A 19-year-old woman presented to our oral and maxillofacial clinic with localized swelling of the mucosal aspect of the right side of her lower lip that had been present for several weeks. It was solitary, intermittently swollen and painless but annoying. It increased in size after accidental biting. The patient was an otherwise healthy nonsmoker.
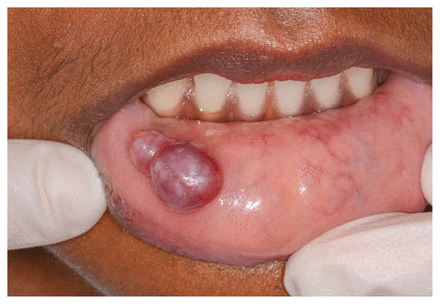
On examination, the lesion was bi-lobed, translucent and bluish, with intact overlying mucosa (Figure 1). On palpation, it was fluid filled and nontender and we could detect no lymphadenopathy. We diagnosed 2 adjacent mucocoeles (mucous cysts) and surgically excised the lesions. Histopathology showed extravasation mucocoeles. Subsequent healing was uneventful, with no recurrence.
Photograph of a 19-year-old woman with 2 adjacent mucocoeles, showing a bi-lobed, translucent and bluish lesion and swelling of the lower lip.
Mucocoeles of the minor salivary glands are common oral lesions with a prevalence of 2.5 cases per 1000 people and are caused by obstruction of an excretory duct.1 About two-thirds of mucoceles occur in patients younger than 30 years.1 Mechanical trauma such as lip biting is a likely cause, sometimes associated with bruxism. This can result in retention of mucus within the duct (mucous retention cyst) or, more commonly, the formation of a pseudocyst in the submucosa (mucous extravasation cyst). Differential diagnoses include hemangioma, fibroma, abscess, lymphangioma, epidermoid cyst and lipoma.
The lower lip is the most common location, but mucocoeles also occur in the cheek mucosa, floor of the mouth, ventral tongue and palate. Superficial mucocoeles sometimes resolve spontaneously, whereas deeper mucocoeles tend to persist. If persistent, excision of both the cyst and the adjacent minor salivary glands is usually curative, minimizes the risk of recurrence and allows histopathologic confirmation. Cryotherapy or the use of a CO2 laser can also be effective, with minimal scarring.2 A small risk exists of sensory disturbance to the lip vermilion. The recurrence rate is low, but appears higher in younger patients.3
Clinical images are chosen because they are particularly intriguing, classic or dramatic. Submissions of clear, appropriately labelled high-resolution images must be accompanied by a figure caption. A brief explanation (300 words maximum) of the educational importance of the images with minimal references is required. The patient’s written consent for publication must be obtained before submission.
Acknowledgements
The authors thank Ian Chambers, Australian maxillofacial surgeon, for proofreading the manuscript.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/