Major depressive disorder is among the most prevalent psychiatric disorders and is a leading cause of morbidity and lost productivity.1 The 1-year prevalence of major depressive disorder in the Canadian population is 3.2%–4.6%.2 A large, multisite prospective trial showed that only 28% of patients experience remission following monotherapy with a serotonin reuptake inhibitor.3 Further, remission rates following antidepressant use decrease with each successive treatment failure, such that after 12 months of follow-up and up to 4 attempts at symptom control with different medications, only 60% of patients experience remission.4,5 The remaining patients can be classified as having treatment-refractory depression.
The failure of monoamine-modulating medications to successfully treat a significant percentage of cases of major depressive disorder challenges the traditional conception of this condition as a monoamine deficiency state.5 Accordingly, and in light of neurocircuitry models of the brain (Appendix 1, available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.121317/-/DC1) and advances in technology allowing various means of modulating activity in key structures of the brain, interest in the therapeutic potential of neuromodulation for difficult-to-treat mood disorders has increased in recent years. In this review, we outline the mechanisms, safety and clinical evidence for neuromodulation in treatment-refractory major depression. The quality of evidence for the different neuromodulation strategies varies substantially, ranging from small, open-label case series to blinded, randomized controlled trials and meta-analyses (Box 1).
Evidence used in this review
We searched PubMed for articles about neuromodulation in major depression. We used the following search terms alone or in combination: “electroconvulsive therapy,” “transcranial magnetic stimulation,” “deep brain stimulation,” “vagal nerve stimulation,” “direct current stimulation,” “major depression” and “treatment resistant depression;” we also searched using the acronyms “DBS,” “ECT” and “TMS.” We did not limit our searches by date. There were no meta-analyses of deep brain stimulation in depression, but we found 21 meta-analyses on electroconvulsive therapy and 17 on transcranial magnetic stimulation. We found no published randomized controlled trials of deep brain stimulation for the treatment of depression. We identified 134 articles on transcranial magnetic stimulation for depression, as well as 230 articles on electroconvulsive therapy. All results were manually searched. We included only those that were relevant and enhanced our discussion and those with clearly defined patient populations and outcome measures.
What are the neuromodulation options for major depression?
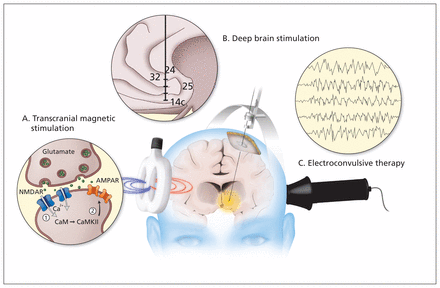
Neuromodulation is either noninvasive or invasive, based on the extent to which the technology interacts directly with the brain (Figure 1). Non-invasive options include electroconvulsive therapy, transcranial magnetic stimulation and trans-cranial direct current stimulation.6 Invasive options include vagal nerve stimulation7 and deep brain stimulation. Here we focus on the 3 modalities for which the most evidence is currently available: electroconvulsive therapy, transcranial magnetic stimulation and deep brain stimulation.
(A) Transcranial magnetic stimulation is thought to produce durable changes in synaptic strength via the NMDA-receptor–dependent mechanisms of long-term potentiation and long-term depression. Simultaneous stimulation of presynaptic and postsynaptic neurons strengthens or weakens the synaptic connection, depending on the frequency and pattern of stimulation. When applied to areas of prefrontal cortex that are hypoactive in depression, repetitive transcranial magnetic stimulation gradually increases their activity, thereby relieving the illness. (B) With deep brain stimulation, electrodes are inserted under stereotactic guidance into regions of the brain believed to drive maladaptive thoughts and behaviours. Constant electricity, provided by an implanted pulse generator, disrupts neural activity both at local sites (i.e., at the target) and at remote, yet connected, structures, comprising a “mood circuit.” (C) Electroconvulsive therapy induces ictal activity, as shown by the electroencephalographic recording.
Electroconvulsive therapy
Electroconvulsive therapy is the oldest neuromodulatory modality still used to treat major depressive disorder. It arguably remains the gold-standard to which other antidepressant treatments are compared, yet it is underused.8 Electroconvulsive therapy involves the administration of an electrical current to the brain via the scalp to induce a seizure while the patient is in a state of general anesthesia. Although its mechanisms are unknown,9 the superiority of real electroconvulsive therapy over sham electroconvulsive therapy (anesthesia, with or without a subconvulsive dose of electrical current) suggests that the induction of the seizure plays a role in the antidepressant effects of this treatment.10,11
Meta-analyses comparing electroconvulsive therapy to antidepressant medication (Table 1) have found that electroconvulsive therapy is superior to medication in reducing depressive symptoms (effect size 0.80, 95% confidence interval [CI] 0.29–1.29)10 and in achieving an antidepressant response, defined as a 50% or greater reduction in patients’ scores on the Hamilton Rating scale for Depression compared with baseline (odds ratio [OR] 3.72, 95% CI 2.60–5.32).11 Traditionally, it has been thought that the melancholic subtype of major depressive disorder was the most responsive to electroconvulsive therapy, although recent studies have suggested that electroconvulsive therapy can produce an antidepressant response across multiple subtypes of major depressive episodes.17–19 Data from the multicentre study by the Consortium for Research in Electroconvulsive Therapy suggest that the median number of electroconvulsive therapy treatments required to produce an antidepressant response is 3, the number for resolution of suicidal thoughts is 4, and the number for remission is 7.14 Given that electroconvulsive therapy is typically administered 2 or 3 times per week during an acute course, achieving a clinically significant response in 1–3 weeks with electroconvulsive therapy compares favourably with the 4–6 weeks typically required with antidepressant medications.
Studies examining the use of electroconvulsive therapy for the treatment of major depressive disorder
Routine use of general anesthesia, muscle relaxants, continuous oxygenation, vital sign monitoring and brief electrical stimuli have minimized the risks associated with electroconvulsive therapy. The mortality rate has been estimated to be less than 1 death per 73 440 treatments.20 The most common adverse effects (myalgia [1 in 5 patients], headache [1 in 3 patients]) are transient, lasting minutes to hours, and can be treated with analgesics.21 Electroconvulsive therapy is associated with immediate posttreatment disorientation and retrograde amnesia. Although these effects are generally short lived, a 6-month longitudinal follow-up study found that retrograde amnesia persisted in about 1 in 8 patients (12.4%).22 The amnestic effects of electroconvulsive therapy are greater for recent events (i.e., within 3 mo of first treatment) than for remote events (i.e., greater than 3 yr).23 Factors associated with greater cognitive impairment following electroconvulsive therapy include pre-existing cognitive impairment, older age and the use of bilateral electroconvulsive therapy.24 There are no absolute contraindications to electroconvulsive therapy, and it can be used safely during pregnancy.25
Repetitive transcranial magnetic stimulation
Repetitive transcranial magnetic stimulation uses powerful (> 2 Tesla), focused magnetic field pulses to noninvasively stimulate cortical neurons by use of an external electromagnetic coil placed against the patient’s scalp. Unlike electroconvulsive therapy, repetitive transcranial magnetic stimulation does not require the administration of anesthesia, and it does not aim to produce a seizure for its therapeutic effects. Trains of repeated stimulation can produce long-lasting changes in neural excitability. The frequency of stimulation determines the effects of transcranial magnetic stimulation. Low-frequency (< 5 Hz) stimulation inhibits neuronal firing, and high-frequency (> 5 Hz) stimulation increases neuronal firing rates.26
Transcranial magnetic stimulation typically involves 10–30 treatment sessions of 15–45 minutes duration, administered once daily, 5 days a week on an outpatient basis. High-frequency stimulation to the dorsolateral prefrontal cortex is the typical protocol for patients with major depressive disorder, based on neuroimaging evidence that this location in the brain is underactive in people with major depression.27
Transcranial magnetic stimulation has been shown to be consistently more effective than sham treatment for major depressive disorder across several meta-analyses and large randomized controlled trials (Table 2). In a large meta-analysis involving 24 studies and 1092 patients, active transcranial magnetic stimulation, compared with sham stimulation, was associated with higher pooled rates for response (25% v. 9%) and remission (17% v. 6%); this translates to a number needed to treat of 7 for remission and 6 for antidepressant response.28 Recent open-label and randomized controlled studies using newer techniques, such as stronger dosing34 and longer treatment courses,35 have consistently achieved remission rates of 30%–35% and response rates of 40%–55%.33
Transcranial magnetic stimulation studies
Randomized controlled trials have found that electroconvulsive therapy is superior to transcranial magnetic stimulation in achieving remission (59.1% v. 16.7%)36 and reducing suicidal thoughts (mean decrease 2.0 v. 0.5 points on the suicide item of the Hamilton Rating scale for Depression)37 in short-term studies. Safety, tolerability and noninvasiveness are the major advantages of transcranial magnetic stimulation over electroconvulsive therapy. Transcranial magnetic stimulation does not require general anesthesia or neuromuscular blockade, and patients remain awake throughout treatment. Most studies have found no immediate or prolonged negative effects of transcranial magnetic stimulation on cognition.38 A study involving 30 patients with major depressive disorder found that, one week after finishing the course of treatment, cognitive performance remained constant or improved (v. pretreatment) among patients who received transcranial magnetic stimulation to the left dorsolateral prefrontal cortex, while deficits in anterograde memory were observed among patients who underwent right unilateral electroconvulsive therapy.39
Transcranial magnetic stimulation may produce transient headache or local pain in 30%–40% of patients.40 These effects diminish within a few days after treatment and typically respond to over-the-counter analgesics. More serious adverse effects include the emergence of hypomania or suicidal behaviour in less than 1% of patients.41 Very rarely (< 0.1% of patients), high-frequency stimulation may induce seizure. There are no known maternal or fetal risks associated with transcranial magnetic stimulation in pregnancy.
Deep brain stimulation
Deep brain stimulation is the treatment of pathological brain states by the chronic, reversible use of direct electrical current, applied focally to neural elements; this treatment aims to alter their function in isolation or within larger networks.42 Deep brain stimulation is a well-established therapy for Parkinson disease, essential tremor and dystonia. The efficacy and safety of deep brain stimulation in treating movement disorders — combined with its advantages over traditional ablative neurosurgical procedures (e.g., reversibility, ability to modify stimulation parameters) — have spurred its recent application to psychiatric disorders, including major depressive disorder.43 Deep brain stimulation is performed through neurosurgically implanted intracranial electrodes connected to a programmable pulse generator in the patient’s chest wall; this therapy is the most invasive of all currently available neuromodulation approaches.43 Once implanted, stimulation is always on and typically continues indefinitely, with periodic adjustment of stimulation parameters to maintain therapeutic benefit.
The precise mechanisms by which deep brain stimulation exerts its effects are still debated. The early theory that deep brain stimulation simply creates a reversible inhibitory lesion has been supplanted by data suggesting that it produces both immediate and long-term, target-specific effects on neuronal firing rates and patterns.44 In major depressive disorder, deep brain stimulation has been used to target nodes within dysregulated mood circuits that perpetuate the depressed state. The most commonly targeted area has been the subgenual cingulate cortex, although the ventral caudate/striatum, nucleus accumbens and inferior thalamic peduncle have also been investigated45–48 (Appendix 2, available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.121317/-/DC1).
Two prospective, open-label trials of deep brain stimulation of the subgenual cingulate cortex49,50 have shown its efficacy and safety. A Canadian trial performed at 3 centres reported a 6-month response rate of 48%, but a somewhat more disappointing 12-month response rate of 29%.49 Another open-label trial that included patients with major depressive disorder or bipolar disorder found a 58% remission rate and a 92% response rate at 2 years.50 This trial included a 4-week single-blind sham lead-in phase to control for placebo response; the authors report that there was a modest stimulation effect of the sham therapy. In both studies, deep brain stimulation was well-tolerated, with no manic or hypomanic episodes, and no suicides were reported. As an invasive neurosurgical procedure, deep brain stimulation carries a small risk of serious complications (e.g., intracranial hemorrhage) and other perioperative risks (e.g., wound infection, anesthetic complications). Larger multicentre trials with longer sham-stimulation periods and true double-blinding are pending.
Which patients should be referred for neuromodulation?
Box 2 presents a fictional case in which the results of this review are applied in clinical practice. Recent Canadian guidelines about the use of neuromodulation for major depressive disorder have been published (Table 3).51 There are currently no Canadian studies examining the cost-effectiveness of neuromodulation strategies for major depressive disorder. Such studies are complex to perform, and they must balance equipment and personnel costs with lost wages and the public health impact of a serious and highly prevalent mental illness.
Applying the results of this review in clinical practice (fictional case)
YL is a 60-year-old retired pharmacist and a divorced mother of 3. She originally received a diagnosis of major depressive disorder when she was 42 years of age. She has received outpatient care for the past 6 years, following a brief stay in hospital for suicidal ideation around the time of separation from her husband. Her condition was initially controlled by a combination of sertraline and bupropion; however, she no longer appears to be responding to previously effective therapies. She underwent cognitive behavioural therapy, but this provided only a modest improvement in her symptoms. Repeated trials of more aggressive pharmacologic regimens (including nortriptyline plus lithium) and subsequently a monoamine-oxidase inhibitor (tranylcypromine) were also unsuccessful. She has now lost weight, is growing increasingly despondent and depressed, and her condition is seemingly resistant to pharmacologic treatment.
YL was referred for repetitive transcranial magnetic stimulation and completed a course of 20 sessions of dorsolateral prefrontal cortex stimulation over 4 weeks. Although the procedure was well tolerated and her condition showed some improvement, she did not meet the response (> 50% reduction in Hamilton Rating Score for Depression) or remission criteria (Hamilton Rating Score for Depression < 8), 2 months later, she was admitted to hospital after an attempted suicide by medication overdose. She underwent 12 electroconvulsive therapy sessions on an inpatient basis over 6 weeks without appreciable benefit. Reassessment of her diagnosis did not identify major personality pathology, comorbid substance misuse or modifiable life stressors. She was referred to a multidisciplinary team, including a psychiatrist and functional neurosurgeon, for consideration of deep brain stimulation. After discussion of risks and benefits, she elected to proceed with the surgery. Three months later, she underwent successful bilateral implantation of deep brain stimulation electrodes in the subcallosal cingulate, with no adverse effects. By 2 months after implantation, her symptoms were reduced by more than half, and by 6 months she had achieved criteria for remission. Pharmacotherapy was maintained with nortriptyline and lorazepam. Although her condition was in remission, she was able to successfully complete a course of cognitive behavioral therapy; she reported this to be helpful regarding negative thoughts. Two years after implantation, she continues to meet remission criteria and is doing well.
Canadian Network for Mood and Anxiety Treatments guidelines for neurostimulation51
Currently, electroconvulsive therapy is the most widely used neuromodulation strategy, and it is available in most hospital psychiatric settings. Guidelines recommend electroconvulsive therapy as a first-line treatment for major depressive disorder in patients with acute suicidal ideation or with psychotic features and as a second-line treatment for major depressive disorder resistant to pharmacotherapy (Table 3).51 Electroconvulsive therapy should also be considered for patients who do not have access to transcranial magnetic stimulation or whose condition does not respond to it.
Transcranial magnetic stimulation is available in most academic centres and in a small, but growing, number of community clinics. It may be used either as an add-on treatment to medication or as a stand-alone alternative for patients who decline or do not tolerate medication; it may be a good option for patients whose condition has proven refractory to initial trials of medication.
Deep brain stimulation is reserved for patients who meet the criteria for severe and intractable major depression and whose condition has failed to respond to at least 4 different treatments, including appropriate trials of antidepressant medication, evidence-based psychotherapy and electroconvulsive therapy.52–54 Currently, patients who meet these or other similarly rigorous criteria can be referred for assessment to selected centres with a multidisciplinary psychiatric surgery team. In Canada, deep brain stimulation for major depressive disorder has largely been undertaken within clinical trials, but it may be offered as an off-label procedure in select cases.
Key pointsMajor depressive disorder is often refractory to standard pharmacologic treatment but may respond well to neuromodulation.
Transcranial magnetic stimulation is least invasive but is less effective than electroconvulsive therapy or deep brain stimulation for treatment of major depression.
The acceptability and tolerability of electroconvulsive therapy is hampered by adverse effects on episodic memory and other forms of cognition.
Neuromodulation can lead to major long-term improvements in depression ratings and quality of life.
Footnotes
Competing interests: See end of article.
This article has been peer reviewed.
Competing interests: Jonathan Downar has received a travel stipend from Lundbeck. Sidney Kennedy has received grants from Bristol-Myers Squibb and Clera. He has received grants and personal fees from Lundbeck, Servier and St. Jude Medical, and personal fees from Eli Lilly, Pfizer, Abbott Laboratories, AstraZeneca, Elsevier, Glia Communications, Indegene Lifesystems, Spimaco, Symbiote Medical Communications Inc. and Spirant Communications. Andres Lozano has received personal fees from Functional Neuroscience and is a consultant for Ceregene, Medtronic, Boston Scientific and St. Jude Medical. Peter Giacobbe is a consultant for St. Jude Medical and has received personal fees from Eli Lily Canada, Bristol-Myers Squibb, AstraZeneca and Pfizer. He holds grants from the Michael J. Fox Foundation for Parkinson’s Research, National Institutes of Health and the Schizophrenia Society of Ontario. No competing interests declared by Nir Lipsman or Tejas Sankar.
Contributors: Nir Lipsman and Peter Giacobbe conceived the article. All of the authors contributed to writing and revising the manuscript and approved the final version submitted for publication.