Abstract
Background: The prevalence of tuberculosis infection is critical to the design of tuberculosis prevention strategies, yet is unknown in Canada. We estimated the prevalence of tuberculosis infection among Canadian residents born abroad.
Methods: We estimated the prevalence of tuberculosis infection by age and year of migration to Canada for people from each of 168 countries by constructing country-specific and calendar year–specific trends for annual risk of infection using a previously developed model. We combined country-specific prevalence estimates with Canadian Census data from 2001, 2006, 2011, 2016 and 2021 to estimate the overall prevalence of tuberculosis infection among foreign-born Canadian residents.
Results: The estimated overall prevalence of tuberculosis infection among foreign-born people in Canada was 25% (95% uncertainty interval [UI] 20%–35%) for census year 2001, 24% (95% UI 20%–33%) for 2006, 23% (95% UI 19%–30%) for 2011, 22% (95% UI 19%–28%) for 2016 and 22% (95% UI 19%–27%) for 2021. The prevalence increased with age at migration and incidence of tuberculosis in the country of origin. In 2021, the estimated prevalence of infection among foreign-born residents was lowest in Quebec (19%, 95% UI 16%–24%) and highest in Alberta (24%, 95% UI 21%–28%) and British Columbia (24%, 95% UI 20%–30%). Among all foreign-born Canadian residents with tuberculosis infection in 2021, we estimated that only 1 in 488 (95% UI 185–1039) had become infected within the 2 preceding years.
Interpretation: About 1 in 4 foreign-born Canadian residents has tuberculosis infection, but very few were infected within the 2 preceding years (the highest risk period for progression to tuberculosis disease). These data may inform future tuberculosis infection screening policies.
Tuberculosis disease is the leading cause of death by a single infectious agent worldwide, surpassed only by COVID-19 in 2020 and 2021.1 Tuberculosis disease is preceded by tuberculosis infection, which has traditionally been identified by testing for immunoreactivity to the causative agent, Mycobacterium tuberculosis. An estimated 23% of the world’s population has tuberculosis infection. Depending on sociodemographic and medical characteristics, the World Health Organization (WHO) suggests that 5%–10% of persons with tuberculosis infection will progress to tuberculosis disease, the cause of 1.6 million deaths in 2021.1,2
The WHO has established targets for tuberculosis disease elimination in low-incidence countries such as Canada, with a goal to reduce the annual incidence of tuberculosis disease to 1 case per million population. The incidence of tuberculosis disease in Canada declined steadily through the second half of the 20th century but has remained essentially unchanged over the last decade. Despite a previous target of reducing tuberculosis incidence in Canada to 3.5 per 100 000 by 2015, it remained at 4.8 per 100 000 in 20213,4 The lack of further progress toward elimination is the result of epidemiologic shifts without the implementation of new prevention strategies.
In Canada, foreign-born residents bear 80% of the burden of tuberculosis disease, despite representing only 23% of the population. 3,5,6 Tuberculosis disease among foreign-born residents occurs largely because of the progression of tuberculosis infection acquired within their countries of origin.5 Preventive treatment for tuberculosis is highly effective at preventing progression to tuberculosis disease. However, implementation of this preventive treatment is limited in Canada.7,8 Widespread screening and treatment programs for tuberculosis infection would likely be cost-prohibitive9 and could result in the provision of treatment to large numbers of people who may derive minimal benefit.10,11
Instead, targeting screening to those at highest risk of tuberculosis infection would improve cost-effectiveness and health gains for treated people.12 However, except for a small minority of people with documented risk factors for progression, no systematic screening and treatment programs or policies exist for migrants. Unlike in the United States, no Canadian population-based surveys include testing for tuberculosis infection. The prevalence of tuberculosis infection among Canada’s foreign-born population is thus unknown. To support the design and implementation of tuberculosis prevention programs, we sought to estimate prevalence and patterns of tuberculosis infection among foreign-born residents.
Methods
We used modelled estimates of the annual risk of tuberculosis infection — the probability of becoming infected with M. tuberculosis each year — from countries from 1889 through 2021 to estimate the probability of tuberculosis infection according to year of birth, age at year of immigration (obtaining permanent residence) and country of origin among people who had immigrated to Canada. We integrated Canadian Census data from 2001, 2006, 2011, 2016 and 2021 to estimate the prevalence of tuberculosis infection among permanent residents and foreign-born Canadian citizens during each census year. We did not include temporary workers, visitors and students.
Data sources
Census data
We obtained Canadian Census data detailing the number of permanent residents and foreign-born Canadian citizens living in Canada (hereafter, collectively referred to as foreign-born residents) from Statistics Canada for years 2001, 2006, 2011, 2016 and 2021.13 These data include the number of permanent residents and citizens from each country (Appendix 1, Table S1 and Table S2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.230228/tab-related-content), further grouped into categories based on age and year of immigration (Appendix 1, Table S1). Within each age and year of immigration category, we assumed a uniform distribution of people for each specific age and year of immigration.
Annual risk of infection data
We adapted a previously published approach to obtain country-specific estimates for the annual risk of tuberculosis infection. In brief, we estimated historic annual risks of infection (ARI) using 2 data sources. We used in-country tuberculin skin test surveys to directly estimate the annual risk of infection, where available (Appendix 1, Table S3).14,15 When tuberculin skin test surveys were unavailable, we estimated historic annual risks of infection based on World Health Organization (WHO) estimates of the prevalence of smear-positive tuberculosis and the documented relationship between smear-positive pulmonary tuberculosis prevalence and annual infection risk,16–18 while accounting for the impact of HIV infection in each country.14 We used the δ method to propagate uncertainty and estimate variance around estimates of annual risk of infection.19 We excluded countries from analysis if their population was below 500 000 people, if they could not be matched with data on the incidence of tuberculosis disease or if neither tuberculin skin test survey data nor adequate tuberculosis disease prevalence data were available.
Definitions
We categorized the annual incidence of tuberculosis disease per 100 000 person-years in country of origin into groups of 0–9, 10–49, 50–99, 100–199 and 200 or higher based on WHO estimates of global incidence of tuberculosis disease from 2021 (Appendix 1, Table S2).20,21 We used estimates from 2021 as this was the final census year analyzed, and data on the incidence of tuberculosis disease before the year 2000 are considered unreliable. 22 We calculated year of birth as the census year minus reported age. Year of immigration was the year in which individuals acquired permanent residence. We calculated age at immigration as the year of immigration minus the year of birth. We categorized age during each census year and age at immigration as younger than 15 years, 15–34 years, 35–54 years, 55–74 years or 75 years or older.
Data analysis
To account for uncertainty around estimates of annual risk of infection, we used a Gaussian process regression model to simulate 200 log-scale trends of annual risk of infection for each country and calendar year from 1934 to 2014, conditioned on the available data. Gaussian process regression models use a Bayesian approach whereby the certainty of 1 variable is used to reduce uncertainty in others, based on an understanding of the covariance between 1 or more variables. In time-series modelling studies, Gaussian process models can efficiently address interactions between covariates and account for time-varying covariates, more than methods such as general linear mixed effect models and generalized estimating equations.23,24
We used estimates of the annual risk of infection for 1934 for previous years back to 1889 and a random walk with drift time series projection to estimate the annual risk of infection from 2014 to 2021. In total, this yielded annual risk of infection estimates and uncertainty ranges for every country and year from 1889 to 2021.
For each of the 200 sampled log-scale trends of annual risk of infection, we generated probabilities of tuberculosis infection for each combination of country, birth year and migration year (Appendix 1, Figure S1 for further details). First, we calculated annual risks of tuberculosis infection, assuming risks were uniform among people from the same country, birth year and migration year, by exponentiating each log-annual risk of infection. Second, we integrated annual risks of infection for each country, birth year and migration year to estimate the cumulative risk of infection for each census year (i.e., 2001, 2006, 2011, 2016 and 2021) — accounting for annual risks of infection in the country of origin before immigration, as well as within Canada after immigration. Since precise calendar dates of immigration were unknown, we assumed that the average date of arrival for each cohort was the midpoint of the calendar year, resulting in the estimated risk of infection during the year of migration representing an average of the risk of infection in the country of origin and in Canada. Finally, using the cumulative risk of infection, we calculated the probability of tuberculosis infection for each combination of birth year, country of origin and immigration year.
For each census year, by summing relevant strata, we estimated the number of foreign-born residents living in Canada overall and by subgroup. These subgroups reflected categorization by age at immigration, age during each census year, incidence of tuberculosis disease per 100 000 people in country of origin and the most frequent countries of origin across census years. Using our estimates of the probability of tuberculosis infection, we estimated the prevalence of tuberculosis infection for each census year overall, for each of these subgroups and by time since immigration. For the census year 2021 only, we estimated the prevalence of tuberculosis infection in Ontario, Quebec, Alberta and British Columbia (the 4 largest immigrant-receiving provinces), and in the rest of Canada. We also estimated the prevalence of tuberculosis infection acquired within the preceding 2 years, as the 2 years after new infection represent the highest-risk period for progression to tuberculosis disease.
We calculated the point estimate and the 95% uncertainty intervals (UIs) for tuberculosis infection estimates as the 50th, 2.5th and 97.5th percentile, respectively. We tested differences in median prevalence of tuberculosis infection across census years using the Kruskal–Wallis test. We performed all analyses using R (version 4.0.2).
Ethics approval
This study involved the use of publicly available, deidentified, aggregate data. Approval by a research ethics board was not required.
Results
Population composition
During census year 2021, 8.4 million Canadian permanent residents and citizens had been born outside Canada. This represented an increase of 3 million (56%) since 2001. The median age of those born outside Canada in each census year from 2001 to 2021 was 46 (interquartile range [IQR] 32–58) years, 47 (IQR 32–61) years, 47 (IQR 32–61) years, 48 (IQR 33–62) years and 50 (IQR 39–63) years, respectively; 67% had immigrated before age 35 years in 2021 (Table 1). In all census years, 52% of those born outside of Canada were female and 48% were male. Between the 2001 and 2021 census years, the number of foreign-born residents from Europe decreased in absolute number and proportion, while those from Asia increased in both absolute number and proportion. In line with these trends, the proportion of foreign-born residents from countries with an incidence of tuberculosis disease of 200 per 100 000 per year or higher increased from 15% to 27% between 2001 and 2021, while the proportion from countries with a tuberculosis incidence of less than 10 per 100 000 decreased from 38% to 24% during the same period.
Composition of the foreign-born Canadian population in census years 2001–2021
Over the 2001 to 2021 census years, 7 countries or jurisdictions (China, India, Italy, Philippines, the United Kingdom, the US and Hong Kong) were consistently among the 10 most frequent places of origin. All except the US, Italy and the UK have an incidence of tuberculosis disease of 50 per 100 000 people or higher, while the incidence is 200 per 100 000 people or higher in India and the Philippines (Appendix 1, Table S2). In the 2021 census year, Pakistan, Vietnam and Iran also ranked among the 10 most common countries of origin (Table 2); all 3 have an incidence of tuberculosis disease incidence greater than 100 per 100 000 people.
Number and proportion of foreign-born Canadians from top 10 countries of origin by census year
Estimated prevalence of tuberculosis infection
We included 168 countries of origin in our analyses of tuberculosis infection prevalence, and excluded 50 countries (Appendix 1, Table S4). The total number of people living in Canada from these 50 countries combined was 66 670 (1.3% of all foreign-born residents) to 83 180 (1.1%) in the 2001 and 2021 census years, respectively.14 The overall estimated prevalence of tuberculosis infection among foreign-born residents did not change substantially over time. It was 25% (95% UI 20%–35%), 24% (95% UI 20%–33%), 23% (95% UI 19%–30%), 22% (95% UI 19%–28%) and 22% (95% UI 19%–27%) in census years 2001, 2006, 2011, 2016 and 2021, respectively.
Between 2001 and 2021, the estimated prevalence of tuberculosis infection decreased among foreign-born residents from India, China, the Philippines and the US (p < 0.0001), decreasing most substantially for China (Table 3).
Estimated prevalence of tuberculosis infection among foreign-born residents from the 7 most frequent countries or jurisdictions of origin by census year
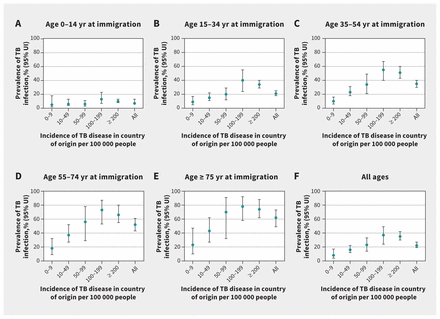
In 2021, the estimated prevalence of tuberculosis infection varied from 8% (95% UI 4%–17%) among people from countries with an incidence of tuberculosis disease lower than 10 per 100 000 people to 35% (95% UI 30%–42%) among people from countries with an incidence of 200 per 100 000 people or higher. Similarly, prevalence increased markedly with age at immigration, ranging from 7% (95% UI 6%–13%) for those who became permanent residents when younger than 15 years to 62% (95% UI 49%–73%) for those who became permanent residents when aged 75 years or older (Figure 1). Findings were generally similar in earlier census years (Appendix 1, Table S5).
Estimated prevalence of tuberculosis infection among foreign-born residents aged (A) 0–14 years, (B) 15–34 years, (C) 35–54 years, (D) 55–74 years and (E) 75 years and older at immigration, and (F) among all foreign-born residents according to 2021 tuberculosis disease incidence per 100 000 people in country of origin. Note: TB = tuberculosis, UI = uncertainty interval.
In 2021, 93% of all permanent residents and citizens born outside Canada resided in Ontario, Quebec, Alberta or BC (Appendix 1, Table S6). In these 4 provinces, the estimated prevalence of tuberculosis infection increased with age at immigration, while for the remaining provinces and territories, the prevalence appeared similar among all those aged 15 years or older at immigration (Table 4). The estimated prevalence of tuberculosis infection was lowest in Quebec (19%, 95% UI 16%–24%) and highest in Alberta and BC at 24% (95% UI 21%–28%) and 24% (95% UI 20%–30%), respectively.
Estimated prevalence of tuberculosis infection by age at immigration and province or territory of residence in 2021
The estimated prevalence of tuberculosis infection increased with age during census year 2021 from 2% (95% UI 1%–2%) among those younger than 15 years in 2021 to 36% (95% UI 29%–50%) among those aged 75 years or older in 2021. Overall prevalence did not change substantially by time since immigration. However, when stratified by age during the census year, the estimated prevalence decreased by time since immigration, reflecting lower values among those who entered Canada at a younger age (Appendix 1, Table S7).
As expected, the estimated prevalence of tuberculosis infection acquired in the preceding 2 years increased with the incidence of tuberculosis disease in the country of origin (Table 5). Overall, only an estimated 0.05% (95% UI 0.04%–0.08%) of foreign-born residents in Canada in 2021 had acquired tuberculosis infection in the preceding 2 years. This increased to 0.8% (95% UI 0.6%–1.0%) when considering only those who immigrated in 2020 and 2021. These data suggest that, among all residents born outside of Canada with tuberculosis infection, an estimated 1 in 488 (95% UI 185–1039) had been infected within the preceding 2 years. For those with tuberculosis infection who had arrived in 2020 or 2021, an estimated 1 in 54 (95% UI 20–312) had been infected within the preceding 2 years. To detect 1 person infected within the last 2 years among all foreign-born residents, 2410 (95% UI 775–7505) would need to be tested. To detect 1 person infected within the preceding 2 years by testing only those who had arrived in 2020 or 2021, 231 (95% UI 59–2787) would need to be tested.
Estimated prevalence of recently acquired tuberculosis infection among foreign-born residents in 2021
Interpretation
Our estimates suggest that almost one-quarter of Canadian permanent residents and citizens born outside the country have tuberculosis infection, a proportion that did not substantially change between 2001 and 2021. However, despite the large number of people with tuberculosis infection, very few were likely infected within the preceding 2 years, the highest risk period for progression to tuberculosis disease.25
Our prevalence estimates for tuberculosis infection are concordant with those from other low-incidence settings, notably an analysis that used similar methods to estimate prevalence among migrants living in Australia.26 They are also concordant with cross-sectional surveys. Using tuberculin skin tests, the US National Health and Nutrition Examination Survey (NHANES) estimated the prevalence of tuberculosis infection to be 18.1% and 20.5% among foreign-born people in 1999–2000 and 2011–2012, respectively.27–29 Other surveys in the UK and the Netherlands using interferon-γ release assays estimated a prevalence of about 20% among foreign-born people between 2008 and 2012.30,31
By census year 2021, most permanent residents and citizens born outside Canada originated from countries with an incidence of tuberculosis disease of 50 per 100 000 people or higher, with a substantial increase in those from countries with incidence of 200 per 100 000 people or higher. This was balanced by a decrease in estimated prevalence of tuberculosis infection among those from some of the countries with the highest incidence of tuberculosis, including China, India and Vietnam. This decline may potentially reflect the impact of improvements in both socioeconomic conditions and tuberculosis care programs in those countries.20,32
These results can help inform clinical and programmatic decision-making around screening and treatment for tuberculosis infection. They provide a provincial-level picture of the prevalence of tuberculosis infection, which is relevant as health care policies fall within the provincial purview. They also have implications for tuberculosis infection screening and treatment programs. Our results reinforce earlier suggestions that screening for tuberculosis and providing preventive treatment to people who immigrated before adulthood will have limited public health impact as the prevalence of tuberculosis infection among this group is low.12,33 Although prevalence is higher among older residents, the risk of adverse events with preventive treatment for tuberculosis — even newer, rifamycin-based regimens — increases with age,34,35 and the likelihood that tuberculosis infection was acquired within the previous 2 years is low. Even if tuberculosis infection testing targets foreign-born residents from high-burden countries shortly after arrival, few residents found to have tuberculosis infection will have been infected within the previous 2 years.
As the yield and cost-effectiveness of any screening and treatment program for tuberculosis infection increase with both pretest probability of tuberculosis infection and risk of progression to tuberculosis disease among those with tuberculosis infection, 10–12,30,33 our results are directly relevant to future tuberculosis prevention programs. They suggest that, although tuberculosis infection is common among foreign-born Canadian residents, it has usually been acquired many years previously. For that reason, groups most likely to benefit from screening for tuberculosis infection are new entrants and very recent arrivals (within 1–2 yr) — particularly adults who have arrived from countries with high incidence of tuberculosis. In the absence of major risk factors for progression to tuberculosis disease (e.g., HIV coinfection, end-stage renal disease, recent contact with a person with contagious tuberculosis disease), most foreign-born residents already established in Canada should not be screened.
With currently available tests, without preventive treatment, a maximum of 5%–10% of people who test positive for tuberculosis infection will ever develop tuberculosis disease. Hence the number needed to screen to prevent tuberculosis disease in 1 person likely exceeds 1000, even if screening focuses on people from high-incidence countries who have recently immigrated. Given the low case fatality rate in Canada, the number needed to screen to prevent 1 death from tuberculosis disease in this group is at least an order of magnitude higher. To contextualize these numbers, although within a completely different disease setting, Canadian guidelines estimate that for females aged 50–59 years, the number needed to screen with mammography every 2–3 years to prevent 1 death from breast cancer is 1333 (95% confidence interval 909–2857).36
Strengths of this analysis include the use of robust, previously reported methodology for estimating risks of acquiring tuberculosis infection over time in many countries. We also accounted explicitly for uncertainty around our country-and time-based estimates of infection risk.
Limitations
The source data assumed that people with positive results on the tuberculin skin test truly had tuberculosis infection and remained infected with viable mycobacteria for life, with no allowance for self-clearance. Thus, we may have overestimated the prevalence of tuberculosis infection, particularly in older age groups.37–39 However, this is a potential shortcoming of any analysis based on current immunologic tests for tuberculosis infection. Indeed, failure to account for self-clearance has been argued to lead to an underestimate of the number of people who have recently acquired tuberculosis infection and their ensuing risk for tuberculosis disease and subsequent transmission.40
We assumed that the annual risk of infection was consistent among people within a given country in any given year, which obscures variation related to geography, mixing patterns and other social factors.41,42 Although the rate of immigration to Canada is expected to increase substantially,43 prevalence patterns for tuberculosis infection may change according to numbers within specific immigration categories (e.g., economic class, family reunification, refugee), which we were unable to account for with Canadian Census data. For example, refugees are more likely to have tuberculosis infection and to progress to tuberculosis disease than others from the same countries.38 The quality of data on the annual risk of infection also varied substantially by country and year, with annual risk of infection estimates most frequently based on incidence of tuberculosis disease as estimated by the WHO.
Similarly, we lacked estimates of annual risk of infection stratified by immigration category or sex, meaning we were unable to stratify our tuberculosis infection prevalence estimates accordingly. 42 Our analysis was limited to permanent residents and citizens born outside Canada; we could not provide estimates for temporary residents, nor could we account for time spent in Canada before acquiring permanent residency. Our annual risk of infection estimates do not account for migrants’ return visits to their countries of origin or for residence in multiple countries before immigration to Canada. Finally, in categorizing countries by tuberculosis incidence, we relied on recent WHO estimates rather than those corresponding to the exact dates when foreignborn residents moved to Canada as robust data were not consistently available before 2000; therefore, some older foreign-born residents from countries with decreasing tuberculosis incidence may have faced higher past infection risks than current incidence estimates implied. We did account for changing annual infection probabilities in our cumulative risk estimates.
Conclusion
About one-quarter of foreign-born residents likely have tuberculosis infection, but few were recently infected. The composition of foreign-born residents has changed over time, with more immigration from countries with high incidence of tuberculosis disease, althought the estimated prevalence has dropped somewhat among immigrants from several key countries. These data can help inform future strategies to reduce the burden of tuberculosis disease among foreign-born residents in Canada.
Footnotes
Competing interests: James Johnston reports support from the Michael Smith Foundation for Health Research BC. Faiz Ahmad Khan reports support from the Canadian Institutes of Health Research, the National Research Council of Canada, Fonds de Recherche du Québec – Santé, Fonds de Recherche du Québec – Nature et technologies, Fonds de recherche du Québec – Société et culture, and Institut nordique du Québec. Delft and qure.ai have provided Faiz Ahmad Khan’s laboratory with use of their software for chest radiography analysis at academic-use pricing. Contractual agreements are in place to ensure the companies do not have input in any aspect of research design, conduct or reporting. Kevin Schwartzman reports support from the Bill and Melinda Gates Foundation and participation on a data safety monitoring board for Laurent Pharmaceuticals. He is a volunteer board member and executive committee member with the International Union Against Tuberculosis and Lung Disease. No other competing interests were declared.
This article has been peer reviewed.
Contributors: Aria Ed Jordan, Jonathon Campbell and Kevin Schwartzman designed this study. Aria Ed Jordan, Ntwali Placide Nsengiyumva, Rein Houben, Peter Dodd, Katie Dale, James Trauer and Justin Denholm contributed to data acquisition. Aria Ed Jordan and obtained and analyzed the relevant data from Statistics Canada. Aria Jordan, Ntwali Placide Nsengiyumva and Jonathon Campbell contributed to data analysis. All authors interpreted the data. Aria Jordan, Jonathon Campbell and Kevin Schwartzman drafted the manuscript. All authors revised it critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work. Jonathon Campbell and Kevin Schwartzman share senior authorship.
Funding: This study was supported by the Canadian Institutes of Health Research (no. PJT-173348). Aria Ed Jordan was supported by an Internal Studentship Award of the Faculty of Medicine and Health Sciences, McGill University. The funders had no role in the design, conduction, data collection, analysis, management, interpretation, or in manuscript preparation or in the decision to submit for publication.
Data sharing: All relevant data are in the main text or appendix. Code is available on Github (https://github.com/Acesa2t).
- Accepted October 12, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/