Abstract
Background: First Nations, Inuit and Métis Peoples across geographies are at higher risk of SARS-CoV-2 infection and COVID-19 because of high rates of chronic disease, inadequate housing and barriers to accessing health services. Most Indigenous Peoples in Canada live in cities, where SARS-CoV-2 infection is concentrated. To address gaps in SARS-CoV-2 information for these urban populations, we partnered with Indigenous agencies and sought to generate rates of SARS-CoV-2 testing and vaccination, and incidence of infection for First Nations, Inuit and Métis living in 2 Ontario cities.
Methods: We drew on existing cohorts of First Nations, Inuit and Métis adults in Toronto (n = 723) and London (n = 364), Ontario, who were recruited using respondent-driven sampling. We linked to ICES SARS-CoV-2 databases and prospectively monitored rates of SARS-CoV-2 testing, diagnosis and vaccination for First Nations, Inuit and Métis, and comparator city and Ontario populations.
Results: We found that SARS-CoV-2 testing rates among First Nations, Inuit and Métis were higher in Toronto (54.7%, 95% confidence interval [CI] 48.1% to 61.3%) and similar in London (44.5%, 95% CI 36.0% to 53.1%) compared with local and provincial rates. We determined that cumulative incidence of SARS-CoV-2 infection was not significantly different among First Nations, Inuit and Métis in Toronto (7364/100 000, 95% CI 2882 to 11 847) or London (7707/100 000, 95% CI 2215 to 13 200) compared with city rates. We found that rates of vaccination among First Nations, Inuit and Métis in Toronto (58.2%, 95% CI 51.4% to 64.9%) and London (61.5%, 95% CI 52.9% to 70.0%) were lower than the rates for the 2 cities and Ontario.
Interpretation: Although Ontario government policies prioritized Indigenous populations for SARS-CoV-2 vaccination, vaccine uptake was lower than in the general population for First Nations, Inuit and Métis Peoples in Toronto and London. Ongoing access to culturally safe testing and vaccinations is urgently required to avoid disproportionate hospital admisson and mortality related to COVID-19 in these communities.
Multigenerational colonial policies that aimed to assimilate First Nations, Inuit and Métis Peoples and appropriate land and resources have led to inequities across most major health outcomes for First Nations, Inuit and Métis living in urban, rural and remote geographies compared with non-Indigenous people in Canada, as well as striking gaps in access to equitable and culturally safe health care.1,2
More than half of Indigenous Peoples in Canada live in urban areas.3 In cities, jurisdictional complexities, including structured exclusion from potentially beneficial government programs, combined with persistent and growing inequities in the distribution of urban health and social resources, have exacerbated pre-existing Indigenous compared to non-Indigenous health inequities during the COVID-19 pandemic.4 Dense and multigenerational social networks; barriers in access to culturally safe health care; and a disproportionate burden of poverty, chronic disease and inadequate housing5–7 create conditions for the spread of SARS-CoV-2 among First Nations, Inuit and Métis living in urban areas in Canada.
The quality, comprehensiveness and accessibility of First Nations, Inuit and Métis health and social statistics in Canada, particularly for those living in urban and related homelands, is a critical problem.4,8 A lack of accurate, inclusive and culturally safe identification processes for First Nations, Inuit and Métis in health service and public health data systems,8 and inadequate engagement of Indigenous leadership in the governance and management of their health information, which is essential,8,9 contribute to this problem. As a result, Indigenous health policy and service responses are commonly implemented without accurate and reliable population-based sociodemographic and health outcomes data.
Although First Nations health authorities mobilized quickly to document SARS-CoV-2 incidence and COVID-19 morbidity and mortality in First Nations communities in the early pandemic period, and vaccination campaigns led by First Nations were successful,10,11 published reports of SARS-CoV-2 outcomes for First Nations, Inuit and Métis living in urban and related homelands remain unavailable more than 2 years into the COVID-19 pandemic.
Since 2008, our research team has partnered with urban Indigenous health service providers to address gaps in health and social information for First Nations, Inuit and Métis living in urban and related homelands to produce representative, population-based, community-controlled health information for urban First Nations, Inuit and Métis,5,6,12 by successfully applying respondentdriven sampling (RDS) methods to generate valid, population-representative cohorts of First Nations, Inuit and Métis adults.13 Drawing on 2 of these cohorts (Our Health Counts Toronto and Our Health Counts London), which had existing linkages to health care databases at ICES, we sought to generate accurate and valid rates of SARS-CoV-2 testing and vaccination, and incidence of infection for First Nations, Inuit and Métis living in Toronto and London, Ontario, and to compare these rates with those in the general populations in each city and Ontario.
Methods
Study setting
We drew on 2 existing cohorts of urban First Nations, Inuit and Métis adults, recruited using RDS, to conduct a linked cohort study during the COVID-19 pandemic. Ontario has the largest populations of First Nations, Inuit and Métis in Canada.3 According to the Canadian Census, more than 70% of this population lives in urban centres.14 Our previous studies have found that the actual number of First Nations, Inuit and Métis living in Ontario cities is higher than reported by the Census.5,6,12,15–17 Using Our Health Counts studies, we estimated the current size of the First Nations, Inuit and Métis population in Toronto to be 88 00015 and in London to be 41 000,16 representing 3.2% and 9.6% of the total population in each city, respectively. First Nations consitute most of the Indigenous Peoples in these 2 cities.13,16 More Inuit and Métis live in Toronto than in London.16,18
Indigenous partnerships
The Our Health Counts Indigenous partnership approach to research advances precepts of Indigenous community-based participatory action research to quantitative population health, centring First Nations, Inuit and Métis epistemologies, concepts and priorities to assure and optimize local community benefit. It formalizes local Indigenous governance throughout the research process through ongoing co-leadership and research, and data-sharing and publication agreements. The academic research team is based at the Well Living House and York University. In Toronto, the academic team partnered with Seventh Generation Midwives Toronto, an Indigenous-focused midwifery practice in Toronto. In London, we partnered with the Southwest Ontario Aboriginal Health Access Centre, which works to improve access to and quality of health and social services for First Nations, Inuit and Métis in southwestern Ontario. Seventh Generation Midwives Toronto and Southwest Ontario Aboriginal Health Access Centre co-lead all Our Health Counts studies in Toronto and London, respectively, and are the legally recognized data custodians.
Baseline cohorts
Our Health Counts methods and results, including cohort recruitment and population characteristics, are reported elsewhere. 5,6,12,15–21 Briefly, baseline Our Health Counts cohorts of 915 First Nations, Inuit and Métis adults in Toronto and 508 adults in London were recruited using RDS in 2015–2016.12,21
Respondent-driven sampling leverages the strength of community social networks to allow for recruitment of a representative sample of a population or community of interest.13 The strong Indigenous social networks and cultural identity in both Toronto and London contributed to the decision to use RDS to ensure successful participant recruitment and study success.19,20
Adults (aged ≥ 15 yr) who self-identified as First Nations, Inuit and Métis and lived, worked in or received health or social services in each city were eligible for recruitment. Our Health Counts Toronto began with 10 initial participants (seeds), each of whom was asked to recruit up to 3 members of their community. To increase enrolment speed, 10 additional seeds were added and the number of coupons increased to 5. Participants received $20 for completing the survey and an additional $10 for each participant they recruited. Similarly, Our Health Counts London began with 6 initial seeds and the same financial incentives for study participation and subsequent peer recruitment. Highly networked people from diverse First Nations, Inuit and Métis social sectors (e.g., young families, Elders and students) were recruited as initial seeds in both cities. After recruitment, participants completed a respectful health assessment survey22,23 with a trained Indigenous interviewer, and consent was sought for subsequent ICES data linkages.5,12,21 To determine personal network sizes, each participant was asked, “Approximately how many Aboriginal people do you know (i.e., by name that know you by name) who currently live, work or use health services in (Toronto or London, respectively).” Recruitment network diagrams are presented in Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.212147/tab-related-content.
Restricted and comparator cohorts
In 2020, we expanded our data linkages to include COVID-19 information. Using Ontario Health Insurance Plan (OHIP) identifiers and updated geographical information (Appendix 2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.212147/tab-related-content), we restricted the cohorts to First Nations, Inuit and Métis who were alive and living in Toronto and London at the beginning of the COVID-19 pandemic. We considered people who did not meet these criteria to be the excluded cohort. We also generated comparator cohorts to represent the total populations of adults 15 years of age or older in Toronto, London and Ontario using ICES databases of people who have ever held an OHIP number. Inclusion in these comparator cohorts required that people were living; had contact with the health care system within the past 9 years (age < 65 yr) or 3 years (age ≥ 65 yr); and were residents of London, Toronto and of the province of Ontario (Appendix 3, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.212147/tab-related-content). Evaluation of rates, convergence and bottleneck plots for the baseline and restricted cohorts in Toronto and London showed that our estimates of key demographic characteristics, including age, gender, Indigenous identity (i.e., First Nations, Inuit or Métis) and education status were stable, which suggests that both the baseline and restricted cohorts were representative of the target population (Appendix 4, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.212147/tab-related-content).24
Outcomes
Our primary outcomes were prevalence of ever having a SARS-CoV-2 test, rate of ever having a positive result for a SARS-CoV-2 test, and SARS-CoV-2 vaccination rate. Secondary outcomes included rates of hospital admission and mortality.
Data linkage
Informed consent of study participants for prospective data linkage to ICES databases was obtained at the time of recruitment. More than 97% of Our Health Counts Toronto and 96% of Our Health Counts London participants agreed to longitudinal ICES data linkages at the time of recruitment. We used direct and probabilistic methods that drew on unique encoded identifiers for successful linkages of 97.3% and 99.6% of baseline Our Health Counts Toronto and Our Health Counts London cohorts, respectively, to ICES databases. We accessed ICES’s COVID-19 Integrated Testing Data set (C19INTGR) for SARS-CoV-2 testing and incidence of infection measures. This data set is a comprehensive set of all available COVID-19 diagnostic laboratory results in Ontario, derived from 3 data sources: the Ontario Laboratories Information System; distributed testing data from laboratories within the COVID-19 Provincial Diagnostic Network; and the Public Health Ontario Case and Contact Management System (previously called the integrated Public Health Information System). For SARS-CoV-2 vaccination rates, we accessed ICES’s COVaxON database. This database is Ontario’s central point-of-care SARS-CoV-2 vaccine management system and database. We obtained data on secondary outcomes through ICES linkage to the Case and Contact Management System.
Statistical analysis
Between Mar. 31, 2020, and Dec. 6, 2021, we produced weekly crude and RDS-adjusted estimates and unadjusted general population comparator rates for the cities of Toronto and London and the province of Ontario for our primary and secondary outcomes.25 This early December 2021 end point reduced exposure to external confounders linked to the emergence of the Omicron variant, including changes in access to polymerase chain reaction testing. To address any potential age confounding arising from the relatively youthful First Nations, Inuit and Métis population demographics, we subsequently age-adjusted general population comparator rates for Toronto, London and Ontario using direct methods26 and Our Health Counts–estimated age distributions for the First Nations, Inuit and Métis populations of Toronto and London as the reference populations.27 We determined that male and female gender distributions were similar for First Nations, Inuit and Métis and comparison populations, which precluded the need for adjustment (Table 1 and Appendix 5, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.212147/tab-related-content).
Characteristics of the population-based cohorts of Our Health Counts Toronto and Our Health Counts London
To ensure convergence of our RDS estimators, we used RDS-II29 weights to obtain RDS-adjusted estimates of sociodemographic, health and cultural continuity characteristics, and SARS-CoV-2 testing, diagnosis and vaccination rates among First Nations, Inuit and Métis living in London and Toronto. We also performed a preliminary evaluation of clinically relevant and statistically significant differences between the restricted and excluded cohorts using the RDS MOVER method.28 We excluded the seeds from all analyses. We conducted the analyses in the R environment at the 5%, 2-sided significance level,30,31 without adjustment for multiple testing. A complete STROBE (Strengthening the Reporting of Observational Studies in Epidemiology)-RDS checklist32 is included in Appendix 6, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.212147/tab-related-content. For data on hospital admission and mortality, we included only crude counts because of the small sample size.
Ethics approval
Seventh Generation Midwives Toronto and Southwest Ontario Aboriginal Health Access Centre requested the study, vetted the design, approved data access and co-led the interpretation of results and publications. The original Our Health Counts Toronto and London studies were approved by the Unity Health Toronto Research Ethics Board (Certificate nos. 14–083 and 14–390). The COVID-19 analyses were also approved by York University’s Research Ethics Board (the Human Participants Review Committee; Certificate no. e2020–254).
Results
We included 723 and 364 First Nations, Inuit and Métis participants living in Toronto and London, respectively, as of Dec. 31, 2019, in the restricted Our Health Counts cohorts. Table 1 provides select sociodemographic, health and cultural continuity indicators for the restricted and excluded populations of Our Health Counts Toronto and London. There is a striking and crosscutting pattern of sociodemographic challenges, disproportion burden of disease, gaps and barriers in access to health care, and strong cultural continuity. Expanded reporting is available elsewhere. 19,20 Our comparison of restricted and excluded cohort estimates showed minor potential differences in a small number of specific age and educational categories. For example, compared with the included cohort, the excluded cohort showed higher levels of postsecondary education among First Nations, Inuit and Métis both in Toronto and London. On balance, however, the restricted cohort appears representative of the local First Nations, Inuit and Métis communities.
As of Dec. 6, 2021, we found higher RDS-adjusted estimates of SARS-CoV-2 testing and a comparable cumulative rate of SARS-CoV-2 infection among First Nations, Inuit and Métis living in Toronto than for crude and age-adjusted rates for the overall Toronto and Ontario populations. For First Nations, Inuit and Métis living in London, the rate of SARS-CoV-2 testing was similar to crude and age-adjusted local comparison rates. We also found that the point estimate for the rate of SARS-CoV-2 infection among First Nations, Inuit and Métis in London was more than twice that of the overall city population, but this difference was not statistically significant (Table 2). Rates of vaccine uptake among First Nations, Inuit and Métis in both Toronto and London were considerably lower than crude and age-adjusted rates among the general populations of the cities and Ontario. This lower rate of vaccine uptake was consistent for both first and second doses. In Toronto, the estimated rate of second dose SARS-CoV-2 vaccination among First Nations, Inuit and Métis was 21.5% lower than the age-adjusted rate among the general population; in London, the rate among First Nations, Inuit and Métis was 19.5% lower than the age-adjusted rate in the general population of the city. Uptake of SARS-CoV-2 vaccine eventually plateaued for all groups (Figure 1).
Respondent-driven sampling–adjusted prevalence of COVID-19 testing, cumulative incidence of SARS-CoV-2 infection, and prevalence of first and second dose vaccine uptake among First Nations, Inuit and Métis in Toronto and London, overall city and province as of Dec. 6, 2021
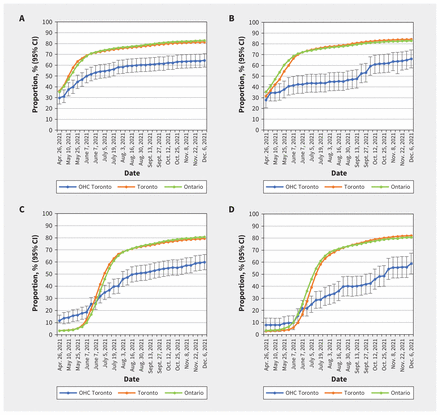
Proportion of First Nations, Inuit and Métis adults (from Our Health Counts [OHC] cohorts) A) in Toronto with a first dose of SARS-CoV-2 vaccine compared with the general populations of Toronto and Ontario, B) in London with a first dose of SARS-CoV-2 vaccine compared with the general populations of London and Ontario, C) in Toronto with a second dose of SARS-CoV-2 vaccine compared with the general populations of Toronto and Ontario and D) in London with a second dose of SARS-CoV-2 vaccine compared with the general populations of London and Ontario. Note: CI = confidence interval.
Small cells and risk of reidentification precluded disclosure and RDS analysis of data for hospital admission for London and mortality data for both cities among First Nations, Inuit and Métis. The unadjusted rate of hospital admission among First Nations, Inuit and Métis in Toronto was 27.1%, compared with 7.7% and 5.9% in the general populations of Toronto and Ontario, respectively, which suggests that First Nations, Inuit and Métis in Toronto were at a higher risk of hospital admission linked to COVID-19 than the general city and Ontario populations.
Interpretation
We found that, although First Nations, Inuit and Métis living in London had an observed incidence rate of SARS-CoV-2 infection more than twice that of the local population, the cumulative rates for First Nations, Inuit and Métis in both cities were not significantly different from overall city and provincial rates. We also found striking and consistent disparities in SARS-CoV-2 vaccine uptake among First Nations, Inuit and Métis living in Toronto and London compared with overall city and provincial populations. As of Dec. 6, 2021, the rate of complete vaccination in Toronto among First Nations, Inuit and Métis was 58.2% (95% CI 51.4% to 64.9%), compared with 79.4% for the overall population of Toronto. The rate of 2-dose vaccination for First Nations, Inuit and Métis in London was 61.5% (95% CI 52.9% to 70.0%), compared with 82.1% for the overall London population. Adjusting for age had little impact on these results. Cumulative SARS-CoV-2 testing rates among First Nations, Inuit and Métis were 10.2% higher in Toronto and comparable in London relative to local age-adjusted city and provincial rates. Our secondary analyses found crude rates of hospital admission for COVID-19 among First Nations, Inuit and Métis in Toronto that were 3.5 times higher than those of the general population of Toronto.
Our observation of lagging rates of 2-dose vaccination among First Nations, Inuit and Métis in Toronto and London compared with First Nations living on and off reserve in Ontario33 and national rates for First Nations living on reserve10,34 are aligned with evidence from Manitoba that showed lower rates of vaccine uptake for First Nations living off reserve compared with on reserve.11 Possible explanations include provincial policies that delayed access to and resources for vaccination among First Nations, Inuit and Métis living in cities compared with First Nations living on reserve, and Indigenous mistrust of vaccines and the urban hospitals that led Ontario’s vaccine distribution.35 According to Dr. James Makokis (a Cree physician), “What’s really important to differentiate [is that] Indigenous people who are mistrusting of the health system because of systemic racism, oppression and genocide are a very different population than those that are protesting outside of hospitals for their perceived infringement on their individual human rights.”36
Our finding of modestly higher rates of SARS-CoV-2 testing among First Nations, Inuit and Métis living in Toronto compared with overall city and provincial rates provides evidence that First Nations, Inuit and Métis living in cities can be engaged in the COVID-19 response. To address systemic barriers in access to hospital-based SARS-CoV-2 testing for First Nations, Inuit and Métis, local Indigenous health providers across Ontario (including Seventh Generation Midwives Toronto and Southwest Ontario Aboriginal Health Access Centre) quickly mobilized to start Indigenous-specific SARS-CoV-2 testing programs. In Toronto, this included Anishnawbe Health Toronto’s mobile testing clinic37 and the Auduzhe Mino Nesewinong comprehensive COVID-19 response clinic and outreach program.38 Our findings on SARS-CoV-2 testing suggest that these “by community, for community” programs were successful in mitigating barriers to accessing SARS-CoV-2 testing.
Based on the higher incidence rates of SARS-CoV-2 among First Nations living on reserve in Canada39 and Native Americans and Alaska Natives in the United States,40 and the elevated rates of inadequate, multigenerational housing and chronic diseases among First Nations, Inuit and Métis living in Toronto and London, 7,41–43 we hypothesized that we would find a higher incidence of COVID-19 among First Nations, Inuit and Métis in Toronto and London than in the overall city populations. We found that point estimates for COVID-19 incidence among First Nations, Inuit and Métis were higher than those of the overall population in both cities, but these differences were not statistically significant. First Nations, Inuit and Métis community members may be motivated to limit the spread of COVID-19 to family and community by participating in public health responses including testing, case management and contact tracing because of heightened awareness of community harms arising from multigenerational, disproportionate morbidity and mortality from infectious diseases. Our preliminary findings of higher rates of hospital admission among First Nations, Inuit and Métis with COVID-19 in Toronto compared with the general population could be attributed to a high burden of comorbid chronic disease among First Nations, Inuit and Métis in Toronto,38 which could result in more severe COVID-19.
Our finding of markedly lower rates of vaccine uptake among First Nations, Inuit and Métis is of concern within the context of the global emergence of highly transmissible new variants and evidence of higher morbidity and mortality among First Nations, Inuit and Métis. There is a time-sensitive need to amplify Indigenous-focused COVID-19 response measures to prevent widespread SARS-CoV-2 infection among those who are not vaccinated with a subsequent surge in hospital admissions and mortality caused by COVID-19 among First Nations, Inuit and Métis. Localized by-community-for-community approaches have successfully engaged First Nations, Inuit and Métis living in cities in the COVID-19 response and could be used to further improve access to trusted COVID-19 information sources and culturally safe vaccination opportunities.42,44 Additional mitigating strategies could include rapid access to Indigenous-led and community-situated SARS-CoV-2 testing, case management, contact tracing and community outreach.37,38 Given the problematic attitudinal and systemic racism experienced by First Nations, Inuit and Métis in urban hospitals, there is also a need to plan and implement culturally safe supports for First Nations, Inuit and Métis who are unvaccinated and may be admitted to hospital in Canadian cities. Finally, there is an ongoing need, highlighted by the COVID-19 pandemic, to address infrastructure gaps in health information that mask health inequities for First Nations, Inuit and Métis living in urban and related homelands.
Limitations
Although we have shown that the study cohorts for Our Health Counts Toronto and London are representative of the overall First Nations, Inuit and Métis population in each city, generalization to other First Nations, Inuit and Métis populations should be approached with caution, given the distinct social, cultural and colonial characteristics of First Nations, Inuit and Métis and settler populations across geographies and jurisdictions. Almost all vaccine clinics, including Indigenous-specific clinics, in both cities and nearby First Nations communities used the COVaxON tracking system; however, it is possible that vaccine events may not have been entered, or entered incorrectly, in this database. Furthermore, RDS design effects limited precision. As a result, we were constrained in our ability to detect significant differences in SARS-CoV-2 outcomes between First Nations, Inuit and Métis, overall city and provincial populations and to produce precise RDS-adjusted estimates of hospital admissions linked to COVID-19 among First Nations, Inuit and Métis. Finally, we could not remove First Nations, Inuit and Métis people from our comparator reference populations because of gaps in existing health system infrastructure, including the absence of inclusive and reliable indicators of First Nations, Inuit and Métis identity in source data sets. Given the large sample size of these populations and relatively small number of First Nations, Inuit and Métis people, particularly in Toronto, this had a minimal effect on our Toronto findings and a small effect on our London findings.
Conclusion
Working in partnership with local Indigenous health service providers, our team was able to bridge critical gaps in SARS-CoV-2 impact and vaccine uptake data among First Nations, Inuit and Métis living in Toronto and London. Although governmental policies prioritize Indigenous populations for SARS-CoV-2 vaccination, vaccine uptake is low among First Nations, Inuit and Métis in these cities. Ongoing access to culturally safe testing, specialized vaccination strategies and community outreach is needed to mitigate disproportionate hospital admissions and mortality linked to COVID-19 among these populations.
Footnotes
Competing interests: Janet Smylie reports grants from the Canadian Institutes of Health Research and Indigenous Services Canada. No other competing interests were declared.
This article has been peer reviewed.
Contributors: Janet Smylie co-led the study design, oversaw the data analyses, co-led the writing of all versions of the manuscript and co-led the response to reviewers. Stephanie McConkey co-led data analyses; led production of tables and figures; and co-led writing of methods and results sections and co-led response to reviewers. Beth Rachlis led ICES data analyses. Lisa Avery supported data analyses and supported the writing of the methods and results section. Graham Mecredy co-led the study design and oversaw ICES processes and data analyses. Raman Brar co-led data analysis and reviewed final draft manuscripts. Cheryllee Bourgeois, Brian Dokis and Stephanie Vandevenne oversaw Indigenous data governance, ensured the study was aligned with Indigenous community research priorities and ensured that the interpretation of findings and overall manuscript were aligned with Indigenous community realities and research requirements. Michael Rotondi co-led the study design, oversaw the data analyses, co-led the writing of the manuscript, and co-led response to reviewers including preparation of the first draft. All of the authors gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This study was supported by ICES through the Applied Health Research Question program, which is funded by the Ontario Ministry of Health and Ministry of Long-Term Care. This study was also supported by the Canadian Institutes of Health Research COVID-19 Rapid Research Operating grant (funding reference no. 172674). Janet Smylie is supported by a Tier 1 Canada Research Chair in Advancing Generative Health Services for Indigenous Populations in Canada.
Data sharing: In keeping with the principles of Indigenous data sovereignty, all project data sets are owned and controlled by the Indigenous community project partners (Seventh Generation Midwives Toronto [Our Health Counts Toronto Dataset] and Southwestern Ontario Aboriginal Health Access Centre [Our Health Counts London Dataset]). Requests for data access should be conveyed to the corresponding author who will support liaison with the Indigenous community project partners, including access to relevant data request forms and processes.
Disclaimer: This study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health (MOH) and Ministry of Long-Term Care (MLTC). The opinions, results and conclusions reported in this paper are those of the authors and are independent from the funding sources. No endorsement by ICES, the MOH or the MLTC is intended or should be inferred.
- Accepted July 4, 2022.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/