. Although not yet approved for PrEP in Canada, it may in the future be considered for people who prefer injections over daily tablet regimens.26
Prescribers should complete an assessment when PrEP is started and every 3 months while the patient is taking prophylaxis (Table 2).6,7 Assessments should include reviewing whether the patient has ongoing indications for PrEP and discussing strategies for adherence. Quarterly HIV testing is important because ongoing PrEP use in patients with undiagnosed HIV can lead to drug resistance.27
Pre-exposure prophylaxis should be part of comprehensive sexual health care and HIV prevention including education, STI screening and reproductive health, as well as harm reduction and mental health assessment and management.
Both formulations of PrEP can be associated with mild gastrointestinal adverse effects, but these symptoms rapidly subside and rarely cause patients to stop PrEP.28 Tenofovir disoproxil fumarate is associated with a small risk of renal toxicity and a slight decrease in bone mineral density, both of which are usually reversible when the medication is stopped.28,29 Tenofovir alafenamide fumarate has been associated with higher rates of triglyceride elevation and weight gain than TDF.30 For most people at risk of HIV, the efficacy of HIV prevention outweighs the risks of these adverse effects.
Tenofovir disoproxil fumarate/emtricitabine can be prescribed for PrEP in people who are pregnant or breastfeeding.6,7,23 This drug has been used widely for treatment of HIV in pregnancy with no evidence of adverse outcomes, and the 2021 guideline update from the CDC and a 2019 analysis of PrEP implementation among pregnant and postpartum women in Western Kenya reported no difference in pregnancy outcomes in women receiving perinatal PrEP.7,31
Tenofovir disoproxil fumarate/emtricitabine and TAF/FTC also have activity against hepatitis B virus (HBV) and, if they are stopped, patients with HBV infection may have hepatitis flares.6,7 This underscores the importance of baseline HBV testing, and vaccination for patients who are not immune to HBV. When HIV PrEP is started in patients with chronic HBV infection, it also functions as HBV treatment and requires guideline-driven monitoring in consultation with an experienced HBV provider if needed.6,7
Adolescents who weigh at least 35 kg can also safely take PrEP using TDF/FTC or TAF/FTC.7
What proportion of eligible patients in Canada are taking pre-exposure prophylaxis?
National surveillance of PrEP use in Canada is not undertaken, which makes patterns of use difficult to quantify. However, use is likely increasing. Pre-exposure prophylaxis was used off label until Health Canada approved daily TDF/FTC for PrEP in 2016, lower-cost generic versions became available in 2017 and the Canadian guideline was released in 2017.2,6,32
A study of prescription data in 8 provinces estimated that 9657 patients were receiving PrEP in 2018, about 98% of whom identified as male.32 Between 2017 and 2019, eligibility for PrEP by Canadian guidelines for GBM in major urban centres ranged from 44.9% to 58.1%, yet only 14.5%–21.8% had used PrEP.3 Even among GBM at elevated risk of HIV, only 24.6% were taking PrEP in 2017.4
In 2018, women made up 25% of new HIV diagnoses yet accounted for only 2% of PrEP users in Canada.1,32 Minimal data on uptake in other populations are available.
What barriers exist for patients in accessing pre-exposure prophylaxis?
The basic prerequisite for PrEP uptake is recognition that a patient is at risk of acquiring HIV. However, HIV risk is often underappreciated by both patients and providers. Because most efforts to increase uptake of PrEP in Canada and elsewhere have focused on GBM, risk is particularly underappreciated in other groups, such as women and people who inject drugs, people for whom there are few validated tools for risk assessment.33,34
Even among patients who know that they are at elevated risk of acquiring HIV, low awareness about, and low acceptability of, PrEP pose additional challenges; systemic discrimination often exacerbates the problem. For instance, among GBM, being “less out” or not identifying as gay have been linked to lower PrEP awareness, knowledge and uptake owing to discomfort with disclosure, fear that PrEP will “out” them or having less access to PrEP awareness campaigns.3,4,35 Identifying as Black, Indigenous or other racialized groups has also been associated with lower awareness and knowledge regarding PrEP.4,36 A 2022 analysis based on interviews with Black GBM in Toronto reported that community outreach programs did not focus on PrEP and, even when advertised, PrEP was often inadequately explained or seemed to encourage condomless sex.37 Many communities have expressed concerns around pervasive stigma that associates PrEP with “promiscuity.”37
Potential users must find a provider with adequate knowledge, comfort in discussing sexual health and a willingness to prescribe PrEP. Both lack of access to a primary provider and little experience with prescribing PrEP among many generalist physicians contribute to this problem; these challenges are exacerbated in rural or remote areas.2–5 Provider biases regarding who they expect to adhere to PrEP can also lead to inequities in access. The frequency of visits and laboratory tests for monitoring are burdensome for both patients and providers.
Affordability is one of the primary barriers to using PrEP in all populations.2,37 Although all provinces and territories provide some amount of coverage for PrEP, who qualifies and how much is covered varies (https://hivclinic.ca/wp-content/uploads/2022/02/2022-Jan_ARV-access-for-PrEP.pdf). Even perceptions of treatment unaffordability may prevent patients from seeking PrEP and learning if they are covered.37
What strategies can be used to increase appropriate use of pre-exposure prophylaxis?
Clinicians should start discussions about risk of acquiring HIV and PrEP as part of routine preventative health care to reduce reliance on patients self-identifying that they are at risk. In particular, discussion about PrEP should be considered standard care for those who present with bacterial STIs or undergo STI testing.6,7,38,39 This requires creating a safe space to discuss HIV risk by explicitly combating homophobia and stigma related to sexual and substance use behaviours.4 Providers can also increase acceptability of PrEP to patients by addressing misconceptions of PrEP as being an intervention solely for gay or highly sexualized people.4,34,37
As a relatively simple primary prevention intervention, PrEP can be delivered in routine primary care. However, prescribing PrEP requires provider knowledge, comfort with discussing sexual health and cultural competence in working with historically marginalized populations.40 Guidelines such as those provided by the CDC can assist clinicians in prescribing PrEP, and easy-to-access Continuing Medical Education modules have been developed to train community-based primary care providers (e.g., https://hivprevention.talentlms.com/shared/start/key:LZGIDNHR).5–7,35
Systemic solutions are also needed for patients who do not get identified within primary care. For example, automated systems can identify and expedite referral to PrEP clinics for patients with risk factors that may otherwise be missed, such as through incorporating predictive models into inpatient electronic medical records or automated referrals when STIs are reported to public health.4,41,42
The pool of potential providers can also be expanded by harnessing the highly protocolized nature of PrEP to task shift from physicians to other professionals working under a medical directive. Successful examples include nurse-led community or sexual health clinics and pharmacist-led delivery and mobile drop-in clinics that offer low-barrier PrEP.4,41,43
Technology can also be used to improve access to PrEP in less-resourced settings or to increase convenience of appointments via telehealth or virtual care to connect with providers in more well-resourced areas.43 Community-based peer-support programs can increase engagement based on trust and culturally informed perspectives for marginalized communities.37,43 Public health leaders also have a responsibility to raise awareness about PrEP as a safe and effective preventive health strategy for many populations.
Among the most important interventions to increase PrEP uptake is reducing financial barriers. Clinicians should be aware of options for drug coverage that are available in their jurisdiction and advocate to extend public coverage where not universally available. On-demand PrEP may also reduce cost-related barriers.
Conclusion
Pre-exposure prophylaxis is an important modality for preventing acquisition of HIV that can approach 100% efficacy among people who adhere well to treatment. It should be employed as part of a comprehensive strategy for HIV prevention, and generalist physicians can play an important role in increasing access and uptake. Guidelines provide easy-to-follow protocols for identifying eligible patients, prescribing medications and ongoing monitoring. Barriers to PrEP include underestimation of HIV risk in some populations, lack of PrEP awareness, inadequate access to those who will prescribe PrEP and medication costs (Box 3). Pervasive stigma and structural inequities in access to knowledge and care exacerbate these gaps. Health care providers can help close these gaps by increasing their knowledge about PrEP, routinely starting PrEP discussions with patients and advocating for system changes such as medication coverage.
Unanswered questions
What are evidence-based tools to help identify women and people who inject drugs who would most benefit from pre-exposure prophylaxis (PrEP) in a high income country such as Canada?
How can uptake and awareness of PrEP be increased in communities that are already facing barriers to health care access?
What are the optimal strategies to increase knowledge of and comfort in suggesting PrEP among health care providers?
Acknowledgement
The authors acknowledge that they live and work on the traditional territory of many Indigenous people, including the Abenaki, Anishnaabe, Attawandaron, Chippewa, Haudenosaunee, Huron/Wendat, Kanien’kehà:ka, Lūnaapéewak and Mississaugas of the Credit.
Footnotes
Competing interests: Jean-Guy Baril has received consultant fees from ViiV Healthcare, Merck and Gilead, and honoraria for lectures from Merck and Gilead. He is also a member of the HIV and HCV advisory boards for the Ministère de la santé du Québec. Mia Biondi has received speaking fees from Gilead Canada and is an independent contractor with Omega Specialty Nurses. Darrell Tan holds a Tier 2 Canada Research Chair in HIV Prevention and STI Research. No other competing interests were declared.
This article was solicited and has been peer reviewed.
Contributors: Darrell Tan conceived the review. Amanda Hempel performed the literature review and drafted the manuscript. All of the authors edited the manuscript, reviewed the manuscript critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: Jean-Guy Baril has received grants from GSK, Merck and Gilead (paid to his institution). Darrell Tan has received grants from AbbVie (in-kind support to his institution for investigator-initiated research), Gilead (support to his insitution for investigator-initiated research) and GSK (support to his institution for conducting industry-sponsored clinical trials).
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/